Paediatricians should offer intrauterine methods of contraception as first-line birth control options for youth, the Canadian Paediatric Society (CPS) says in a new position statement.

The statement, released Thursday, looks at the pros and cons of each type of birth control method and provides healthcare providers with the strategies and tools to help them discuss suitable contraception methods to youth.
READ MORE: One-third of young Canadian women can’t afford menstrual products, report finds
“Long-acting reversible contraception is a really effective and safe way to provide contraception,” says Dr. Giosi Di Meglio, member of the CPS Adolescent Health Committee. “In Canada, the only long-acting reversible contraception that we currently have is the intrauterine system (IUS) and the intrauterine devices (IUD), but providers are often under the misperception that they’re not safe to use in teenagers and we’re trying to get the message out that they are safe to use with teenagers.”
According to Di Meglio, this outdated perception dates back to the 1970s where people thought that the intrauterine contraceptives increased the risk of pelvic inflammatory disease, which is actually not the case. They were worried about fertility so they tended to use intrauterine contraception for people who already had completed their families, or felt that the risk of infertility was not a concern to them.
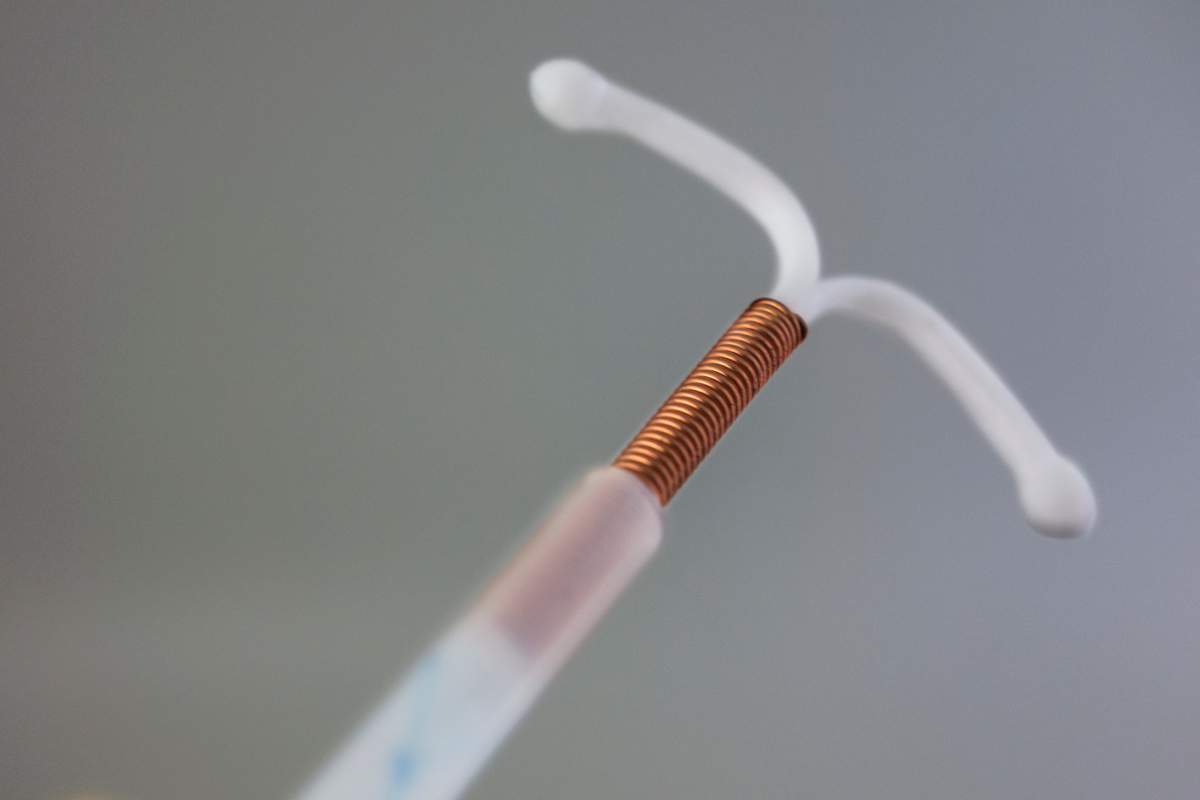
An IUD or IUS is a small, often T-shaped device implanted inside the uterus by a healthcare provider to prevent pregnancy. Both methods can stay in place over the course of several years but can be removed at any time by a healthcare provider.

Get weekly health news
The two methods are more than 99 per cent effect, the CPS says. This is compared to the hormone pills which are 91 per cent effective and condoms which are 82 per cent.
Just like with any method of contraception though, intrauterine methods do come with some potential risks and side effects, but they are often minimal.
If you are allergic to copper, there may be a possibility of an allergic reaction, De Meglio says. However, that is rare.
If you have an untreated pelvic infection, then the device or system may also impact your fertility. This is something physicians will discuss before putting the device or system in and any potential symptoms of an infection will be discussed beforehand.
As well, there is a slight increased risk of acquiring an infection from the bacteria within the vagina after insertion.
“Any time you do anything in the womb as a procedure and you go through the vagina, you have a tiny risk of infection,” Di Meglio explains. “But if you treat it promptly, then it’s not an issue for fertility.”
There is also a small risk of perforation when the device is inserted. And lastly, some people’s body may reject the device and it may fall out. That, too, is rare, Di Meglio says.
As for side effects, some devices come with more than others.
“With the copper IUD, it can increase cramps and the volume of bleeding when you have your period,” Di Meglio points out. “And with both types of IUDs, sometimes when you insert it, there is a period of time when you have a lot of spotting after the insertion but that usually settles down.”
READ MORE: Should women be entitled to time off work during their periods?
And with the IUS, Di Meglio says sometimes people will bleed a lot less or not at all while menstruating. Usually, with this method, there aren’t a lot of side effects. In fact, the cramping one experiences during a period is often less.
Every now and then, Di Meglio says she’ll encounter people who have side effects from the small levels of hormones that come with these methods, like nausea.
However, the benefits of IUD and IUS methods far outweigh the minor and rare side effects and risks.
The CPS statement also advises that providers:
- Discuss sexual health, fertility, family planning and contraception with all youth starting early in adolescence, preferably before they become sexually active
- Have a collaborative approach that empowers youth to makes informed decisions about their birth control options
- Encourage youth to always use condoms, regardless of the method of birth control they use, to prevent sexually transmitted infections
- Inform youth about emergency contraception as back-up methods of preventing pregnancy
Di Meglio hopes that these recommendations help in reducing common barriers adolescent girls run into today when it comes to contraception and their sexual health — barriers like the cost and the referral process, which Di Meglio says hinders an efficient process because healthcare providers would rather send patients to another doctor rather than doing the process themselves.
“We want to make contraception use as simple as possible for youth,” Di Meglio says. “We want providers of all sorts to have contact with youth to facilitate the use of contraceptives and we’re encouraging also discussion before people are even sexually active. We also want to encourage providers to encourage parents to have those conversations so that parents are then in the loop as much as possible so that they too can encourage young people to use effective contraception.”











Comments
Want to discuss? Please read our Commenting Policy first.