Canadians who need medically necessary surgeries waited longer than ever for treatment — with average wait times hitting 20 weeks, a new Fraser Institute report concludes.

Before the 20-week record in 2016, wait times were longest in 2011 at 19 weeks, according to the organization. It began recording wait times for medically necessary elective treatments in 1993. At that point, wait times were only about 9.3 weeks to see a specialist, such as an ophthalmologist, gynecologist, and general surgeons.
READ MORE: Medical wait times in Canada longer than ever at 20 weeks in 2016
“Excessively long wait times remain a defining characteristic of Canada’s health-care system, but this year is the longest we’ve ever seen and that should trouble all Canadians,” Bacchus Barua, senior economist at the institute, said.
“Long wait times aren’t simply minor inconveniences, they can result in increased suffering for patients, lost productivity at work, a decreased quality of life, and in the worst cases, disability or death,” Barua said.
READ MORE: Here’s how long Canadians are waiting for surgery across the country

Right now, Canadians are waiting for nearly one million medically necessary procedures, the institute warned. Doctors polled for the report conceded that they thought their patients were waiting more than three weeks longer for treatment after seeing a specialist than what they consider to be “clinically reasonable.”
- Trudeau tight-lipped on potential U.S. TikTok ban as key bill passes
- Canadian man dies during Texas Ironman event. Her widow wants answers as to why
- Hundreds mourn 16-year-old Halifax homicide victim: ‘The youth are feeling it’
- On the ‘frontline’: Toronto-area residents hiring security firms to fight auto theft
Here’s a look at the report’s findings:
Q: How long are wait times for various procedures?
National wait times were the longest for neurosurgery at 46.9 weeks and shortest for access to a medical oncologist and at only 3.7 weeks.
READ MORE: Patients in Nova Scotia, New Brunswick face longest wait for medically necessary surgery
Twelve medical specialties were considered in the report, spanning from orthopedic surgery to plastic surgery. The wait times below factor in how long it took to see a specialist after being referred to by a doctor and, subsequently, how long it took to receive a procedure.
Wait times (in weeks) by procedure in 2016:
Plastic surgery: 25.9
Gynecology: 18.8
Ophthalmology: 28.5
Otolaryngology: 22.7
General surgery: 12.1
Neurosurgery: 46.9
Orthopedic surgery: 38.0
Cardiovascular: 8.4
Urology: 16.2
Internal Medicine: 12.9
Radiation Oncology: 4.1
Medical Oncology: 3.7
The average wait time across the board sat at 20 weeks in 2016.
Question: How long are wait times by province?
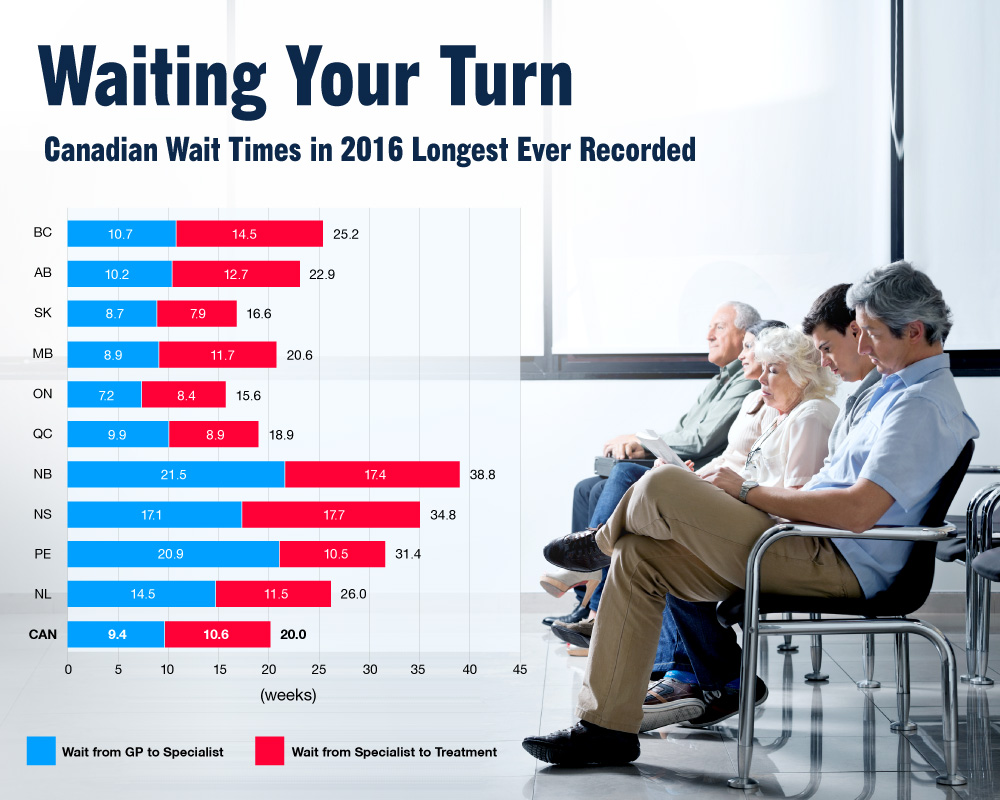
Ontario had the shortest wait times at 15.6 weeks, but up from 14.2 weeks in 2015. New Brunswick saw the longest wait times at nearly 39 weeks in Canada.
