In theory, abortion is a publicly funded medical service like any other.

In practice, it’s far more complicated.
In the wake of a fatal mass shooting at a Colorado clinic, as a new government takes the reins and as a new abortion pill rolls out next year, Global News took a closer look at who gets access to abortions — and who doesn’t.
ABORTION FOR SOME: Access still depends on who you are and where you live
Where can you get an abortion? It’s a secret
How the ‘abortion pill’ Mifegymiso could change reproductive health
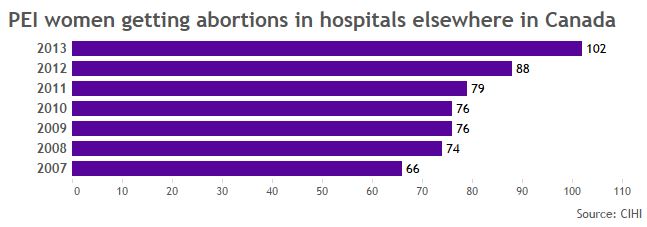
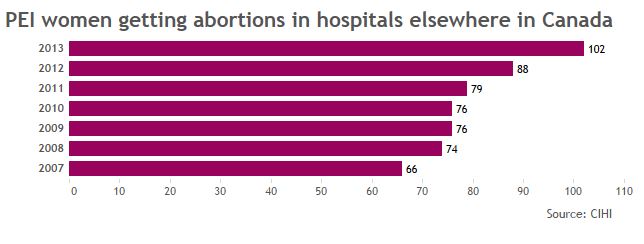
PEI has no clinics. The province will cover the cost of your abortion in a select few hospitals out of province, if you find a physician to refer you, but won’t cover the cost of your getting there.
In 2013, the most recent year for which we have data, at least 102 PEI residents left their home to get abortions in hospitals out of province. Many more sought out clinics, paying out of pocket for the trip.
This past January New Brunswick removed two of the most restrictive parts of its abortion rules: the requirements that two doctors approve a woman’s abortion and that only specialists in obstetrics and gynecology perform the procedure.
But the province still won’t pay for abortions like Mary’s: She went to a clinic whose wait list was shorter than the eight weeks she’d have to wait to get a hospital abortion.
Global News contacted provincial health ministries in New Brunswick and PEI for comment. They haven’t responded but we’ll add their comment when they do.
Just about every other province will cover the cost of an abortion in a hospital or a clinic, but it can be trickier to get the cost of travel covered: Sometimes there are travel vouchers available but these can take time and you need to be referred by a family doctor or community nurse.
As of this past summer, a reciprocal billing agreement between provinces means you’re covered if you travel out of province for an abortion but only if you have the procedure in a hospital, not a clinic — even though both your home province and the province where you have the procedure done probably both publicly pay for clinic abortions.
Making abortions inaccessible doesn’t mean women who need them won’t get them: It just makes it more difficult, and more dangerous, for them to do so.
READ MORE: How the ‘abortion pill’ Mifegymiso could change reproductive health
There are huge gaps when it comes to the number of abortion-providing facilities per woman:
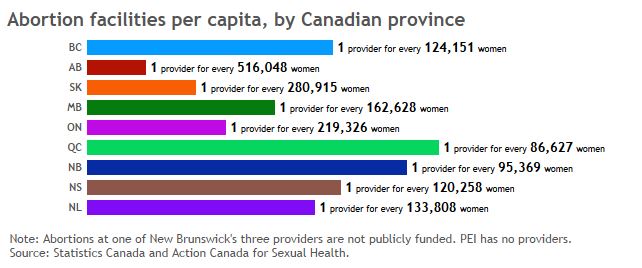
…and per square kilometre in a country defined by yawning stretches of wilderness and remote, rural communities:

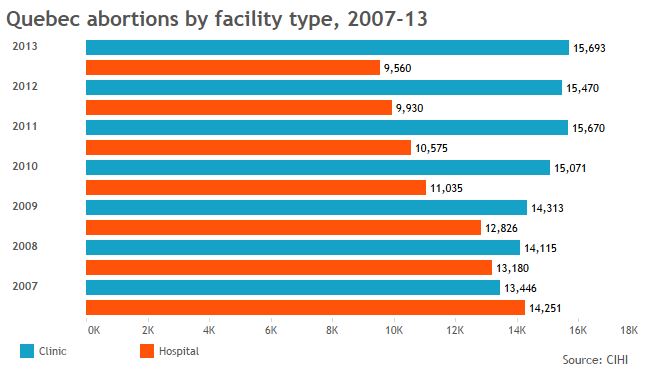
But the rate of hospital abortions per capita is especially high in some of the provinces where access is toughest, Global News analysis shows:

The cost and complexity tend to affect the most vulnerable women the most.

