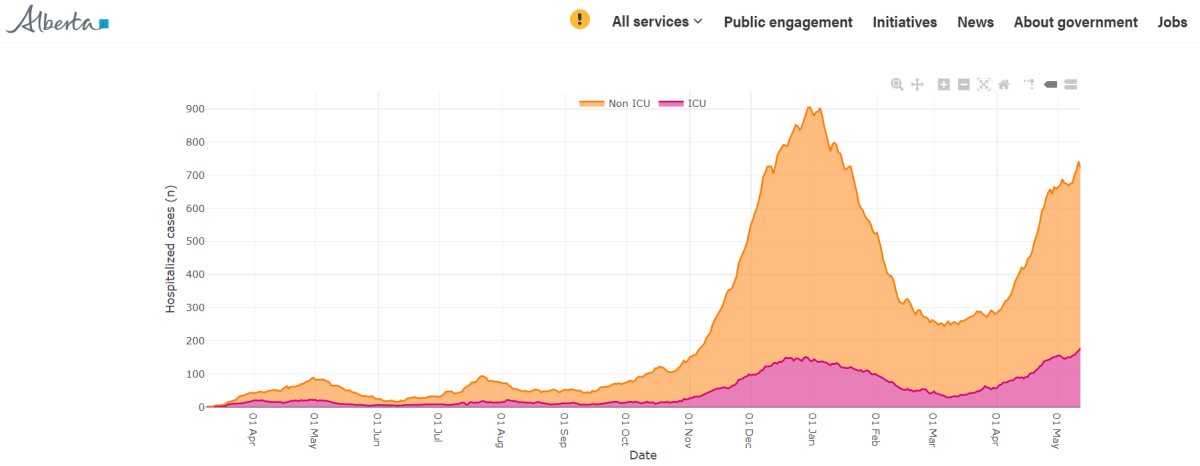
While Alberta’s general hospital admissions for COVID-19 aren’t as high as they were in December’s second wave, the number of patients requiring intensive care has never been higher.

On Dec. 29, there were 890 hospitalizations due to COVID-19, 153 of which were in ICU. On Thursday, there were 722 hospitalizations, 177 of which were ICU patients — a record high in Alberta since the pandemic began.
Read more: ‘That’s going to happen here’: Alberta physician says Ontario is ‘sending out distress signals’
Two Alberta doctors who spoke to Global News said ICU patients now are typically younger than they were in the second wave, and they’re spending less time needing ICU treatment.

“The number of patients being admitted to ICU in Alberta each day has increased significantly but has been counterbalanced by a shorter average length of stay in ICU,” said Dr. Noel Gibney, adding it’s now about three days shorter than in the second wave.
“The overall numbers of ICU patients has increased more slowly than the numbers being admitted.”

Gibney is the co-chair of the Edmonton Zone Medical Staff Association’s Strategic COVID-19 Pandemic Committee. He anticipates the peak number of COVID-19 patients in ICU in the third wave will be somewhere in the low 200s.
However, he points out non-COVID patients also still need of ICU care. Taking into account COVID and non-COVID patients, Alberta Health Services says there are 240 total patients in ICU right now.
Critical care physician Dr. Darren Markland says he’s a bit more cautiously optimistic in the third wave than he was in the second, despite the higher ICU numbers.
“There’s a lot less moral ambiguity with the third wave.

Get weekly health news
“With the second wave, we were seeing people who were much older and we really had to make decisions about whether people would benefit from ICU care, and that was agonizing.
“But now, when you have a 40-year-old otherwise healthy person in your emergency department, it’s clear. You go hard and they benefit from that care,” he said.

There are more patients in ICU but greater turnaround and fewer complications, Markland explained.
Read more: Alberta surpasses 2M COVID-19 vaccine doses administered as 1,558 new cases identified Thursday
“There have been some drug shortages but for the most part, the benefit of having so much of our vulnerable and frail population vaccinated is a lot of people come into hospital and turnaround quite quickly and we’re seeing shorter times in the ICU.
“When you’re young, the numbers look bad but the patients look good.
“We watch them very closely in the ICU, they never end up going on breathing machines and they turn around pretty quickly… and the ones that do have to go on ventilators… it’s much shorter.”

Dr. Daniel Niven, an ICU doctor in Calgary, is still bracing for what’s next.
“If you just do the math on that, the ICU admission number has been .07 per cent of the total, so seven out of every 1,000. So if you have 2,000 there is at least 14, but what’s not factored into that really yet is the impact of the variants, which have a higher risk of ICU admission.
“Our patient volume has never been higher.
“It’s dominated by COVID-19, it’s dominated by young, otherwise healthy patients with COVID-19 whose lives have been completely disrupted,” Niven said.
Read more: Hospital beds versus staff: Is COVID-19 overwhelming the human side of Alberta’s health system?
Andrea Irwin has worked as a Registered Nurse for about nine years. She’s worked casual shifts in Edmonton ICUs as well as her job in clinical education. Two weeks ago, she was redeployed to work all her shifts in the ICU.
“There’s been a lot of work done to make sure we can do this… that needs to be recognized. We’re here for Albertans if they need us. But it’s really shocking to see so many people so sick,” she said.

“We’re looking after people who don’t have COVID and we’re looking after a lot of people who have COVID.”
Irwin said, in her career, she’s never seen the need to double bed capacity, until now.
“It’s quite shocking to see that. I just think of the patients in the beds.
“There’s a lot of talk about capacity, but every person that’s there has a family and they’re very, very sick. And their lives will forever be changed, even if they survive.
“Every person that ends up in ICU that has critical illness, that’s life-changing. I just keep thinking about those people who are so sick from something that was preventable.”
She explains there are serious implications when the health system gets strained.
“Every day I check the numbers and I’m anxious every day to see the numbers because I know what that means,” Irwin said.
“The number of people sick — and so sick that they need ICU — everyday, that’s shocking and that’s really serious. Even if our health system can sustain this, the focus also still needs to be on the number of people who are very sick and currently experiencing very severe illness.”
Another challenge is hearing comments from others that the pandemic isn’t that bad or COVID-19 isn’t real, Irwin says.
“That’s probably the most distressing thing to me when I’m there more often,” she said.
“I actually get more upset about the comments because I’m seeing all these different people from all walks of life ending up very sick and that’s really hard and then to hear someone tell you that it’s not true and you’re making it up…”
She shares a metaphor she’s come up with.
“When I walk in the ICU… it seems like there’s been this mass event — say, a bus crash — and there’s this event that could have been prevented and people are super sick but we’re arguing about whether the bus crash happened.”









Comments
Want to discuss? Please read our Commenting Policy first.