Nicole Polizzi, also known as Snooki from the TV show Jersey Shore, isn’t afraid to get real about her adventures in motherhood.

Now, the reality star is opening up about a painful side effect of breastfeeding: mastitis.
READ MORE: Mom’s raw photo shows the painful side of breastfeeding — ‘Why is this so hard?’
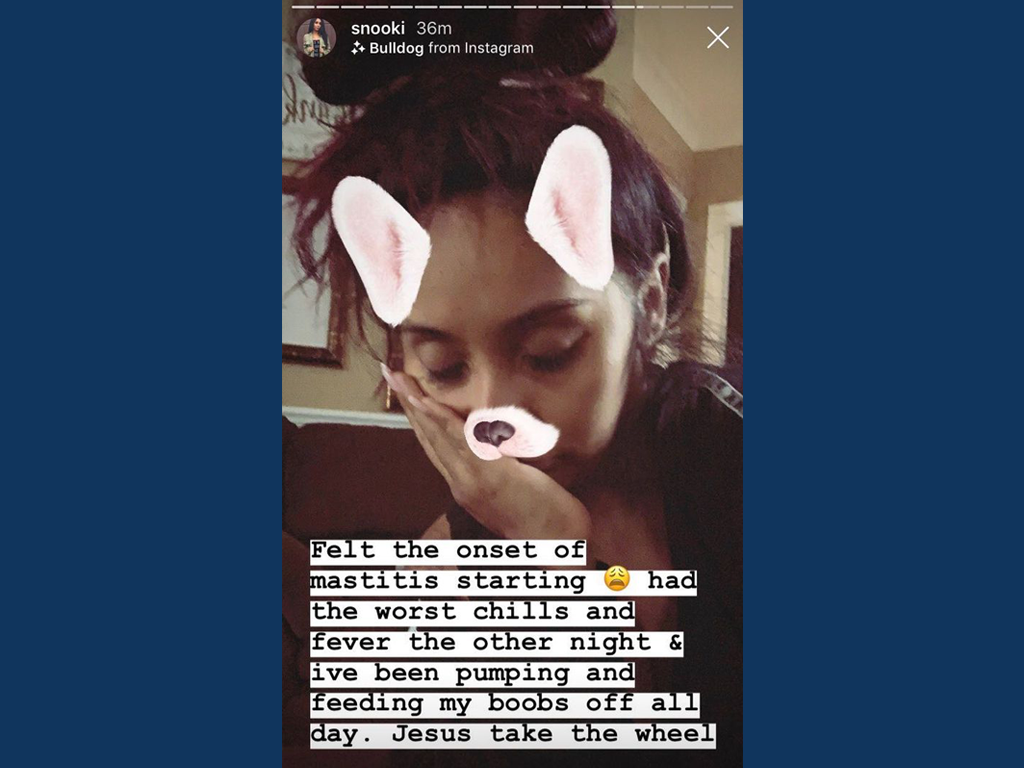
In an Instagram story on Thursday, Polizzi shared a picture with her head in her hands.
“Felt the onset of mastitis starting. Had the worst chills and fever the other night, and I’ve been pumping and feeding my boobs off all day. Jesus, take the wheel,” she wrote.
She and her husband Jionni LaValle welcomed their third child, Angelo James, at the end of May.
READ MORE: When should your child stop using a stroller?
According to the Canadian Breastfeeding Foundation (CBF), Polizzi’s symptoms sound similar to those of mastitis, which can also produce a painful lump in the breast and redness near the infected site.
“Mastitis is due to an infection (almost always due to bacteria rather than other types of germs) that usually occurs in breastfeeding mothers,” says the site.
Jandy Beresford, a board-certified lactation consultant based in Durham Region, Ont., says mastitis is most often caused by a blocked duct.
“It’s milk that has stayed in the breast too long… if that blockage isn’t cleared, it gets infected and then it can cause some serious symptoms for the mother and be very uncomfortable,” Beresford told Global News.
Signs and symptoms
In Beresford’s experience, mastitis makes you feel like you’ve been “hit by a truck.”
“It’s like getting the flu really badly and really quickly,” she said.
Sometimes, you can feel the bump of hardened milk, though not always. It depends on where the lump is in your breast.
“The telltale sign of mastitis is a fever because it’s an infection,” said Beresford.
According to Dr. Jack Newman, founder of the International Breastfeeding Centre, a blocked duct can occur when the mother has an abundant milk supply but the baby’s latch is not as good as it can be.

Get weekly health news
“This results in poor drainage of the breast while the baby is feeding,” he said.
Unfortunately, the presence of mastitis can make it even more difficult for the baby to feed.
“Often, the breast will not empty well because of the swelling,” said Newman.
WATCH: 50 litres of breast milk donated by Okanagan mothers to help babies in need

In his view, a mother with mastitis should continue to breastfeed with the affected breast as long as the pain isn’t too bad.
“For years, physicians had been telling mothers not to feed on the affected side, which makes no sense at all,” he said.
Maintaining a normal feeding schedule should allow the duct to clear on its own.
READ MORE: Breastfeeding mother claims she was asked to leave Montreal courtroom
If the pain is too severe, both Beresford and Newman recommend ibuprofen, which is anti-inflammatory and will ease the pain.
“If it’s not getting better in 24 hours, you want to get antibiotics,” said Beresford. “You don’t want to let it get worse.”
If left untreated, mastitis can lead to an abscess in the breast. Sometimes, surgery is necessary.
Can it affect the baby?
If you have mastitis, you don’t need to worry about your baby catching the infection because you’ve already shared all of your germs via breastfeeding.
However, if the pain isn’t too severe, you should continue to nurse because it’s the baby’s natural shield against illness.
WATCH: Alberta woman gives new meaning to term hockey mom

What you need to ensure is that your baby doesn’t get hungry, says Beresford.
“There’s a blockage… which may affect the flow of milk, and the baby may get frustrated,” she said. “Sometimes, the baby won’t be able to get enough.”
In this case, she would recommend consulting a lactation expert who can help you and your baby get back to a normal feeding pattern as soon as possible.
Prevention
To avoid mastitis, it’s crucial that the baby achieves a good latch on the very first day of breastfeeding.
He added that it’s not normal for the mother to have sore nipples, although it is a common side effect of breastfeeding.
READ MORE: Breastfeeding for 6 months can cut women’s risk of diabetes, study says
Beresford emphasizes that everyone’s experience with breastfeeding will be slightly different. The important thing is that the baby is getting the nutrients he or she needs to grow.
“If your baby is latching on and drinking well, if they’re satisfied when they come off the breast… if they’re growing well, if they’re happy and content, if you can put them down, if it doesn’t hurt… things are going well,” she said.
“If any of those things aren’t happening, then see a breastfeeding specialist or a lactation consultant… so you can prevent potential issues.”
Meghan.Collie@globalnews.ca








Comments
Want to discuss? Please read our Commenting Policy first.