Get weekly health news
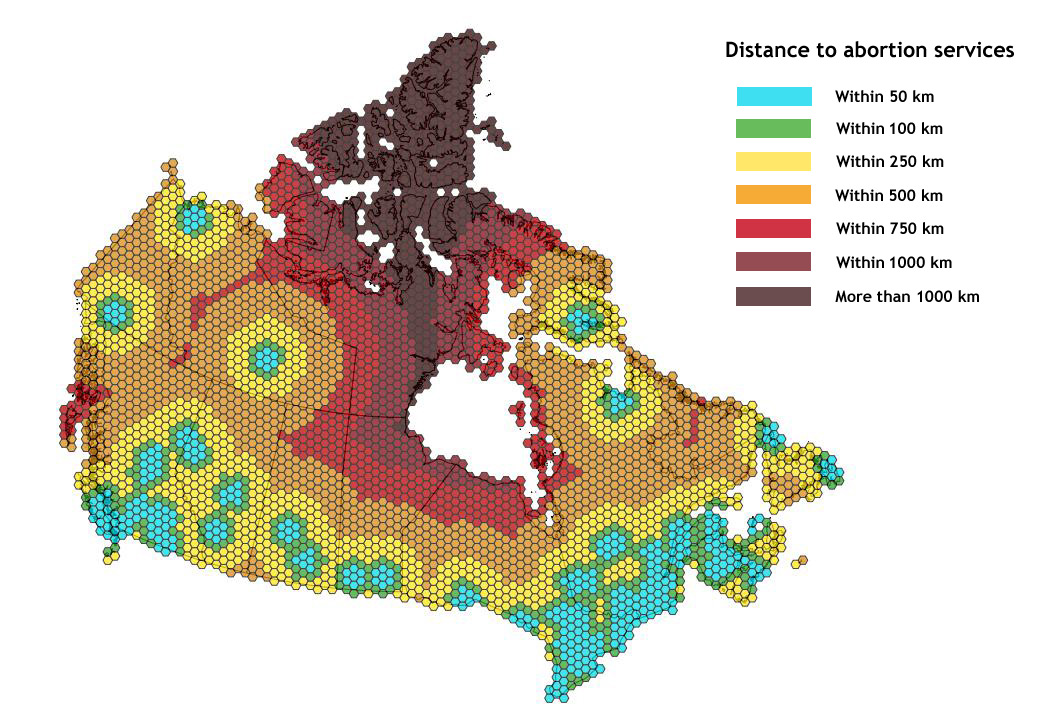
“The further a woman has to travel to access abortion, the less likely she is to obtain one and the more likely she is to be young and underprivileged,” a a 2012 study finds.
Between 2003 and 2006 the percentage of Canadian hospitals providing abortions actually dropped, from 17 per cent to 15.9 per cent.
In some cases, even women who live relatively close to a hospital will bypass it in favour of a clinic, says University of Ottawa women’s studies professor Christabelle Sethna.
Sethna has spent years studying the “accidental tourists” of Canada’s health care system — women of all ages, ethnicities and backgrounds who find themselves travelling far from home to get abortions.
Sethna and Marion Doull studied the often circuitous route women take to freestanding abortion clinics. In many cases, women lived relatively close to abortion-providing hospitals but eschewed them to travel farther to clinics instead.
Could be misinformation. Hospital wait times. The need for a clinic’s anonymity.
“We need more hard data,” Sethna said.
But one way or another, women who need to are terminating pregnancies.
- 3 clam fishermen die off coast of Savary Island when boat capsizes
- Saskatchewan’s hospital safety review expected to cost $1 million
- Saskastchewan Roughriders prepare for first CFL game in Saskatoon in 35 years
- ‘Completely ridiculous’: $547,000 in B.C. government funding for 2 tenants in Vancouver SRO
In some cases, especially in places like Prince Edward Island where abortion access is scarce, it’s resulted in the kind of nightmarish attempts at do-it-yourself abortions that seem to belong to another era.
