On the third floor of The Research Institute of St. Joe’s Hamilton, Dr. David Bulir is in a constant war to find pieces of plastic roughly the size of a pinky finger: pipette tips.

They are ubiquitous in labs around the world. Scientists and lab technologists use them to transfer miniscule volumes of liquid.
But amid the ongoing pandemic that has infected over 40 million people, including over 200,000 Canadians, they are critical to conducting novel coronavirus tests. Without them, the tests can’t be completed.
“I never would have thought in a million years I would be trying to find pipette tips from any supplier that I can,” said Bulir, also a researcher from McMaster University. “There is just a demand for every single thing that a lab uses to function right now.”

Everything from plastic transfer tips to tubes to gloves have become so difficult to obtain that the lab at St. Joe’s converted an old office into a secret storage room to ensure they have enough supplies to carry out the next round of coronavirus tests.
But even his secret stockpile is only large enough to last two weeks.

“The fact that we even have to lock up our supplies and gloves and keep them in an area so that other people don’t know about it… it’s unbelievable, is all I can say,” Bulir said.
The supply crunch in Bulir’s lab is similar to the situation in dozens of other Canadian labs that are struggling to keep up with the demands for coronavirus testing. Most are facing backlogs in processing test results amid a second wave of COVID-19, the disease caused by the virus.
READ MORE: Ontario training hundreds of lab workers to deal with testing backlog. But is it enough?
More than half a dozen physicians and researchers told Global News that labs in Ontario and Quebec continue to face a crisis despite the early warnings and experience from the first wave of the COVID-19 pandemic in the spring.
Their concerns were backed up by key provincial health documents, obtained by Global News.
Doctors who spoke with Global News acknowledged that the labs are processing more tests than ever before, but say that Canada desperately needs its own domestic supply of these vital medical components as a long-term solution.
“If we don’t have our own secure supply chain, then we’re going to be toast,” Bulir said. “It’s disheartening that these extra pressures are added on top of actually just needing to do the testing.
“I don’t know how or when this is actually going to change,” he said. “I don’t see a light at the end of the tunnel to say that this problem is going to be fixed any time soon.”

Dr. Jerry Zaharatos, chief of medical microbiology at the McGill University Health Centre and the Jewish General Hospital, likened the problem to a game of Jenga: one missing piece, like a plastic tube or plate, can bring testing at a lab to a halt.

Get breaking National news
“It’s that one piece at the bottom of the tower. If you pull it out, the whole tower collapses,” Zaharatos said. “That is what we are living on a daily basis right now. I’m going into work or I’m actually picking up my phone in the morning, dreading what text I’m going to get next from which lab manager about what’s happened, what didn’t get delivered, what got blocked at the border or was lost.
“We are feeling like we’re at the precipice day to day, week to week,” he said. “I want to run out of the building screaming. (Some of) our laboratory technologists are having moments where they have to stop and cry.”
While diminished supplies of reagents — the specific chemicals needed by laboratories to complete the tests — or swabs have often received attention from public health officials in the past, little attention has been paid to the vital medical plastics that are in short supply.
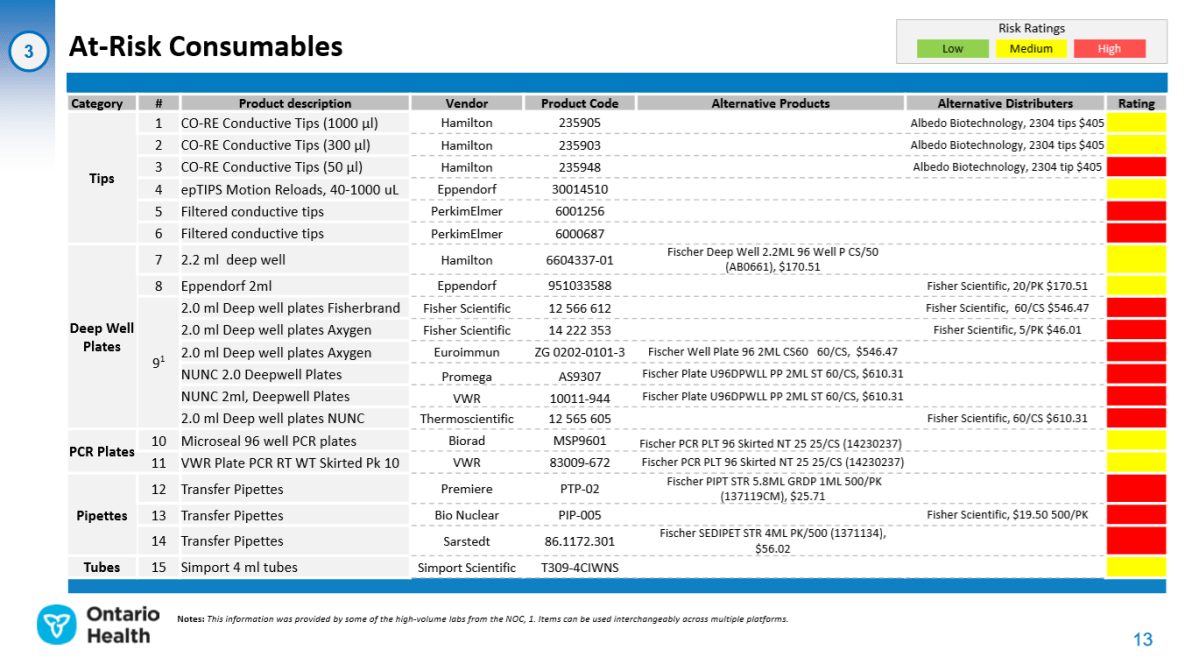
An internal document from Ontario Health revealed 15 different “consumables”, like plastic tubes or plates, that are at a “high” or “medium risk” of running out. The ministry sent the list to the “COVID-19 Provincial Diagnostic Network” on Oct. 15. The network is a group which includes Sunnybrook, Mount Sinai, and private companies, like LifeLabs and Dynacare.
“Laboratories in the network have (begun) experiencing shortages as result of increased testing,” the document said. “This has required laboratories to borrow from each other, look for alternative suppliers and assess replacements.
“Fifteen products across five categories (tips, deep well plates, PCR plates, transfer pipettes and tubes) were identified as immediately at-risk of having a shortage.”
Global News contacted all the companies listed in the document for comment on the difficulties suppliers are facing obtaining products from overseas. Only one company responded.
Surender Choudhry, president of Bio Nuclear Diagnostics Inc. based in Toronto, said increased demand for COVID-19 testing products in the U.S. has caused prices for things like transfer pipettes to skyrocket, forcing him to back to more complicated supply chains in Asia.
“We’re trying to meet I would say about 70-75 per cent demand, but I still cannot keep up,” Choudhry said.
READ MORE: Ontario reports 704 new coronavirus cases, majority in Toronto, Ottawa, Peel and York regions
He said he’s begun working with a company in China to procure transfer pipettes and the shortage “will be taken care within the next two weeks.”
Meanwhile, at the Shared Hospital Lab whose members include North York General and Michael Garron hospitals, Sunnybrook Health Sciences Centre and Scarborough Health Network, its medical director, Dr. Kevin Katz, said for “the moment” his lab has enough supplies, but that could change in an instant.
“The whole world wants to do the exact same thing in very high volumes at the same time,” he said, adding that wait times for some important molecular analyzing machines have gone from days to six months.
Video from inside his lab shows pallets of supplies stacked from floor to ceiling. But as some distribution companies have moved to a rationing system, the lab often shares with others across the province in case of a shortage, making stacks of tubes, plates and other supplies seem small.
“We have a storage room where we’ve stockpiled some of the really critical pieces so that we don’t run dry,” Katz said.

