This the fourth in a series of stories on temporary emergency room closures in Nova Scotia. To check out the rest of our CODE ZERO series, click here.

Nova Scotia’s health minister believes the new agreement between the province’s government and its doctors will provide a solution to ER closures in rural Nova Scotia.
Randy Delorey said the new master agreement, a four-year labour deal approved by Doctors Nova Scotia last month, will make the province’s emergency physicians the highest-paid in the region.
“We believe this will help with both our recruitment, retention and perhaps encourage some physicians who may not have been providing those services but have the expertise to do so to maybe consider filling those positions as well,” he said.
Delorey’s comments come after Global News analyzed provincial government reports and found a sharp increase in temporary emergency room closures in Nova Scotia.
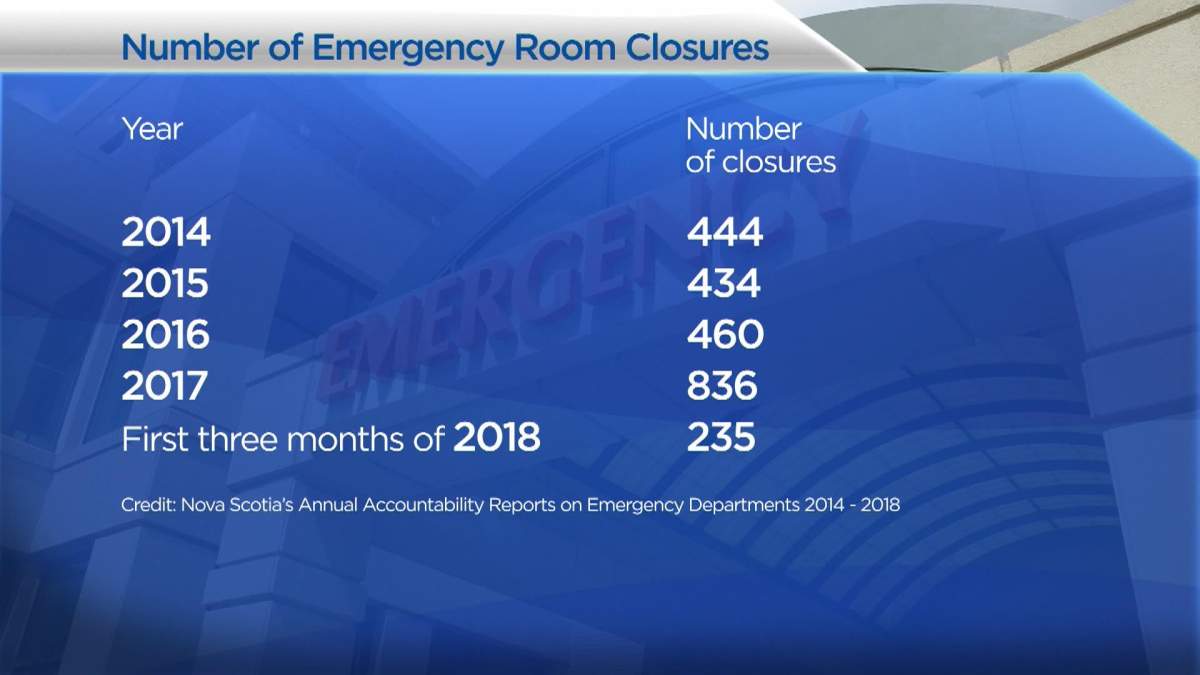
Between 2014 and the first three months of 2018, just under half of the emergency rooms in the province — 18 of 37 — were forced to temporarily close, often as a result of a lack of doctors or nurses.
Most closures are unscheduled and can come with as little as half a day’s notice.
In 2014, Nova Scotia’s ERs temporarily closed 444 times. By 2017, the number of temporary closures had jumped to 836.

Get weekly health news
In the first three months of 2018, the most recent publicly available data, there were 253 temporary closures.
If closures continued at the same rate, the province would be on track to set a record with more than 1,000 temporary closures in 2018.
Delorey characterized the recent increase in ER closures as the culmination of 15 to 20 years of health policy rather than the result of actions taken by the Liberal government, which was swept into power in 2013 under Premier Stephen McNeil.
“We’ve recognized a lot of those challenges do relate to workforce availability,” the health minister said.
“That’s challenges that are shared not just in Nova Scotia, but in jurisdictions across Canada.”
When it was pointed out that the closures only doubled in 2017 — well into the Liberal government’s first term — the health minister once again pointed to the lack of available staff.
- Leadership vote to be announced for B.C. Conservative Party after Rustad ouster
- Suspect dead in officer-involved shooting in Surrey, B.C., investigation ongoing
- Immigration lawyers say automation is partly driving a massive Federal Court backlog
- Ottawa under increasing pressure to show how policy changes are affecting emissions
He admitted that it’s not ideal for local emergency departments to close but said that it’s important to remember that regional hospitals do not close, remaining open “100 per cent of the time” even when smaller, rural facilities are forced to temporarily close due to staffing issues.
“So it’s not a decision made lightly,” he said.

No plans to consolidate facilities outside of Cape Breton
Delorey says the upcoming revitalization of the health care system in Cape Breton came under unique circumstances but didn’t say “no” when pressed on whether the province has similar plans for other areas of the province.
Announced in 2018, the plan would see the Northside General Hospital in North Sydney and the New Waterford Consolidated Hospital in New Waterford permanently closed as beds and resources are shifted to an expanded Cape Breton Regional Hospital in Sydney and a strengthened Glace Bay Health Care Facility in Glace Bay.
The response from Cape Bretoners was hostile but it’s believed that consolidation could work to help reduce the number of closures at the Glace Bay Health Care Facility, which between 2014 and the first three months of 2018 was closed 364 times — the most of any ER in the province during that time period.
The health minister said his department will continue to work with the Nova Scotia Health Authority to monitor staffing levels and that he hopes the revitalization project delivers the results Nova Scotia is looking for.








Comments
Want to discuss? Please read our Commenting Policy first.