A controversial proposal to give free drugs to users is among the topics that will be heard at a forum on possible solutions to B.C.’s overdose crisis on Friday.

Health experts, police, government officials and stakeholders are meeting for the third annual Overdose Action Exchange, a roundtable designed to brainstorm “out of the box” policies to help stem the tide of deaths caused by fentanyl and street drugs.
LISTEN: Brainstorming solutions to the overdose crisis
The meeting is scheduled a day after the BC Coroners Service released its latest data on illicit drug deaths in the province, reporting 124 suspected fatal overdoses in April and bringing the 2018 death toll to at least 511. Drug overdoses killed more than 1,400 people in B.C. last year.
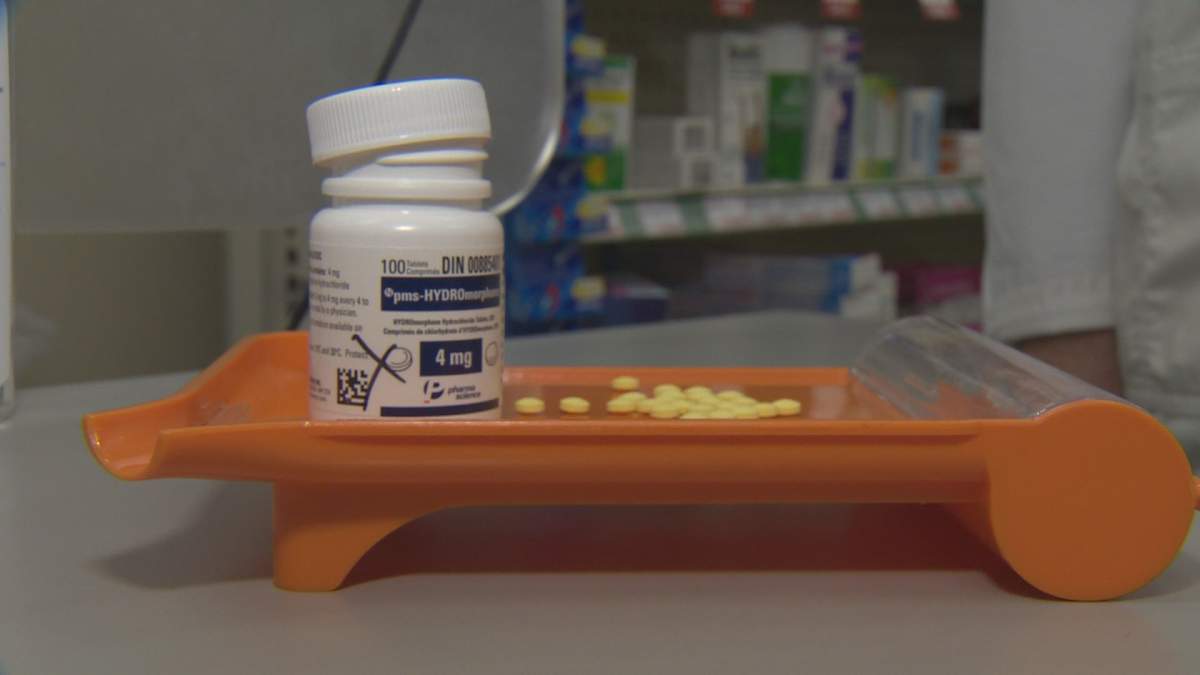
The BC Centre for Disease Control (BC CDC) has proposed a pilot project involving automated “vending machines” that would dispense hydromorphone tablets, better known as dilaudid, to drug users. The centre’s executive director said it’s one of the more aggressive harm reduction models that will be discussed on Friday.
Hydromorphone is a pharmaceutical-grade opioid that’s five times as strong as morphine.
“We’re at a point now where the drug supply is so toxic that we’re really talking seriously about how to get people access to a safer supply of drugs and that’s a direction we’re going right now,” Dr. Mark Tyndall told CKNW’s The Jon McComb Show.
WATCH: BC CDC proposed drug vending machines

The idea is controversial, with critics charging that the move amounts to a government sanction of drug use, and that it removes personal responsibility from the equation.
Other critics such as Dr. Launette Rieb with UBC’s Department of Family Practice have warned that unsupervised hydromorphone use carries its own risks and can still result in overdoses, or help others become addicted to drugs.
But Tyndall argues the medical evidence is in, and that the proposal is one of the best ways to stop people from dying so that they can then seek treatment.

Get weekly health news
He said therapy with products like methadone and suboxone have their place, but that many hard-core drug users simply aren’t ready to use them.
“Certainly it helps people take away their drug cravings, but it does not address the many problems that people are using drugs in the first place for, and so people will continue to use drugs,” he said.
“We’ve come to the conclusion that most of the drugs people are purchasing illegally are very toxic and they have a high chance of overdosing, so I think it’s just a logical next step that we, as a first step, to connect with people, we try to offer them the drugs that they’re seeking right now, and then we’ll have time to work on substitution therapy and other treatments.”
Tyndall pointed to the pilot project at Vancouver’s Crosstown Clinic which has been offering hydromorphone injections to people with serious addiction issues, and which has been successful at keeping those people away from fentanyl-tainted drugs.
READ MORE: Vancouver drug users will now be able to test their drugs for fentanyl
“Many people don’t want to go three times a day to a medical facility to inject drugs so the next logical step is to try to get people access to hydromorphone pills.”
Tyndall said the machines can be equipped with biometric sensors to ensure only users registered in the pilot have access to the drugs, and that the pilot could be rapidly scaled up in areas most affected by the overdose crisis.
WATCH: Heartbreaking stories on the opioid crisis at national pharmacist conference

Tyndall acknowledged that the idea of giving drugs to users won’t sit well with many people, but said he believes that attitudes are slowly shifting.
And he argued that other alternatives, such as police crackdowns, have failed.
“We know also that it’s just not a deterrent. I’ve never met anyone that’s using that’s deterred because of law enforcement.”
READ MORE: Free naloxone kits now available at 220 pharmacies throughout B.C.
Under the proposed pilot project, the vending machines would be installed at existing harm reduction sites or health facilities.
The BC CDC has yet to reveal details on how many or which sites the machines could potentially be placed in, when the pilot project might begin, or how drug users would qualify for it.











Comments
Comments closed.
Due to the sensitive and/or legal subject matter of some of the content on globalnews.ca, we reserve the ability to disable comments from time to time.
Please see our Commenting Policy for more.