Residents of London-Middlesex who identify as members of the region’s visible minority population have been disproportionately impacted by COVID-19, new data from the Middlesex-London Health Unit (MLHU) shows.

Despite making up 17 per cent of the region’s overall population as of the last census, the data shows people who identify as a visible minority account for more than 30 per cent of all cases reported between Jan. 24 and Oct. 31.
The figures are outlined in a new report going before members of the region’s board of health on Thursday which details the race and socio-economic data collected by MLHU from confirmed cases over the last several months.
Local health officials began collecting such data voluntarily from lab confirmed cases in April, months before the province made collection of the data mandatory in late June. The report presents this data up until the end of October.
Under the Employment Equity Act, the health unit says a visible minority is defined as “persons, other than Indigenous peoples, who are non-white in race or colour.”
The health unit found that 10 per cent of all cases reported between January and October self-identified as Asian South, while 6.7 per cent identified as Middle Eastern, and 4.8 per cent identified as Latin American.
White residents, who accounted for roughly 82.9 per cent of the region’s population in 2016, made up about 46.5 per cent of cases reported in the time period analyzed.
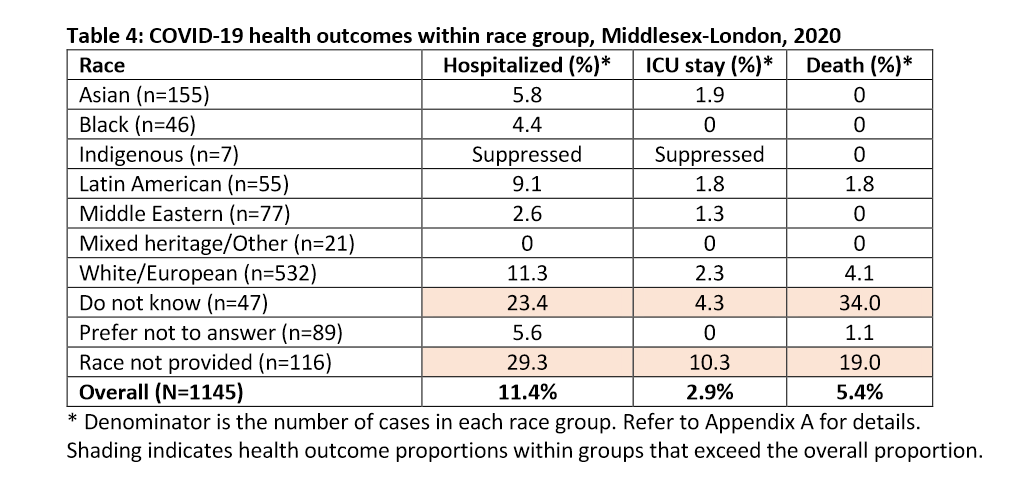
The health unit also found that people who self-identified as Latin American (55 in total) were slightly more likely to be hospitalized due to COVID-19 compared to other visible minority groups.
According to the health unit, 9.1 per cent of cases involving people who self-identified as Latin American were hospitalized, compared to 5.8 per cent for those identifying as Asian, and 4.4 per cent for those identifying as Black. For white residents, the percentage was 11.3.
Similar hospitalization data was not available for those who identified as Indigenous because of small case counts, the report says.
The health unit said roughly 10.1 per cent of all cases (116 cases) did not have race data, 7.8 per cent (89) chose not to answer, while 4.6 per cent (47) told health officials they did not know their race.
For reasons not outlined, the percentage of hospitalizations/deaths reported among cases without race data, and those who did not know their race, is notably high — 29.3 per cent/19 per cent, and 23.4 per cent/34 per cent, respectively — compared to the regional average of 11.4 per cent/5.4 per cent.

Get weekly health news
“Limitations of the data available, including the small number of cases within racial groups as well as the number of cases without race data provided, made meaningful comparisons between groups difficult,” the report says.
Data was also collected for other indicators including household size, language, occupation, Indigenous identity, and whether the person was homeless or underhoused, according to the report, which noted that six cases were confirmed homeless or underhoused.
The health unit said it also collected data on household family income, however the data it gathered was limited to the point that, like with race, it made meaningful comparisons between groups difficult, the report said.
For example, some 22.7 per cent of cases said they did not know their family income, while 20.4 per cent chose not to answer.
Roughly 13.6 per cent of all cases told the health unit they made between zero and $29,999 pre-tax in 2019, while 31.7 per cent said they made $30,000 or more.
According to the health unit, families of two or more making less than $30,000 pre-tax would fall below the poverty line under the Market Basket Measure — a population group which was 15 per cent locally in 2015.
- Toronto library, UHN offer mobile health clinic to reach most vulnerable
- Alberta rolls out activity-based surgery funding model to more public hospitals
- Saskatchewan drug traffickers can now face civil lawsuits for related damages
- Ebola cases in Congo reach 282 as Brazil investigates 2 suspected cases
Looking at age, the health unit found the mean age of cases in London-Middlesex stood at 44, while in their 20s accounted for the largest number of cases.
The report found that severe COVID-19 outcomes — hospitalizations, ICU stays, or death — disproportionately impacted those in older age groups, such as those 50 or older.
The percentage of hospitalizations has been particularly high among people in their 70s — 47 per cent of cases in that age group compared to 36.4 per cent for those 80 or older, and 19.1 per cent for those in their 60s.
People 80 or older, however, had nearly twice as many deaths as those in their 70s — 33 per cent to 18.2 per cent. Roughly six per cent of those in their 60s died.
The regional average stands at 11.4 per cent for hospitalizations and 5.4 per cent for deaths.
The mean age for an ICU stay stands at 65, while the mean age for hospitalization was 69, the report says. The mean age of those for whom COVID-19 was found to be the primary case of death was 82.
“The COVID-19 pandemic has exposed and exacerbated existing health inequities, highlighting the need to prioritize the collection of health equity information to assess and modify our response to health crises and protect the health of all individuals,” the report concludes.
“The findings included in this report suggest that inequities exist related to who is infected and experiencing severe outcomes related to COVID-19 infection. These findings should inform MLHU’s COVID-19 response and priorities as the pandemic continues.”
With some data incomplete, the health unit says its vital that it continue collecting health equity data to better understand disparities among different groups.
“Additional data will especially help clarify the relationships between race and income with COVID-19 infection. Overall, health equity considerations should be included in pandemic planning, response, recovery, and beyond.”
The report adds it may also be worth considering collecting such information “across all MLHU’s public health programs and services, where the capacity to do so exists.”
The full report, which will be presented to the board of health on Thursday, can be found here.



















Comments
Want to discuss? Please read our Commenting Policy first.