Petra Schulz’ son Danny was a chef working in one of the best restaurants in Edmonton and was on the road to recovery from an addiction to heroine when one day of relapse became his last.

“He went to work on the day he died. He died after work. He had relapsed, took one more pill, and at the time, fentanyl was just emerging,” Schulz said.
The grief of losing her son prompted her to take action and connect with other parents whose children had died of opioids, eventually co-founding the now national advocacy group called Moms Stop the Harm.
Eight years later, tens of thousands more Canadians have died from drug toxicity overdoses – a total of 29,052 since 2016. And it’s a crisis that has become significantly worse in the last two years.
New data released last week by the federal government paints a grim picture of the fatal toll the opioid crisis is having on an alarming number of Canadians.
In 2021, the number of deaths reached an all-time high: 21 Canadians a day died from opioids, which represents a 162 per cent increase from 2016, and a 101 per cent increase from just the year before. A total of 7,560 Canadians lost their lives to the opioid crisis last year, up from 3,747 in 2020.

Gillian Kolla, a postdoctoral fellow at the Canadian Institute for Substance Use Research at the University of Victoria, says the sharp increase in people dying from opioids is “shocking” and should be deeply concerning to all Canadians.
“The way in which this crisis has been hitting the country and exacerbated by COVID, the tremendous amount of grief and loss that this has caused within communities, I think has really not been paid attention to by any level of government over the last three years,” Kolla said.
“It’s an urgent crisis with urgent interventions that are necessary.”
And the disturbing numbers don’t stop there.
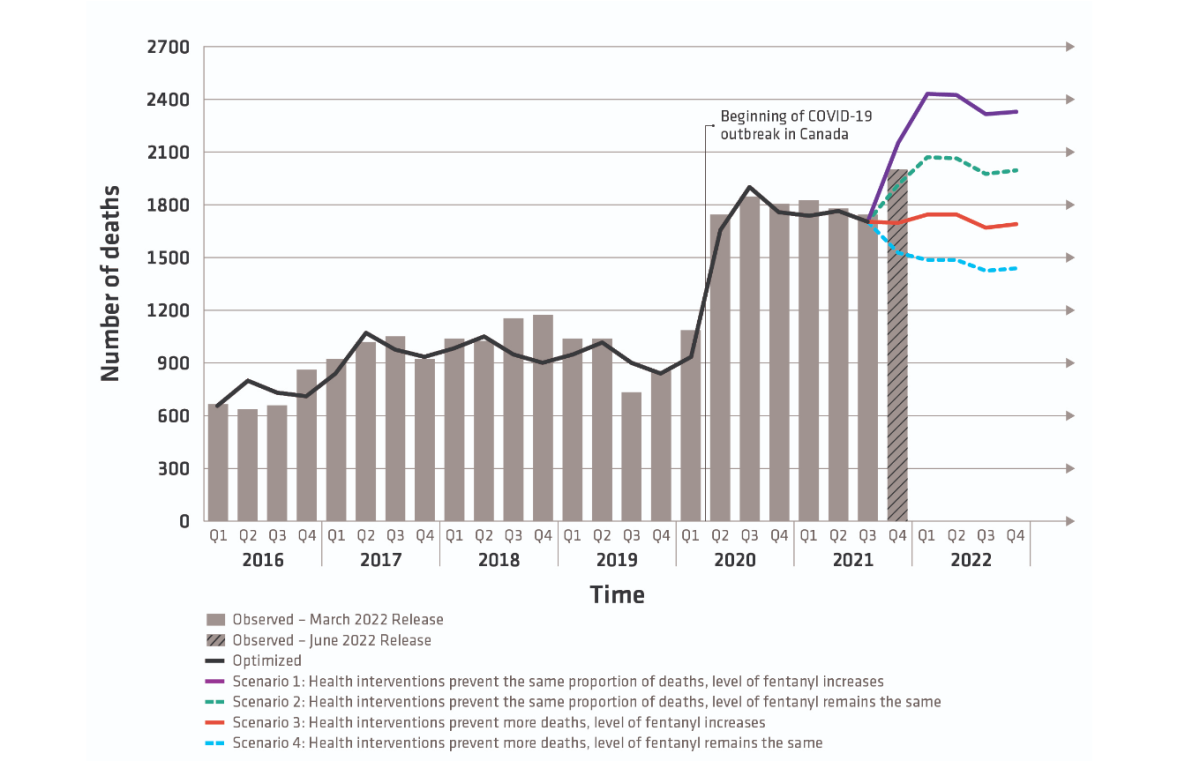
The Public Health Agency of Canada (PHAC) has also released modelling projections for the number of opioid-related deaths it believes could continue to occur for the rest of this year showing the death toll is expected to remain high – or get worse – over the next six months.
Between 1,400 and 2,400 people could lose their lives due to opioid-related harms every quarter from now until the end of this year, PHAC modelling suggests.
As part of this modelling, PHAC has included a number of different death-rate scenarios with varying outcomes, based on whether health interventions could prevent between 30 and 50 per cent of deaths and whether the level of fentanyl in the drug supply remains the same or gets worse than it was in December 2021.
But Dr. Andrea Sereda, a physician who works on street-level intervention and support programs for drug users at the London InterCommunity Health Centre in Ontario, says she takes issue with these projections.
For one thing, she says the fentanyl potency in street drugs has never gone down, but has become worse and more toxic, which makes any projections based on assumptions the toxicity of the drug supply would remain the same or get better is “incredibly naïve,” she said.
Sereda also questions why all levels of government aren’t treating the issue with more urgency when their own modelling projections predict an alarming number of deaths.
“What other thing in Canada that was killing … thousands of people per year in Canada would we be OK with only a 30 or 50 per cent reduction in mortality?” Sereda said.
“I think looking at COVID, we tried to prevent every death. And so why are we making models where the best things that we’re aiming for is maybe a 30 or 50 per cent decrease in deaths of humans in our community?”
