It has been a deadly year in British Columbia as the province grapples with an epidemic of opioid overdoses, many linked to the toxic narcotic fentanyl.

More people now die from overdoses in B.C. than car accidents, with nearly 700 deaths so far this year alone.
For many the deaths are a statistic – a numbers game. Not so to the men and women on the front lines, who come face to face with fentanyl and its deadly effects every day.
Emergency departments under the Vancouver Coastal Health authority have already handled nearly 4,700 illicit or unknown drug overdoses this year.
Seventy per cent of them go to St. Paul’s Hospital.
LISTEN: BC’s Opioid Epidemic: A Non-Stop Emergency in Vancouver
The new normal
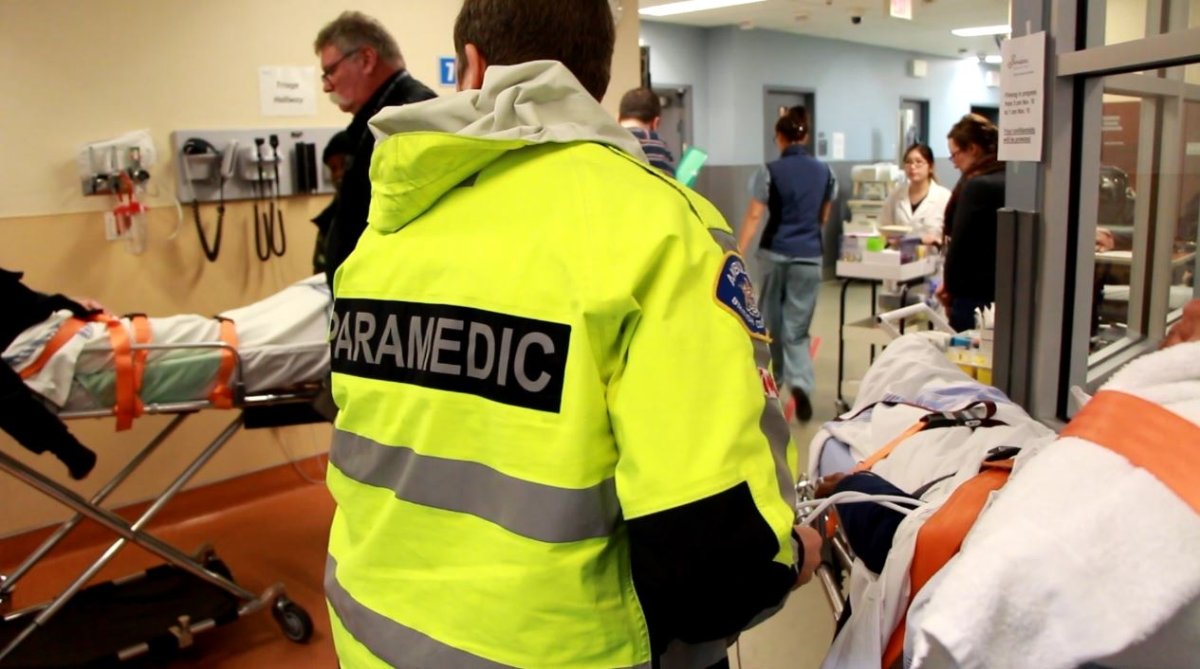
It’s early on a Friday evening, around 7 p.m. One overdose patient is on a stretcher in the Ambulance Bay area of St. Paul’s Hospital.
Within minutes, three more arrive, sitting on chairs, barely lucid, completely hunched over. These days, it’s a sight seen every shift by emergency room Doctor Kevin Nemethy.
“Sometimes we see patients who are awake and alert and interactive, sometimes we see patients who are still a little bit drowsy if the medication hasn’t been totally effective as an antidote. And sometimes we see the reverse, where we see agitated patients because they are completely in withdrawal from the opioids they are used to,” he explains.
