Nursing has always been a demanding career, and that was never more true than over the last two-and-half years during the COVID-19 pandemic and fallout.

“I’ve been in nursing for about 20 years but I’ve worked in the health-care profession since the 80s,” said Alberta nurse Renee. “I’ve always wanted to be a nurse.
“I didn’t realize it for many months, because you became very consumed with the day-to-day work and just doing the tasks, but ultimately, the stress affected my health to the point where I had to seek medical help,” she said.
Global News agreed to use a pseudonym for Renee to protect her from potential job repercussions.
In the past, Renee had worked in medicine, day medical, palliative and family medicine. Just before the pandemic, she’d taken a leadership position in infection control at a long-term care facility.
“It was when I started noticing the deterioration of my own physical health that I knew I could not keep it up.
“When I look back to try to summarize what it was like working, the two words that come to mind are: perpetual anguish.
“To go to work with that everyday — going: ‘I don’t know how I’m going to get through today, I don’t know what we’re going to face today, individually and as a team,’ — it was just like dragging a big, heavy ball on my leg to get to work.
“But you did it. You had to. You had patients whose lives were affected… staff needed us there as well.”
Read more: Veteran Edmonton nurse on staffing shortages, skyrocketing COVID-19 patients: ‘It’s devastating’
In the spring of 2020, the challenges of nursing — the stress, tough schedule, staffing challenges, long hours, the high stakes, the tough decisions, the personal health risks, mental health drain — were exacerbated.
The stresses of front-line hospital nursing — severe illness and death, emotional family and loved ones, managing differing opinions, administrative red tape and taking that all home — increased exponentially.
Protests — some even outside hospitals — and political rhetoric and polarization only made things worse, several Alberta nurses told Global News.

Renee left her job in long-term care and took a community nursing position in a Primary Care Network (PCN).
“I wanted to be back with patients and feel like I was making a difference,” she explained. “I really enjoy what I’m doing again. Once you get out in the community and find other positions that relate to your profession, there can be a lot of autonomy. Once you get a taste of that, it can be very empowering, very rewarding.”
For registered nurse Ali Ryan, the pandemic conditions were the final push she needed to make a change.
“I just wanted to come home and not be so exhausted mentally.
“I love nursing. I love the fact that we can empower our patients with knowledge and ease their suffering and help them, but in the same token, I wanted to do something a little more creative and do something less intense all the time. Mentally, it was the right time.”
After working in neuro surgery and then recovery, Ryan decided to finally enroll in a medical aesthetics course.
“It was something I’ve thought about for a long time. I’ve always been a pretty creative person and then with the pandemic — and seeing everybody just at their wit’s end and the burnout of that — I think gave me that extra incentive to say: ‘OK, it’s time for a change.'”
She now works in aesthetics, providing cosmetic injections, while still picking up casual shifts in hospital.
“I love the hospital. I love my colleagues. I love the nature of the work.

Get weekly health news
“I just think mentally, I have to look after my own health and I have to be not just ‘Nurse Ali,’ but a mom and a good friend and a good family member. And if I want to do all those things, then I need to have boundaries and I think that’s OK.”

Ryan says her work now has better hours, allows her to spend more time with her two young children and gives her more work-life balance.
“You can’t give good care if you’re hating what you’re doing. We’re lucky as nurses that we can move around and I think we need to keep our eyes open to those opportunities.”
The work is also just more positive, she says.
“You’re helping people feel beautiful and giving them a little pick-me-up.
“There’s nothing better than having that interaction with people where they walk away going: ‘Oh, I love it,’ and carry on. This is the joy of nursing: you can work in so many different capacities.”
Schools and companies that offer courses in cosmetic injectables have seen a huge increase in registration over the last two years. Frida Academy in Calgary saw its highest enrollment ever in 2021, doubling from the year before. It had to add courses to meet the demand, a spokesperson told Global News.
Renee and Ryan aren’t the only two who have left the front lines; the union that represents Alberta nurses is noticing a definite trend.
“This is a common refrain that we’ve been hearing from nurses in all sorts of practice settings,” said Cameron Westhead, second vice president of United Nurses of Alberta.
“Whether it’s moving from ICU to a less acute type of care provision or from moving from full-time to part-time or part-time to casual, nurses are experiencing an incredible amount of stress and they’re looking for ways to reduce that and have more of a semblance of a work-life balance.”
The union says issues that existed prior to COVID-19 — nursing shortage, the relationship between the government and healthcare workers — were inflamed by the pandemic.
“When you’re dealing with these stressful situations — violence in the workplace, mandatory overtime, working short staffed — having your work acknowledged as important and critical in providing healthcare to Albertans,” Westhead said.
“Vacations are being denied, working short staffed, mandatory overtime, sometimes a lack of training.
“With Connect Care, which is an electronic documentation method, nurses are being asked to undertake this training on their spare time and are not being paid for it or being asked to do it without pay.
“It’s one demand being placed on top of another and it just eventually results in a collapse.”