That’s why many experts and those who work on the ground say the federal government should declare drug toxicity overdoses a national public health emergency, and take more urgent action to prevent more people from dying.
And one of the key harm reduction strategies many experts and advocates would like to see expanded in Canada is offering a safer supply of drugs.
Sereda runs a federally-funded safe-supply program at her centre in London, and she says the improvements when it first opened were immediate and eye-opening.
As part of this program, she is able to prescribe pharmaceutical-grade opioids to people who are dependent on street-level fentanyl. This means they don’t have to experience the debilitating effects of withdrawal and instead know what drug they are taking, how much they’re taking and they know where and when they can legally obtain it.
“We have seen dramatic reductions in overdoses, it dropped immediately in the first month by 50 per cent. We’ve seen huge reductions in hospitalization admissions in emergency departments. We’ve seen enormous increases in people’s physical and mental well-being. And we’ve seen decreases in criminalizing behavior like petty crime or survival sex work,” Sereda said.
“Everything gets better with a safer supply.”
Last month, federal Mental Health and Addictions Minister Carolyn Bennett spoke in favour of adopting more progressive harm reduction approaches to stop the rising death toll from toxic drug poisonings, including embracing safe supply.
“Putting in place a regulated safe supply of drugs is the real antidote to the toxicity of the present supply,” Bennett said in a news conference May 31 in British Columbia, adding that Ottawa understands it must “really accelerate the progress to safe supply.”
In a statement to Global News, Bennett’s office says the federal government is committed to “reducing barriers to providing people who use drugs with safer, pharmaceutical alternatives to the toxic illegal drug supply” and has supported 17 safer supply projects across 30 sites in British Columbia, Ontario, Quebec and New Brunswick, as well as one national community of practice – a total investment of more than $64 million.
“There is no one solution to address the overdose crisis and the government is taking a comprehensive approach,” the statement said.

But advocates and experts are united in saying they believe federal and provincial governments aren’t moving fast enough to embrace and roll out more large-scale harm reduction measures – delays that are costing lives.
Cheyenne Johnson, executive director of the B.C. Centre on Substance use, says while the federal pilot projects on safe supply are welcome, they are only reaching a small number of people in just a few targeted regions of the country.
“So there’s this large swath of the population that either have another substance use disorder or the health system isn’t reaching them, or they’re in a rural and remote area and these programs are really not reaching them, which is why we continue to see that number of overdose deaths remain very high.”
Eight years after losing her son and seeing the opioid death toll in Canada rise exponentially, Schulz says she has come to believe progressive measures like safe supply are key in trying to save the lives of people like Danny.
“I did not start out this way after my son died. I’ve slowly come to the realization that he did not die from substance use, but from poor substance use policies.”
She believes the opioid crisis should be treated as an urgent priority by all levels of government, and especially by Prime Minister Justin Trudeau.
“He should lead by example to parliamentarians and talking about the need to address this,” she said.
“We need to get this death toll under control and we need to roll out large scale safe supply models.”





Comments