While the Middlesex London Health Unit (MLHU) reported the first detected case of monkeypox in the region on Monday, an expert and local consultant on infectious diseases aims to calm residents’ nerves, saying the disease “is much less contagious than COVID-19.”

MLHU staff members have determined that the person diagnosed with monkeypox has had no close contacts who require post-exposure action to prevent infection or additional follow-up from public health.
“Although we are reporting this new local case of monkeypox, the risk of the community remains very low,” said Dr. Alex Summer, chief medical officer of health at MLHU.
Summers could not “expand profoundly on the details” of the specific case in the region, yet the MLHU believes that it is associated with travel and not from transmission.
Monkeypox is a viral, endemic illness that is typically transmitted from animals to humans.
“It can be spread to people through direct contact with the bodily fluids or lesions of infected people or animals, as well as from contaminated clothing or bedding and through respiratory droplets following prolonged exposure to an infected person,” described in the MLHU media release.
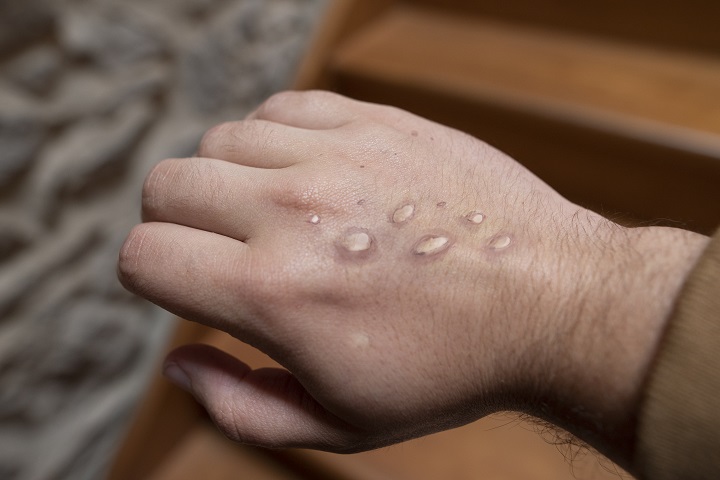
Symptoms of monkeypox are similar to but less severe than smallpox, which can include fever, headache, swollen lymph nodes and lethargy, followed by the development of a rash referred to as pox lesions. The rash can appear on the face and appears a few days after symptoms begin with the possibility of spreading to other parts of the body.
According to Dr. Sameer Elsayed, an infectious disease physician and professor at Western University, monkeypox is associated with a group of closely related viruses that include smallpox, cowpox, and camelpox.
“Monkeypox virus was first discovered in 1958 as the cause of a non-fatal, smallpox-like skin disease of captive monkeys at a research facility in Denmark. They were using these monkeys for polio vaccine manufacturing,” Elsayed said.
“However, a research study done not too long ago showed that monkeypox existed even before the 20th century.”
Skin samples collected from about 1,000 preserved rodents who lived prior to the 1900s were found with traces of monkeypox virus DNA. This study was performed in museums, one in New York City and the other in Central Africa.
As a result of these findings, Elsayed said the name monkeypox is a misnomer — a wrong or inaccurate use of a name or term — since “terrestrial African rodents (rats and squirrels) serve as the natural reservoir of the virus while monkeys and other primates are believed to have been accidentally infected.”
The first case of a human contracting monkeypox was in a nine-month-old baby in the Democratic Republic of the Congo in the 1970s, after smallpox vaccination programs started to disappear and monkeypox cases began emerging in Africa.
While there is no specific treatment for monkeypox infection, antivirals and prior vaccination against smallpox have helped provide cross-protection, according to the MLHU.

