It was late in the spring and a former drug user was feeling desperate.

She had been sober for more than a decade, but now faced a relapse under the pressure of coronavirus lockdowns.
This type of story is becoming all too common for front-line workers who say they are struggling to keep up with rising demand.
“This one particular individual came in and said it ruined 12 years of sobriety for them,” said Amanda Sauer, the education co-ordinator for AIDS Program South Saskatchewan (APSS).
Sauer’s program offers support services, including a needle exchange for people living with HIV/AIDS or who are at risk of contracting diseases from contaminated needles.
Lately, this has been a tough job, Sauer said.
“It’s hard. We just want to be able to help everyone as best we can,” she told Global News. “I wish we could do more, I really do.”
In the case of the woman seeking help, Sauer said they reassured her that she wasn’t alone and offered help and supplies to keep her safe.
Halfway through 2020, APSS says it has already handed out 873 naloxone kits, which are used to treat an overdose. In all of 2019, the organization said it only distributed 357 kits.
But Sauer said she knows there are many more people relapsing after years of hard work. To make matters worse, this was all happening at a time when APSS had scaled back some of its services to comply with COVID-19 public health orders.
“It’s heartbreaking,” she said. “We’ve had clients (with) years of sobriety behind them and unfortunately this pandemic has hit, and they’ve had to break that sobriety just to get some level of comfort.”
‘They realized that they weren’t going to get help’
The situation in Regina follows a trend in some other Canadian cities as well as around the world. Front-line workers say that the coronavirus is exposing significant gaps in the existing services needed to support and treat people suffering from addictions.
There is also evidence that the pandemic is introducing additional dangers to a volatile situation.
In markets where highly-addictive opioids are becoming harder to come by, users may turn to more readily available and riskier consumption methods, such as injections, according to the United Nations Office on Drugs and Crimes.
The UN agency has been studying the impact of the coronavirus on the illegal drug supply and noted on June 25 that there are already signs that the global pandemic is triggering some shortages that result in both impurities and high prices.
Regina-area addictions counsellor Rand Teed agreed that substance use was trending up provincially in Saskatchewan, particularly among people who are out of work or doing reduced hours.
He says it’s not just the social service agencies that have been cutting their own services and that detox centres have operating bare bones.
Teed said he even had to set up out-of-province treatment options for a handful of people who could afford to pay for it.
The rest, he explained, could get stuck in a vicious circle. Even under normal circumstances, he said a month’s wait would be typical, but the situation is now more dire.

Get weekly health news
In-patient treatment for addictions only resumed in Saskatchewan on July 13, according to a press release sent out that day by the Saskatchewan Health Authority. The body runs the majority of the detox centres in the province and all of the ones in the Regina-area.
“So if you’ve got somebody with a substance use disorder who is looking for help and they get told, ‘Well you can’t get in now. You have to wait two weeks or three weeks or four weeks,’ that’s really discouraging for them,” he said in an interview.
“One of the characteristics of a substance use disorder is when you feel stressed you tend to go to that substance as a stress management tool. So the effect was people, in general, were starting to use more because they realized that they weren’t going to get help and that was scary.”
Lethal combination
The numbers show some alarming trends.
There have been 532 overdoses recorded by the Regina Police Service from the beginning of 2020 up until July 14. At least 27 of the people who overdosed died.