READ MORE: Why wait times for psychiatrists vary depending on where you live
For the fourth year in a row, B.C. saw an increase in wait times — there, west coast Canadians wait for about 25.2 weeks — the longest the province has ever recorded.
Wait times (in weeks) by province in 2016
British Columbia: 25.2
Alberta: 22.9
Saskatchewan: 16.6
Manitoba: 20.6
Ontario: 15.6
Quebec: 18.9
New Brunswick: 38.8
Nova Scotia: 34.8
P.E.I.: 31.4
Newfoundland and Labrador: 26.0
Question: Why are wait times so long?
The Canadian Medical Association, which represents the country’s doctors, said that long wait times are “usually a symptom of poor health system performance or poor coordination between systems that need to be addressed.”
“Alternate-level-of-care (ALC) is a key example where patients (the majority of whom are seniors) occupy acute care hospital beds while waiting for more appropriate care such as at home, in the community or in residential settings,” a spokesman said in a statement.
“This is why the CMA is calling on governments to prioritize seniors care,” the statement read.
READ MORE: Medical wait times have nearly doubled in the last 20 years
John Sinclair, president of Novari Health, said he’s not surprised by the wait times recorded in the new paper. The Kingston, Ont.-based organization helps with wait list management, e-referrals and patient intake.
He said the trouble occurs when patients are handed off from family doctor to specialist.
“One of the most dangerous times for patients is transition of care, when one provider — hospital, clinic, doctor — passes a case to another provider. Referrals can get lost, information can get misplaced and bad outcomes come from that,” he said.
“Canada has spent billions of dollars to try to bring down wait times for more than 10 years, and the outcome has been mediocre at best compared to other similar Western industrialized countries.”
When patients get referred by their general practitioner, their doctor is in the dark about how long wait times may be on the other end. Patients could wait weeks then follow up with their GP to see if a specialist will be in touch.
Some provinces, Ontario and Manitoba, for example, have worked on transitioning to online tools to make the transition seamless and transparent for doctors, specialists and patients. Otherwise, doctors’ offices are relying on fax machines and outdated equipment, Sinclair said.
Question: Why are critics challenging this report’s findings?
The report is based on survey responses from physicians across the country. It zeroed in on 12 medical specialties that patients are referred to by their family doctor.
Only 21 per cent of doctors responded to the survey results.
Sinclair said this is a “small sample,” and not necessarily representative of the entire country. Keep in mind, it could be time-strapped doctors frustrated with the wait times they’re grappling with that responded, too.
The methodology is “questionable,” but it points to a general message: that wait times are too lengthy in Canada and that health officials need to carve out some reprieve.
Federal Health Minister Jane Philpott told Global News not to put so much weight into the study because of its methodology.
Question: How do the Fraser Institute’s findings compare to other organizations’ reports on wait times?
