More than 7,000 Canadians died from chronic exposure to air pollution in 2015, a new study on the health impacts of climate change found, and that’s just the tip of the iceberg.

According to a Canadian briefing done as part of the Lancet Countdown 2018 international report on climate change and health, Canadians can expect to experience more allergies, heat stroke, respiratory illnesses like asthma, vector-borne diseases like Lyme disease as well as cardiovascular impacts from chronic air pollution.
“This is a code blue for the environment,” said Dr. Courtney Howard, an emergency room physician and lead author of the Canadian report.
“This is a situation that requires urgent response.”
The report, released Wednesday evening, recommends that all levels of government standardize ways of tracking heat-related illness and death, that climate change and health become part of medical school curricula, phase out coal-powered electricity and apply carbon pricing as soon as possible.
Here’s what the report says about the potential impact of climate change on Canadians’ health — and how we’re already seeing the effects.
READ MORE: Donald Trump doesn’t believe his government’s own climate report warning of U.S. economic harm
Heat-related deaths may increase
A prolonged heat wave was blamed for more than 90 deaths in Quebec in the summer of 2018 and experts predict more hot days to come.
“We know heat events are increasing in Canada,” said Peter Berry, a senior policy analyst at Health Canada’s climate change and innovation bureau. Hot days, and especially hot nights, mean that people can’t cool down and are vulnerable to heat stress, heat stroke and even death, he said.
WATCH: Why did Quebec have so many heat-related deaths in July?

Health Canada has expanded the number of heat alert systems across Canada in response, he said, as well as developed a guide for health-care workers on how to diagnose and treat heat-related illness.
Air pollution could cause more death and illness

Get weekly health news
The Lancet report estimated that 7,142 deaths were attributable to air pollution, specifically particulate matter, in Canada in 2015. A November 2017 report from Health Canada put the annual figure a bit higher, at around 9,500.
“Exposure to ambient air pollution, for example, increases the risk of premature mortality from heart disease, stroke and lung cancer,” reads the Health Canada report.
New diseases will creep into Canada
Lyme disease, virtually unknown in Canada decades ago, has been skyrocketing in Canada recently. There were 144 cases in 2009 and 1,479 in 2017, according to data from the Public Health Agency of Canada.
WATCH: The number of cases of Lyme disease in Canada has increased 10 times in less than a decade thanks to tick bites.