The supply shortage hasn’t just affected the clinical labs doing the COVID-19 testing. It’s also slowed research at universities conducting important studies to help better understand the constantly mutating virus.
“There’s been this huge bottleneck where nobody can get the resources that they need to do the experiments,” said Dawn Bowdish, a McMaster professor of pathology and molecular medicine and the Canada Research Chair in Aging Immunity, who is currently studying how the virus spreads and who is most at risk.
“It’s been challenging to do any research.”
As more and more critical supplies and personnel have been directed towards clinical testing including swabs and testing agents, Bowdish said research across the country — in which the federal government has invested more than $1 billion — has been “really impaired.”
READ MORE: Massive coronavirus test wait times not a sign of ‘good testing regime
She said Canada needs to invest in making critical supplies here at home the same way other industries have shifted towards manufacturing ventilators and personal protective equipment like face shields.
“It’s always been cheaper and easier to buy them from someplace else,” she said. “I think one of the important learning tools that certainly we are coming to terms with now is the fact that we have to manage these essential ingredients at home.”

Health Canada said the federal government has worked with a “variety of companies” to secure domestic sources of the chemicals and plastic consumables necessary to support federal and provincial labs.
The agency pointed to contracts signed with GL Chemtec to manufacture guanidine thiocyanate “a key chemical required for COVID testing” and a $16-million contract with Plastiques Moore, a company based in Quebec, to produce plastic consumables used in the testing process.
“The Government continues to pursue sourcing opportunities from traditional suppliers and is working with domestic firms who have retooled to bolster domestic capacity for key inputs that were in global shortage, for example swabs and reagents,” Eric Morisette said in an email.
“Canada is supporting provinces and territories by providing $4.28 billion in funding to help them augment their testing, contact tracing and data management capacity.”
Ontario Health, meanwhile, said there is a global shortage of certain reagents, required for diagnostic equipment used by labs in the lab network, and that although “some labs in the network have experienced shortages in pipette tips” it has not “impacted testing capacity.”
“To help make up for the loss in capacity from Roche, labs impacted by this shortage are bringing in other diagnostic equipment for testing,” a spokesperson said in a statement. “Other labs within the network have been able to share pipette tips from their own stock until the lab experiencing the shortage receives their next delivery.”
READ MORE: Global coronavirus cases pass 40 million as nations struggle with 2nd wave
Quebec’s Ministère de la Santé et des Services Sociaux said the province is facing a “global shortage” of plastic consumables.“A team is dedicated to finding these products from all suppliers in order to obtain and guarantee a sustainable supply,” said spokesperson Marjorie Larouche in an email.
She said the province is in close contact with suppliers in order to obtain “the maximum supply” for COVID-19 and has set up “provincial reserve” in anticipation of the second wave, but did not provide further details.
“(Quebec]) works in collaboration with the federal government to ensure that the materials, equipment and reagents required for the complete process of the COVID-19 analysis are distributed equitably among the provinces,” she said.
Dr. Bulir and Zaharatos are calling on governments to make supply chains more transparent and say that far more needs to be done to shore up Canada’s lack of testing supplies.
“We’ve never seen anything like this in our lifetime,” Zaharatos said. “Understanding (supply chains) in a really granular way and what the issues are that has to be on the top of the agenda right now.”












Comments
Want to discuss? Please read our Commenting Policy first.