By now, you’ve likely seen a naloxone kit.

It’s a small, zippered black case marked with a grey or red cross that holds a syringe and a life-saving drug that can instantly reverse an overdose.
With more than 1,100 people dead of suspected overdoses in B.C. this year, CKNW’s Niki Reitmayer approached health workers to learn just how the kits work.
LISTEN: How to use naloxone
CKNW met with Neil Henderson, a clinical psychotherapist at Vancouver’s Commercial Health Centre, one of many clinics hoping to educate the public on how to use naloxone to slow the mounting body count amid the overdose crisis.
The drug, he said, is not a magic bullet — and that in the case of an overdose, the most important thing anyone can do is call 911 and start administering First Aid.
“Getting people to the hospital is key,” he said.
But once the call is made, bystanders can be the difference between life and death if they know how to use a naloxone kit.
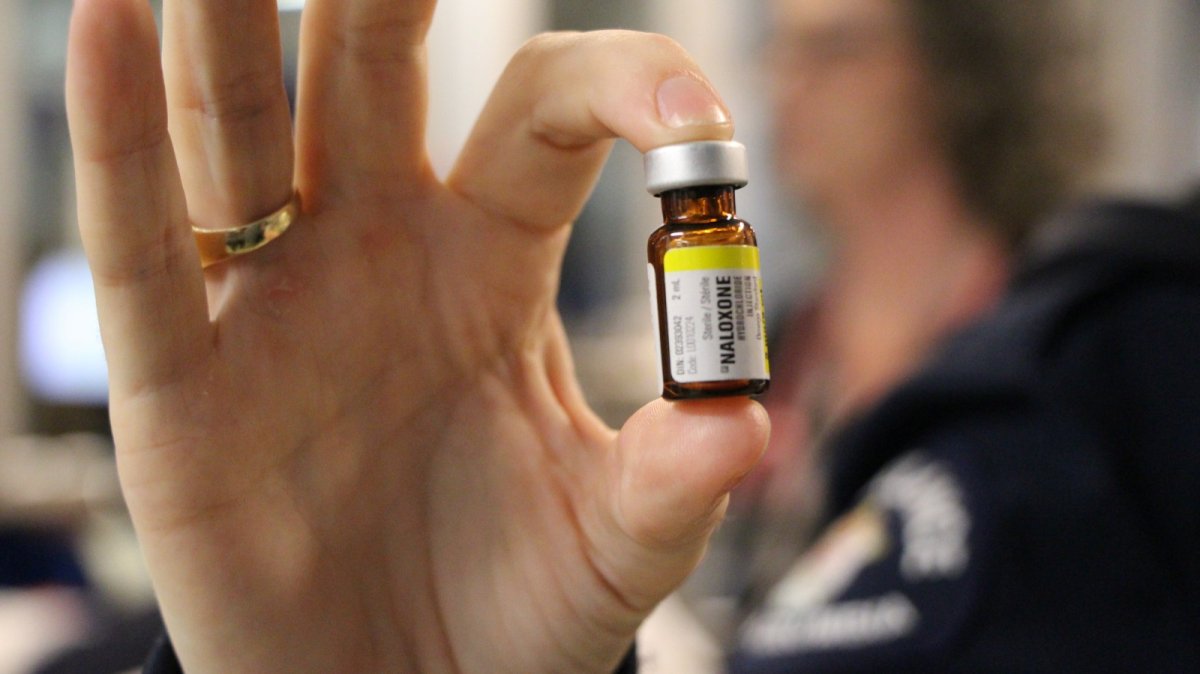
Inside the kit are three packaged needles, disposable blue gloves, a surgical mask and three glass vials of naloxone, sometimes referred to as narcan.
Before using naloxone, it’s important to be sure the subject is having an opioid overdose, Henderson said.

