Researchers in London, Ont., have begun testing a new non-invasive ventilation mask that aims to reduce the risk of spreading the novel coronavirus during treatment while lessening the demand for invasive ventilators.

The effort is being led by the Lawson Health Research Institute, London Health Sciences Centre (LHSC), University Health Network (UHN) and General Dynamics Land Systems-Canada.
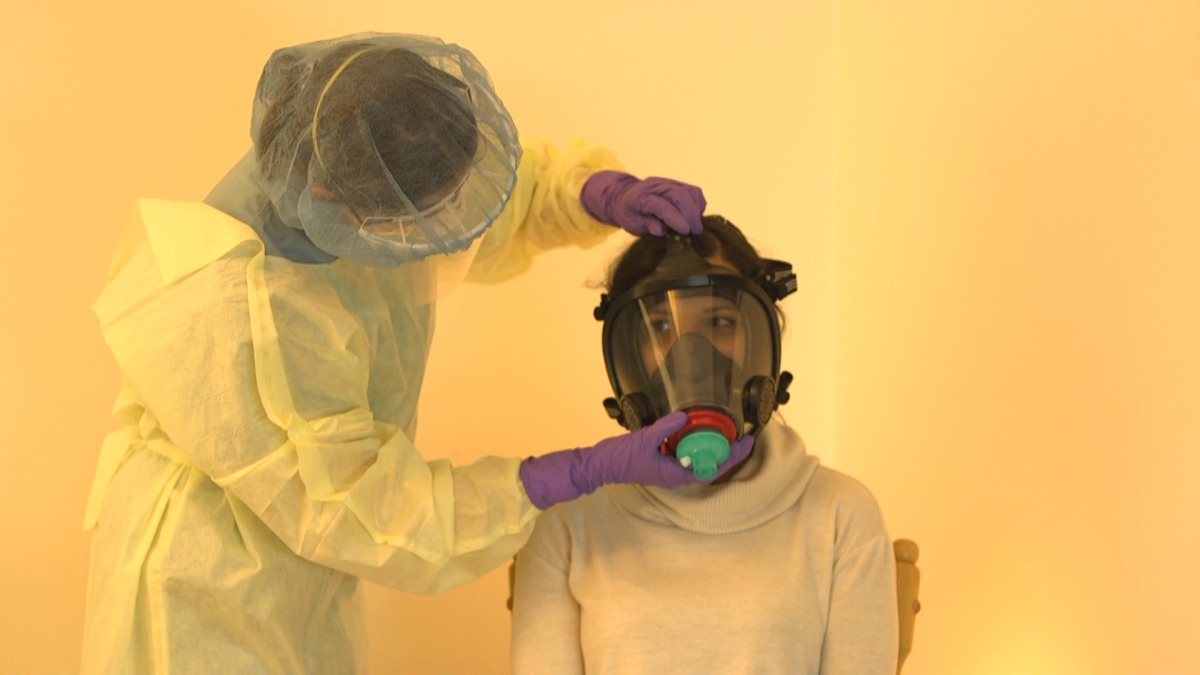
It centres around a mask that was created by modifying a standard firefighter’s mask through 3D printing. The mask can be attached to non-invasive ventilators such as a CPAP machine or a BiPAP machine.
Once fitted, the mask creates tight seals around the patient’s mouth and nose, allowing them to breathe in and out of a filter that captures any viral particles before they are released into the air.
The mask also carries the potential to reduce aerosolization when treating patients with COVID-19. Aerosolization refers to the production of airborne respiratory droplets that may contain viruses or bacteria. The inhalation of these droplets is how coronavirus is commonly spread.

Get weekly health news
The reduction in aerosolization also reduces the transmission risk associated with non-invasive ventilators such as CPAP and BiPAP machines.
The mask aims to respond to concerns surrounding ventilator shortages by bringing these sidelined machines back into the fight against COVID-19.
“There are countless CPAP and BiPAP machines idling around the world while all resources go towards invasive ventilation,” said Dr. Azad Mashari, a developer of the device and an anesthesiologist at UHN’s Peter Munk Cardiac Centre.
“Our mask aims to put these machines back into the clinician’s toolkit.”
According to a release from Lawson, a clinical trial is now underway to test the mask with up to 50 patients at LHSC’s Victoria Hospital and University Hospital.
The trial will include patients with COVID-19, asthma, chronic obstructive pulmonary disease (COPD) and congestive heart failure (CHF).
Researchers say the device can be used in emergency departments and has the potential to be used in intensive care units, remote nursing stations and during pre-hospital transport.
They add it has also been designed for easy production in resource-strained locations.
“This problem affects everyone and it’s critical that we all do what we can to help,” said Dr. Tarek Loubani, another developer of the device and a London-based physician who has previously worked to create affordable health-care tools.
“We hope it will help not only those in urban centres like Toronto and London but people in remote communities around the world.”

Questions about COVID-19? Here are some things you need to know:
Symptoms can include fever, cough and difficulty breathing — very similar to a cold or flu. Some people can develop a more severe illness. People most at risk of this include older adults and people with severe chronic medical conditions like heart, lung or kidney disease. If you develop symptoms, contact public health authorities.
To prevent the virus from spreading, experts recommend frequent handwashing and coughing into your sleeve. They also recommend minimizing contact with others, staying home as much as possible and maintaining a distance of two metres from other people if you go out.
For full COVID-19 coverage from Global News, click here.













Comments
Want to discuss? Please read our Commenting Policy first.