West Nile Virus is also a good example of this kind of disease, said Susan Elliott, a professor of geography at the University of Waterloo.
And as these diseases become more common, doctors need to know how to recognize and treat them, she said. “There are so many stories we hear about people who go to their family doctor with symptoms of Lyme disease and they don’t get a diagnosis for weeks or months because our physicians are not trained to recognize the health impacts of climate change, like Lyme disease and other infectious diseases.”
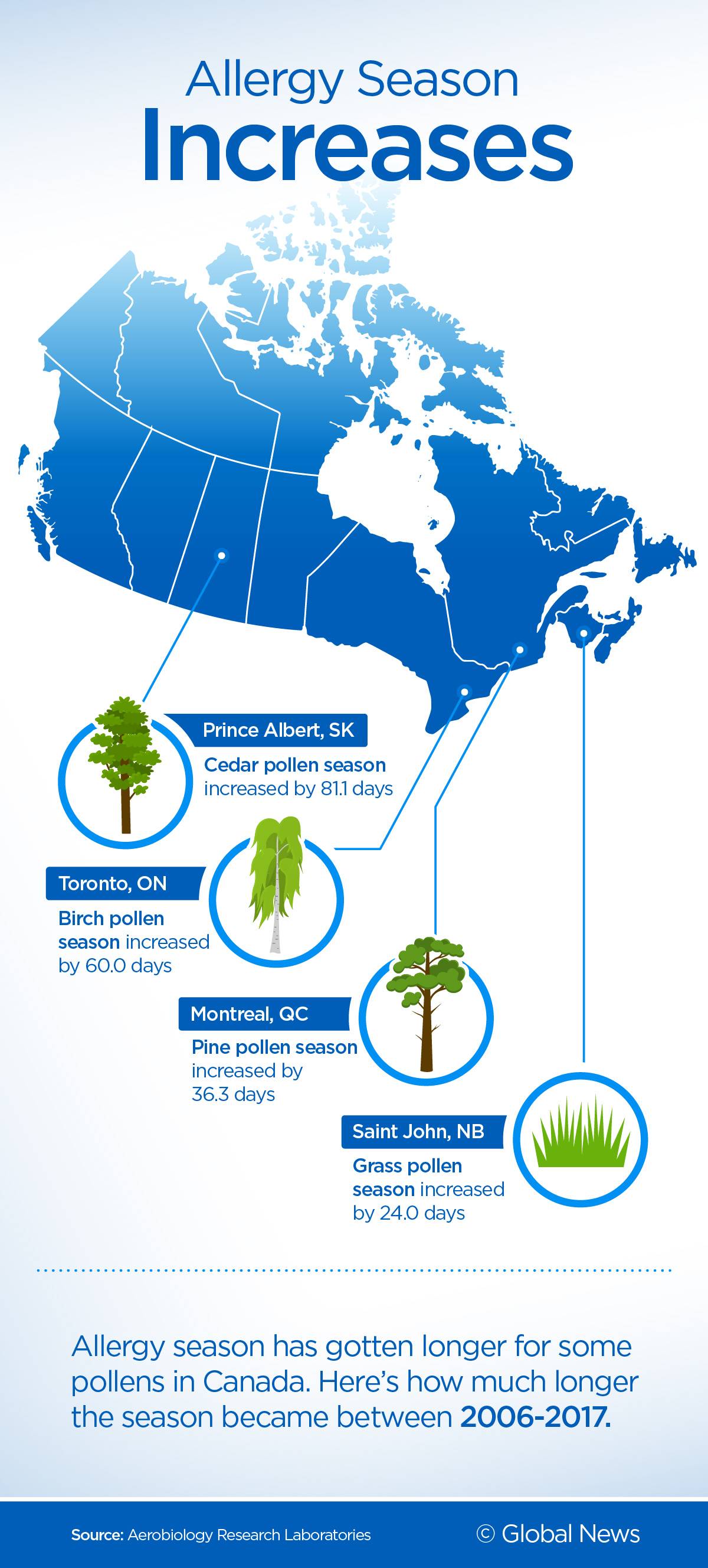
Allergy seasons will increase
Allergy seasons for various allergens have already been getting longer across Canada. Data from Aerobiology Research, a company that measures pollen and provides forecasts to the Weather Network and others, found that birch pollen season increased by 60 days in Toronto between 2006 and 2017, to give one example.
“You may not be allergic to ragweed today, but guess what, when the weather warms, there are going to be increasing amounts of environmental allergens and different types are now going to blossom that didn’t blossom before,” said Elliott.
“So we’re going to see a significant increase in environmental allergies in Canada.”
Disasters could lead to more mental health problems
Disasters like wildfire and floods don’t just create immediate danger, they can have a lasting impact on the people who experience them, the report said.
“You can imagine that if your house is destroyed, there’s additional stressors on you,” said Howard.
Researchers have found that people experienced elevated levels of depression and even post-traumatic stress disorder following the wildfires in Fort McMurray in 2016. Another study on residents of the Northwest Territories, which had a massive wildfire season in 2014, found that the fires had a detrimental event on their mental well-being, as well as contributing to more emergency room visits for asthma because of smoke.
Some research has also suggested that people are more likely to have problematic substance use following a disaster.
Howard believes that Canadians are beginning to take all these dangers seriously.
“People are seeing it in their day-to-day lives. So I think it makes it easier for us to make that diagnosis ourselves.”
She thinks that Canada can still deal with the problem. “If we pull together and look at this as a public health emergency, and treat it the way we treat other public health emergencies, it’s a really big opportunity for us to make real progress.”







Comments
Want to discuss? Please read our Commenting Policy first.