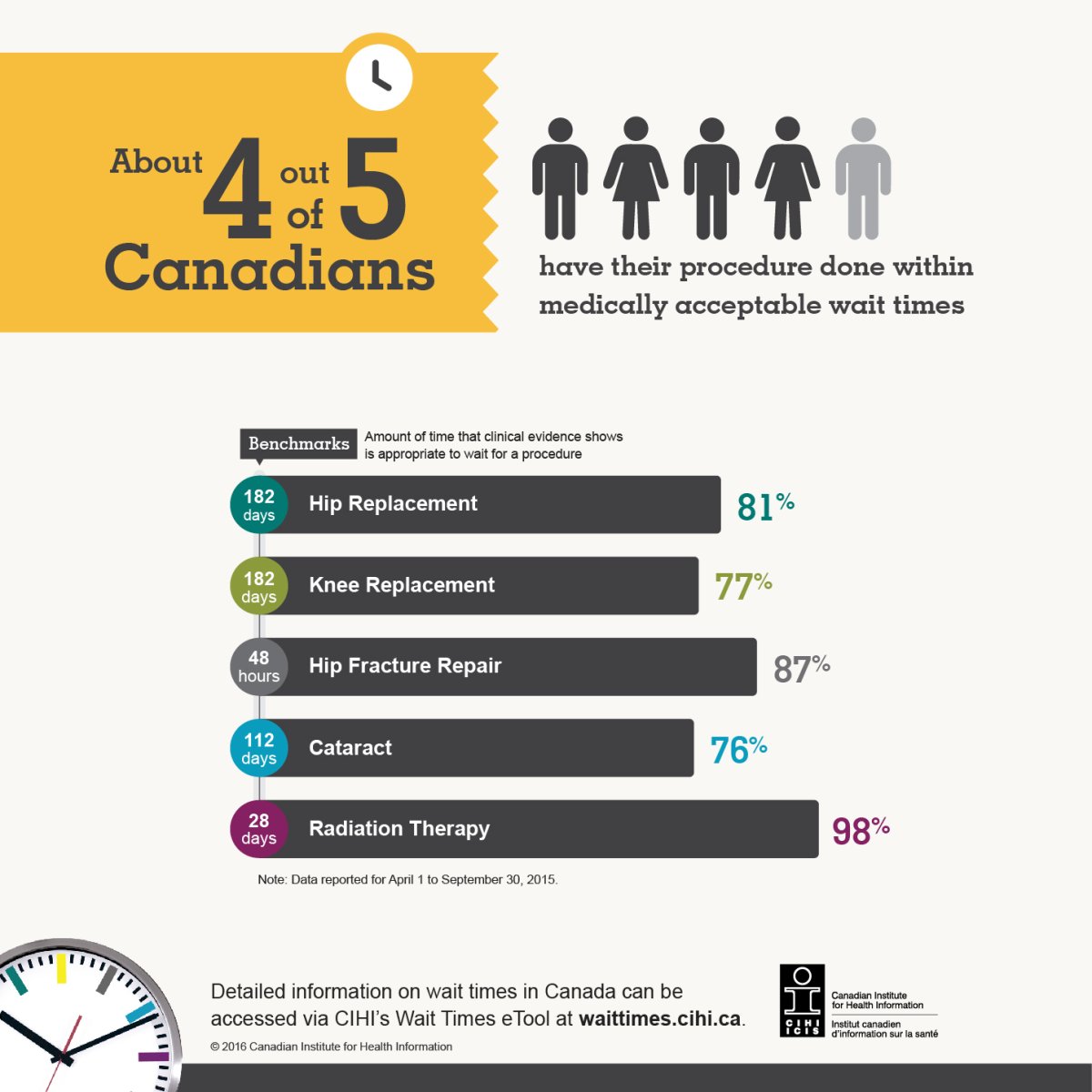
The Canadian Institute for Health Information says that more surgeries are being performed in Canada but wait times haven’t budged.
Overall, about eight in 10 Canadians going under the knife waited for their surgeries within established benchmarks. The CIHI data suggests that Canada has the shortest wait times for cataract surgery and the second-shortest wait times for hip and knee replacements.
CIHI reports that one in four ‘older’ Canadians waited at least 2 months to see a specialist.
Question: What are the implications for the Canadian economy and for the everyday patient?
The Fraser Institute points to research that suggests that the estimated cost of waiting per patient in Canada is roughly $1,305 if only hours during the normal working week are considered “lost.”
If Canadians counted all hours of the week, excluding eight hours of sleep per night, they’re losing about $3,951. This accounts for time off work, acting as a family caregiver, pain relief and other expenses tied to pain management.
“This is expensive for our economy and has personal consequences for individuals. We all end up as patients, not one of us can avoid the health care system,” Sinclair said.
Read the full Fraser Institute report here.
carmen.chai@globalnews.ca




Comments