The union said it’s noticing more nurses moving away from certain units (ICU and other critical care units, in particular) and into other units, like recovery, where the proportion of shift work is less.
“We’ve had so many nurses from cardiovascular ICU, ICUs come over to recovery room,” Ryan said, “because you have better working hours, your patients flow throughout the day, so you’re not spending endless time where you’re seeing just chronic suffering all day long.”
The UNA is also noticing more Alberta nurses moving from full- or part-time to casual.
“Casual nurses are able to have much more control over their schedule,” Westhead explained. “They can’t be mandated to come in to work, and they’re able to refuse shifts as well, which is not the case with part-time or full-time nurses.”
Currently, just over 25 per cent of nurses working for AHS and Covenant Health are casual.
Westhead understands why other nursing jobs might be appealing.
“Settings like aesthetics and community care, primary care, involve a lot less shift work and and so it’s much more predictable in terms of how you can juggle your family life and your professional life.”
Alberta Health Services says it’s increasing the nursing workforce and says there are 1,900 more nurses working now than before the pandemic.
AHS hired 1,188 RN/RPN graduates — nearly 90 per cent of the 2021/22 Alberta RN grads.
However, AHS says there are still staffing strains, especially in general medicine and emergency in the large hospitals in Edmonton and Calgary, where demand is highest.
“Vacancies have increased because we are recruiting aggressively to increase the workforce further,” AHS spokesperson James Wood told Global News.
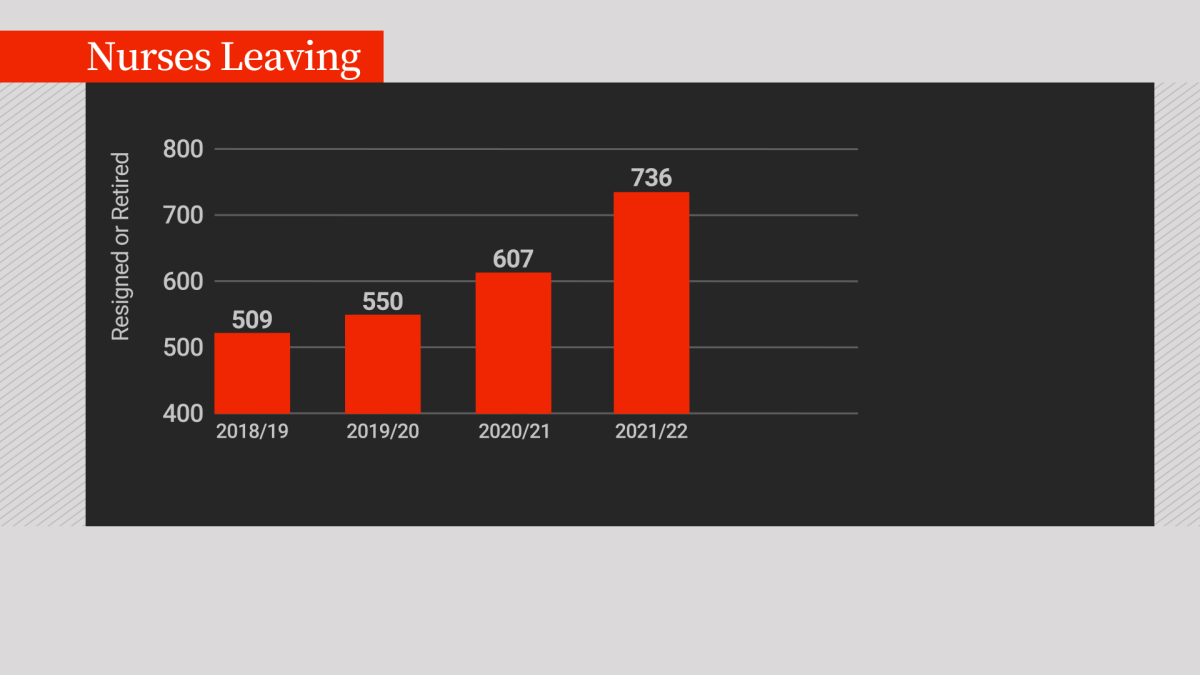
Data shows both AHS and Covenant Health saw an increase in the percentage of nurses leaving during the pandemic. In the 2018/19 year, 459 full or part-time registered nurses resigned or retired from AHS (two per cent). In 2021/22, that number was 686 (2.8 per cent). (At Covenant Health, it went from 2.7 to 2.9 per cent).
In what world could they stay?
Could AHS or Covenant Health have made any changes that would have made Ryan or Renee consider staying?
Additional resources would help, Renee said, as would more autonomy and a less “top-heavy” organizational structure.
Ryan says the system, in a lot of ways, is broken. She’s not sure if any changes could have convinced her to stay full-time, but believes listening to front-line staff about what they’re experiencing would go a long way.
“Flexibility with hours, flexibility with shifts and allowing people to get the time off that they need” would also help foster a better work-life balance, she said.
“Creating more part-time lines that people can then share full-time positions would be hugely helpful because people get locked into these full-time rotations that are just not healthy. They’re working seven days in a row. That’s not good for anybody.”

Westhead says the union believes making current nurses feel valued and supported would be a good first step.
“The retention of senior nurses is one of the most important factors for mentoring new grads and nurses who are new to that specialty area of practice,” he added.
“I think what nurses are looking for is hope.
“We know that from time to time there are exceptional circumstances like pandemics or natural disasters that require us to go above and beyond even the contributions we normally make. But we also want to know that there’s going to be a light at the end of the tunnel.”
Ryan wants to encourage all nurses to consider their own health and wellbeing.
“The options are out there.
“You just have to open your eyes, be a little brave and be willing to take that leap of faith and just go for it.”









Comments
Want to discuss? Please read our Commenting Policy first.