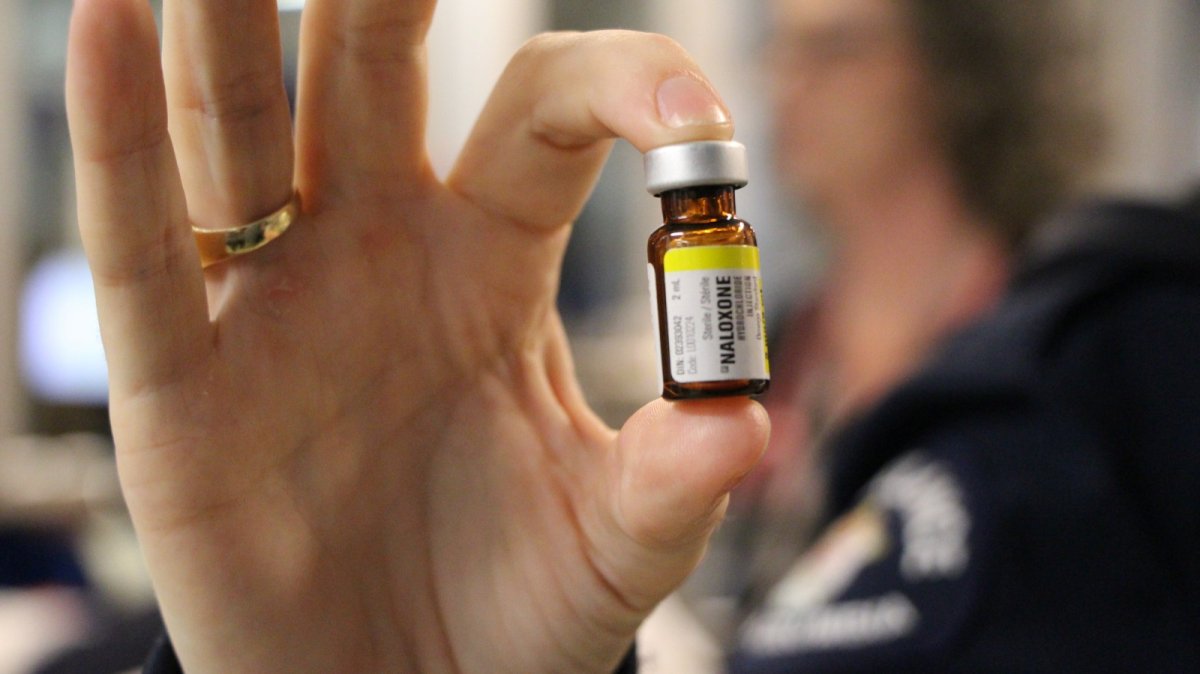
For Dr. Nemethy, his colleagues, and the triage nurses and paramedics at St. Paul’s, doling out naloxone to reverse the effects of an overdose is an everyday occurrence.
Dr. Dan Kalla, head of Emergency at St. Paul’s, admits it can put a strain on resources in a department that’s already seen volume rise by 25 per cent in the last five years.
“It fluctuates from night to night and week to week, and around the time of the welfare cheques it gets certainly much worse, so we’ll see anywhere from four or five overdoses anywhere up to double digits,” he says. “So certainly, it adds a whole new pressure to the department.”
But while every extra body adds demand, Kalla says overdoses themselves aren’t necessarily “heavy” to deal with. That’s because paramedics have often administered the antidote in the field – meaning the arriving patients are frequently breathing again, out of immediate danger, and often awake.
“We were busy before, now it’s just insane,” says paramedic Jason Neault.
“It’s call after call after call. There’s no rest, doesn’t matter what time of day it is, doesn’t matter if it’s a day shift or a night shift. We are run off our feet. And it’s exhausting, and it’s sad,” he says.
Indeed, much of the frontline ER care of OD victims ends up being performed by the paramedics.
In addition to administering naloxone, they’re often the ones to find space for the patients, to hook them up to oxygen and heart rate monitors, and monitor them in the triage area as they begin to recover.
Ironically, because the antidote they wield is so effective, it’s often the only care the patients end up receiving.
- Joffre Lakes to close for 3 periods this year under agreement with First Nations
- ‘Why aren’t we doing more?’ White Rock on edge with killer on the loose
- B.C. carjacking victim says she doesn’t trust the ‘catch-and-release’ system
- B.C. woman’s journey to sobriety highlights the need for drug treatment
In and out
Administering naloxone, says Dr. Nemethy, can be as much an art as it is a science.
With the strength of the fentanyl on the street, staff say they often have to give patients higher than usual doses of naloxone. But sometimes it’s exactly the opposite.
“We’ll actually try a low dose of antidote such that we get the patient breathing again but not necessarily awake and alert and fully reversed,” says Dr. Nemethy.
That was something CKNW witnessed firsthand; over the course of our night at St. Paul’s, at least four overdose patients roused themselves and walked out having never made it past the ambulance bay.
In fact – in many cases, they don’t even make it to the bay, according to Neault.
“A good majority of our calls in the Downtown Eastside area here in Vancouver, they don’t want to go to the hospital afterwards. There’s a real risk to that, they can overdose again. And we’ve seen that before, too, the same patient having multiple overdoses in one day,” he says.
ER head Dr. Kalla says while that situation – a repeat visitor in the same day – is fairly uncommon, seeing the same patients within a week or a month is not.