Get weekly health news
“It’s largely contextual,” he said. “There’s a really, really high chance that you will know — or somebody will know — that they have been using a drug and that they are overdosing.”
In that case, the victim will appear cold and clammy, with discolored skin, decreased respiration and a weaker heart rate, he explained.
“And if you determine that it is required, then you simply go through this process of administering the naloxone. It’s very, very straight forward.”
The process works like this:
- Remove a needle from its plastic packaging
- Open the vial of naloxone. Some vials may not have a lid, and instead need to be snapped in half
- Draw the medication into the syringe, then push the plunger in slightly to force out any air
- If possible, use an alcohol wipe to disinfect the spot where the injection will happen
- Insert the needle into the subject’s upper arm, thigh or buttocks at a 90-degree angle
- Inject the entire dose of naloxone
Henderson said you can push the needle in through the subject’s clothing if need be.
“It really is that straightforward and that simple,” he said.
“All we’re going to do is inject somebody. We’re going to inject into the thigh, the buttock, or the shoulder – just the fleshy areas of the body.”
Of course, there is no substitution for hands-on instruction, and people can find training if they want it.
“We are here and we are making a difference in the community,” said Nirmala Raniga, an opioid addiction expert and founder of the Chopra Addiction & Wellness Centre, which works in connection with Henderson’s clinic.
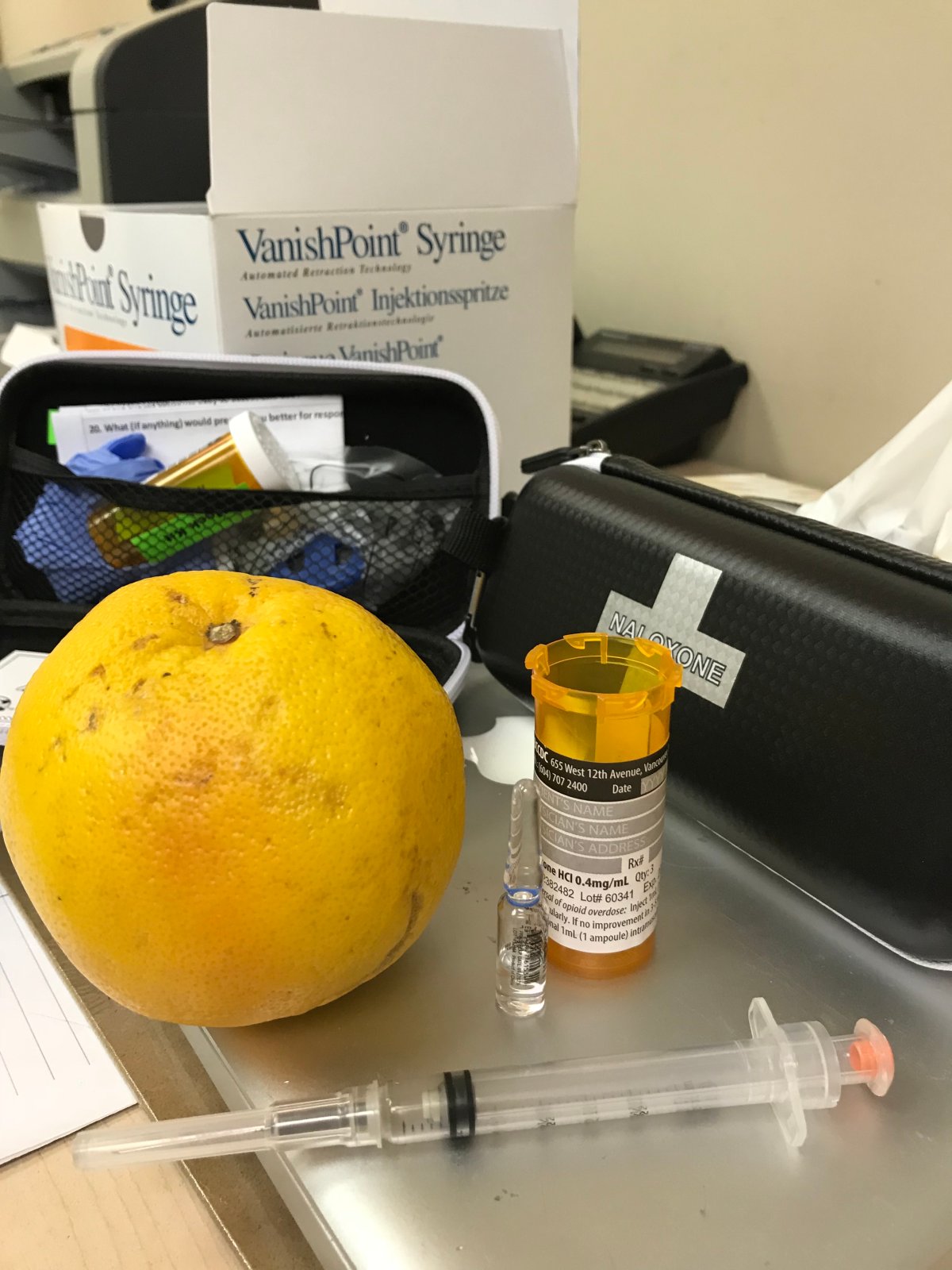
Each demonstration begins with an educational video.
Trainees are then presented with the contents of a naloxone kit and an orange, which is used to simulate an overdose victim’s arm during the demonstration.
The need for such life-saving treatment just keeps growing.
There was a 31 per cent increase in the number of drug overdose deaths in September, 2017 compared to the same period the year prior.
“Drugs are so much stronger now,” said Michelle Ibaraki, a former heroin addict who now works as an artist creating her own greeting cards.
She is a client at the methadone clinic, as well as a spokesperson for treatment.
“That’s why it’s great that they’re giving the naloxone kits out now and making people more aware, because it is such a crisis right now.”
You can find out more about where to get naloxone or naloxone training here.
- ‘Deeply ashamed’: Canadian Medical Association apologizes for harms to Indigenous peoples
- Kate Middleton marks quiet return to work following cancer treatment
- Health Canada gives 1 year to remove BVO from drinks. What are the risks?
- Never heard of eastern equine encephalitis? Cases are ‘likely underreported’














Comments