Canada’s health care system could be a lot greener, experts say.

According to a new report, the health care system is the third-highest-emitting health system per capita in the world — behind Australia and the U.S. — but it represents not quite five per cent of Canada’s total greenhouse gas emissions.
By comparison, Canada’s agricultural sector accounts for about 10 per cent of emissions, the transportation industry 24 per cent and the oil and gas industry 27 per cent, according to government data.
Health care is relatively efficient, though, as it accounts for around 11 per cent of economic expenditure, but only five per cent of emissions, one study found.
But that doesn’t mean it can’t do better, the authors say.
“We all have a responsibility to do our fair share,” said Dr. Courtney Howard, an emergency room doctor in Yellowknife and lead author of the 2019 Countdown on Climate Change Briefing for Canadian Policymakers.
“It’s like a budget. Five per cent over time adds up,”

The report is part of the Lancet’s annual Countdown on Health and Climate Change Report, released Wednesday. This year’s report found that children around the world were at risk from climate change, including from malnutrition as a result of a changing food supply and infectious diseases that are expected to spread more easily.
Canada’s country report suggests that we cut back on emissions in the transportation sector, develop better plans to deal with wildfires, and clean up the health care system itself.
“One of the first things they taught me in med school was ‘do no harm,’” Howard said. “And so we want to be consistent with that in terms of how we’re actually conducting our own operation.”
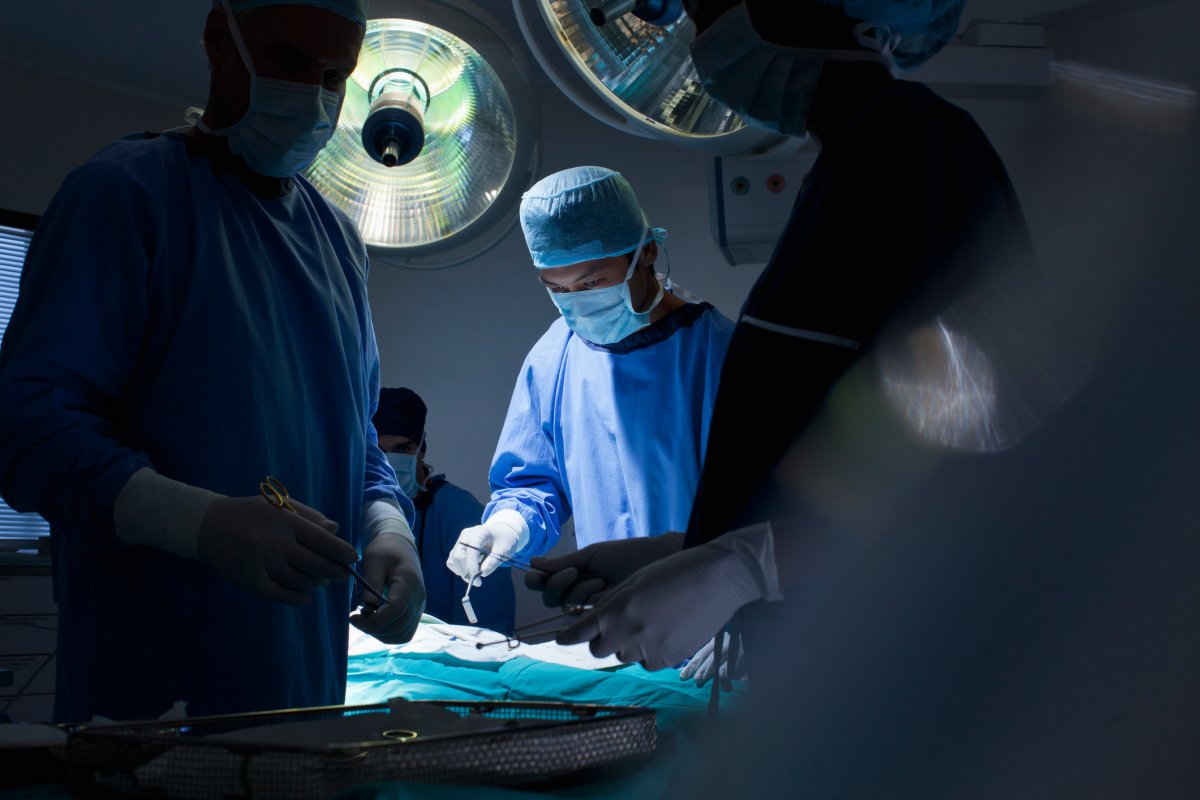
Hospitals and acute care facilities are big contributors to emissions in health care, she said. Aside from basic things like keeping the lights on, what goes on in an operating room can also have a big impact.
- Naloxone-resistant street drug linked to 9 deaths in Eastern Canada seized in Alberta
- ‘She gets to be 10’: Ontario child’s heart donated to girl the same age
- Buzz kill? Gen Z less interested in coffee than older Canadians, survey shows
- Bird flu risk to humans an ‘enormous concern,’ WHO says. Here’s what to know
A recent study comparing three operating rooms in Vancouver, Minnesota and the U.K. found that anesthetic gases used during surgery contributed significantly to a hospital’s carbon footprint.
So, too, did the ventilation systems in the operating room, which completely circulate the air many times a day. They constituted about 52 per cent of an inpatient hospital’s energy use.
Another huge contributor of emissions is the energy used to make, transport and dispose of items used in health care settings, like syringes, medications, bandages and so on. According to a report by the group Health Care without Harm, these account for 71 per cent of emissions attributable to the health care sector.
Howard believes there’s “low-hanging fruit” that could be tackled to reduce the sector’s emissions.
Some anesthetic gases are more polluting than others, she said. That same study showed the British hospital relying on a different anesthetic than North American ones, which meant these emissions were lower.
“So if anesthetists simply switch from one to the other, it can result in a really big decrease in greenhouse gas emissions.”
The operating room study found that simply turning off the ventilation systems in unused operating rooms at Vancouver General Hospital in the middle of the night or on weekends reduced their energy use by half.
“That’s a lot of wasted energy,” she said. “And when they fixed it, they also saved a lot of money.”
Fixing these problems won’t necessarily be expensive, she thinks.
“We anticipate this will actually save money,” she said, by reducing energy use or moving away from certain disposable items — which have to be manufactured and transported — to reusable ones.
“I remember when I was a med student at Squamish Hospital, there was one day when the rep came in to extoll the virtues of disposable drapes,” Howard said. Many hospitals in the early 2000s swapped out their surgical drapes, which are placed over the patient during surgery, for a disposable option.
Unfortunately, she said, when staff threw out the drapes after the surgery, they often also accidentally threw out a lot of expensive surgical instruments that were caught in them.

Canada wouldn’t be the first country to tackle emissions in health care, either. Between 2007 and 2017, the U.K.’s National Health Service reduced its emissions by 18.5 per cent, despite increasing clinical activity. Howard attributes this mostly to government standards and programs that applied to all public sector activities, including public health.
As the Canadian public becomes increasingly aware of the links between climate change and health, she said, she thinks that both health care providers and their patients will increasingly want to take action.
“I think this is just a place where there’s huge win-wins for all of us to be making change that we can all feel good about.”

Comments