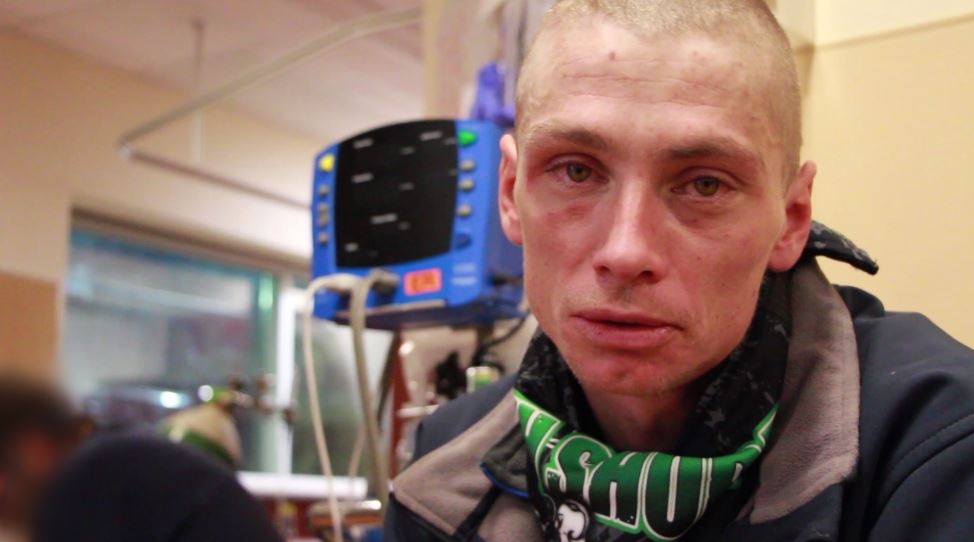
Take Alex Blume, who was escorted in by paramedics around 9 p.m., after overdosing on what he thought was heroin.
He says it’s his third trip to the ER in as many months, and says while he wants to kick the habit, he’s found detox centres and shelters full when he tried.
Asked if he’d go back out and score again that night?
“I have to. You’re gonna get dope sick, I won’t be able to walk, I won’t be able to move. So unless I go right from here into detox, I don’t have a choice. I don’t know if you guys know how much like… you are ready to murder somebody when you are dope sick.”
Less than an hour later, he told staff he was going out for a cigarette, and never came back.
WATCH: ER Doctor Joseph Finkler on the scale of the crisis

‘A killer like we haven’t seen in a long, long time’
“Certainly, with the introduction of fentanyl into the community, it’s changed the problem generally for the worse,” says Dr. Kalla.
“I don’t think people realize how deadly this problem is. I don’t even think users out there are aware of how quickly people are dying from this issue. This is a killer like we haven’t seen in a long, long time.”
Kalla says doctors are seeing increasing numbers of seasoned users come through the doors. He says they’re suddenly not knowing their dosage, taking what used to give them a high and now ending up on the edge of death.
That was Alex Blume’s case; he says he normally does between one and one-and-a-half points (tenths of a gram) of heroin; this night he did half a point and it nearly killed him.
He says he knows the drug supply is bad. He tries to manage the risk, but he can’t stop.
“You try to get from the same guy… I usually like to do a little tester first, a little dragon before I shoot it up. At that point you’re not really thinking about that because you’re so dope sick you just want to feel better, right?”
Kalla says as tough as it is to watch repeat patients come back in through the doors, they’re not the ones he’s most concerned about.
“I worry about the ones we don’t see again. Every day two or three patients are dying, most of them young.”
The mental toll
“Everybody that we touch and everybody that we deal with has a story and it’s difficult to hear some of these stories,” says Neault, the paramedic.
“The people using drugs on the Downtown Eastside are regular people. They are somebody’s daughter, somebody’s son, somebody’s father, somebody’s mother, et cetera, et cetera.”
He’s visibly emotional, and there’s no disputing the crisis has touched him. But he says it doesn’t wear him down, he doesn’t dread coming to work: he signed up for this for a reason.
WATCH: ER Nurse Lauren Parker on the mental toll

ER nurse Lauren Parker says there’s no doubt the higher volume leads to more stress for staff on the floor. And she says some of the cases they deal with are so tragic, they’re hard to let go.
“I saw a woman who was living in the Downtown Eastside, homeless, IV drug user, and she was pregnant. I’m not sure if she knew she was pregnant at the time, but unfortunately the baby passed away because she had overdosed… That was a very, very unfortunate case, very hard on the staff… we care about our people, we care about our patients, and we want to see people do well. And when these kinds of heartbreaking cases come in, it’s really, really hard on everyone.”
But while everyone on the floor has seen hard cases, Dr. Kalla says overall the crisis hasn’t affected morale.
“I think most of us who’ve worked here have seen everything once or twice,” he says.
“And we’re used to it. There’s a lot of compassion here for our patient population, and as I say, we know a lot of our clients here. I don’t know that it’s affected the morale – sometimes the volume is just too much and we get overwhelmed, but I think all of us want to see a solution that keeps the patients safe.”









Comments