Get weekly health news
There are two strains of the monkeypox virus, Elsayed said, that have been described in Africa: West African strain and Central African strain. The mortality rate for the West Africa strain is approximately 3.6 per cent while the mortality rate for the Central African strain is about 10.6 per cent.
“However, these rates were based on research conducted in Africa between the 1970s and 1990s and may not be commensurate with what would be expected for incidental infections seen among individuals living in developed countries,” Elsayed said.
The Democratic Republic of the Congo has had the “biggest share of cases,” according to Elsayed, specifically in children from constant touching and handling of animals who carry the disease.
But human monkeypox infection is not new to Europe and North America.
In 2003, an outbreak of infections involving over 80 children and young adults broke out in several Midwest states in the U.S. after acquiring exotic pet prairies dogs which became sick after contact with African rodents during transportation and importation.
Yet there were no human deaths, Elsayed said, adding that three children were noted to have experienced brain inflammation or encephalitis but eventually recovered.
“Between 2018 and 2021, several travel-associated cases of monkeypox infection were noted among visitors to Nigeria who returned to the United Kingdom, Israel, Singapore, and the U.S., with no deaths reported,” Elsayed said.
All recent infections, including the one identified in the London region, have been due to the West African strain, or clade, which appears to cause milder symptoms compared to the Central African clade.
However, Elsayed said that clinically, it may be difficult to distinguish the two strains of monkeypox.
“After the virus spreads from the area of inoculation or entry, it then travels throughout the body and eventually it will go to the skin, and it may go to other places,” Elsayed said. “So, it may go to the eye, it may go to the liver, rarely will it go to the brain as a cause of inflammation, but usually the target site is going to be the skin, the same for both strains.”
Elsayed added that he was not surprised to hear about the first reported case of monkeypox in the London region.
- Toronto library, UHN offer mobile health clinic to reach most vulnerable
- Alberta rolls out activity-based surgery funding model to more public hospitals
- Saskatchewan drug traffickers can now face civil lawsuits for related damages
- Ebola cases in Congo reach 282 as Brazil investigates 2 suspected cases
Elsayed said people are more mobile now, and not just internationally but also provincially.
“During the COVID-19 pandemic, people were not really mobile during that time. Now people are feeling a little bit freer and perhaps there’s more interpersonal contact and gatherings after a two-year hiatus. I guess, from activities and crowded events, things can spread pretty easily from person to person when you’re dealing with an infection.”
But Elsayed said that monkeypox is not anywhere near as contagious as COVID-19.
“The West African variant of monkeypox is 100 times less contagious than the Omicron variant of COVID-19,” Elsayed said.
Unlike COVID-19, he said that there is no evidence that monkeypox virus is transmitted by the airborne route.
Bites from infected animals and consumption of infected animal meat are common ways of acquiring the infection in Africa, though “physical contact remains the most frequent mode of transmission,” according to Elsayed.
“You need 10 people with monkeypox to transmit the virus to one person essentially,” Elsayed said, “versus Omicron, where you have one person that infects 10 people.”
Elsayed believes that a lot of people are afraid after the seemingly constant panic and stress caused by two years of anxiety from the COVID-19 pandemic. “But monkeypox is a different virus.”
“It has a different means of transmission and many people who are over the age of 50 have been vaccinated against smallpox,” Elsayed said.
“As long as these individuals have an intact immune system, don’t have any other major health problems, they will have some degree of protection against monkeypox, with an 85 per cent cross-protection in general with the smallpox vaccines.”
According to his research, monkeypox has been infecting humans for over 50 years with more than 1,000 cases reported in the Democratic Republic of the Congo annually.
No deaths have occurred in any cases reported outside of Africa.
Infection control recommendations, however, align similarly to those related to COVID-19, Elsayed said.
“People who are infected with monkeypox should wear surgical masks, and skin lesions should be covered until they have healed,” Elsayed said. “Personal use items such as towels and sheets should not be shared.”
Frequently touched surfaces should also be regularly disinfected, and social distancing should be practised with household and non-household members until the illness is resolved.
“In humans without prior smallpox vaccination, the chance of a close household contact becoming infected is between seven and 12 per cent, compared to three per cent or less for non-household contacts,” Elsayed said.
“I’m personally not worried about monkeypox more than I am about other things that affect public health such as mental health, education, alcoholism, and cigarette smoking,” Elsayed said. “Those are more important, in my opinion, in terms of tackling public health issues.”











Comments
Want to discuss? Please read our Commenting Policy first.