Regina police suspect at least some of the overdoses are linked to the same batches of fentanyl-laced drugs.
More needles on the streets
Meantime, over the past five months, the volunteers of Queen City Patrol have picked up more than 10,000 needles in outdoor public spaces throughout Regina.
The fire department, which responds to needle pick-up calls on evenings and weekends, has also noticed the high volume.
Between the beginning of the year and July 7, crews responded to 109 needle pick-up calls, said assistant chief Kevin Digney, noting in all of 2019, they responded to 133.
“There’s a lot of times where you’ll go and there’ll be hundreds of needles,” he said, adding it’s not just in specific areas of the city, either.
Queen City Patrol co-founder Wade LeCaine said the high volume of needles highlights a longstanding problem. There aren’t enough options for drug users who want to discard needles, and recent service disruptions triggered by the pandemic have made matters worse, he explained.
Mobile site immobilized
People who need to pickup or drop off drug paraphernalia are encouraged by both APSS and the health authority to do so in-person at a harm-reduction site in the city.
- Alberta rolls out activity-based surgery funding model to more public hospitals
- Saskatchewan drug traffickers can now face civil lawsuits for related damages
- Ebola cases in Congo reach 282 as Brazil investigates 2 suspected cases
- Late spring start, dry conditions to blame for intense Edmonton allergy season
In addition to APSS, drug users can exchange supplies at the Regina Qu’Appelle Health Region clinic at 2110 Hamilton St.
Both have remained open with limitations throughout the pandemic, although APSS noted some clients didn’t realize that at first.
Many users relied on another option: the Street Project van.
The mobile harm-reduction site was pulled on April 8 “and it won’t be used until a modification to its floor plan can be put into place to ensure physical distancing,” said the health authority’s media relations consultant, Lisa Thomson, in an email, adding it’s important to get it back up and running by the time the cold weather returns.
Collection curbed
Through the media, Queen City Patrol has been calling for more large public outdoor needle drop boxes, which fall under the purview of the health authority. Right now, Regina only has two needle drop boxes, compared to 24 boxes in Saskatoon.
The health authority hasn’t received any suggestions for a dropbox in any new neighbourhood or area of Regina, Thomson wrote in an email, noting that it works with “relevant stakeholders” to evaluate requests.
It wasn’t immediately clear whether Queen City Patrol was among those relevant stakeholders.
While both Regina and Saskatoon have a needle exchange rate in the high 90th percentile, according to the Saskatchewan Health Authority, the overall recovery rate in Saskatoon is much higher.
The executive director of AIDS Saskatoon, who has been leading the charge for the province’s first safe consumption site in that city, questions why Regina doesn’t have a similar setup.
“At the end of the day, if we don’t do a good job on the community cleanup, needle cleanups, it’s going to further contribute to stigma and discrimination for people who need drugs,” Jason Mercredi said in an interview with Global News.
“We need to be treating this like a health care issue.”
‘We already know that the numbers are high’
Margaret Kisikaw Pyesis, CEO of the All Nations Hope Network, said she has been concerned about what this could all mean for the transmission of HIV and other blood-borne infections.
The Saskatchewan Ministry of Health’s 2018 HIV Prevention and Control Report contains the most recent publicly available data on intravenous drug use and the transmission of the blood-borne infection. Of the new cases reported that year, 71 per cent were in people who had injected.
“We already know that the numbers are high because of the people that walk through our doors and we talk as community agencies about what we’re seeing,” Kisikaw Pyesis said.
“It’s not getting any better. It’s getting worse.”
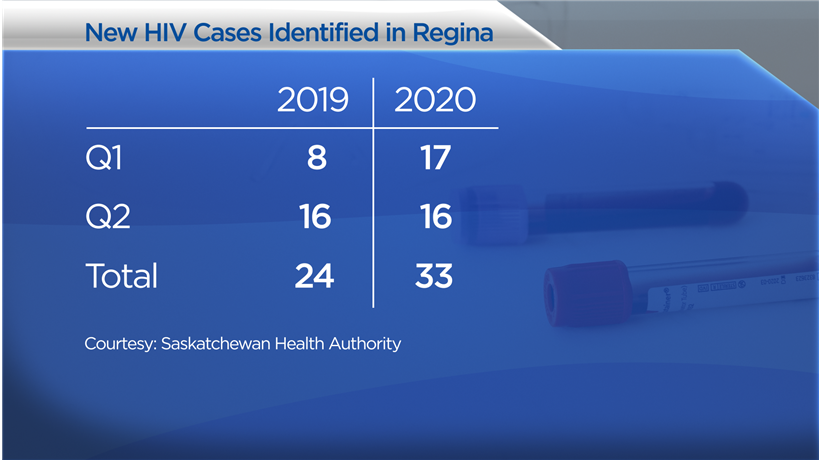
The Saskatchewan Health Authority’s data shows 33 new cases of HIV were identified in Regina in the first half of 2020 compared to 24 in the first half of 2019.
Thomson, the health authority’s spokesperson, told Global News in her email that “generally, there wasn’t notable difference in cases seen between the first and second quarters of 2020.” She also noted a decrease in testing.
“We need to do something because this can’t go on. It’s ridiculous,” Kisikaw Pyesis said.
“It’s not just the frontline community organizations that are mandated to work with HIV and harm reduction,” said Kisikaw Pyesis, from the All Nations Hope Network. “It’s the mandate of everybody.”









Comments
Want to discuss? Please read our Commenting Policy first.