“A woman that’s pregnant and doesn’t want to be will do anything she needs to do to terminate the pregnancy,” says Patricia LaRue, director of Gatineau’s Clinique des Femmes.
LaRue counts staunch anti-abortion activists among her clients. One woman who protested outside her clinic daily called out of the blue: Her daughter needed an abortion immediately.
“We do have women coming here to the clinic, saying, ‘I’ve always been against abortion but now I need one.'”
Going through the procedure themselves doesn’t always change their mind, she said.
Days after her daughter’s abortion, that protesting mother was back outside the clinic, placard in hand.
“It’s really difficult when they move on and say, ‘Well the other women that needed the abortion in the clinic didn’t really need it. But I really did.'”
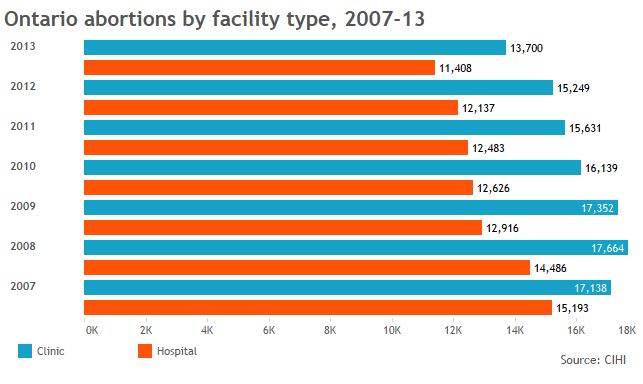
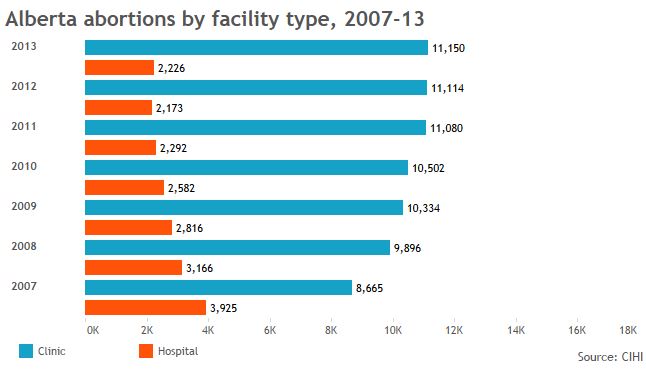
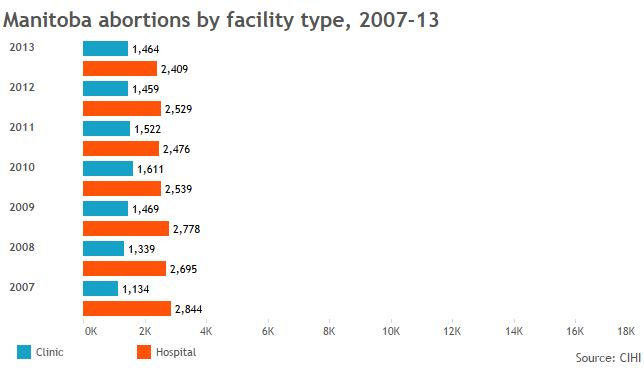
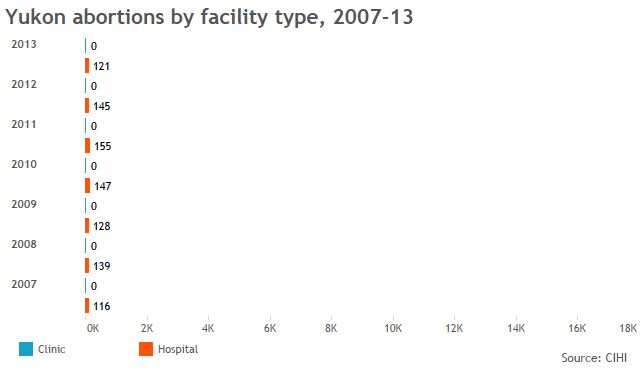
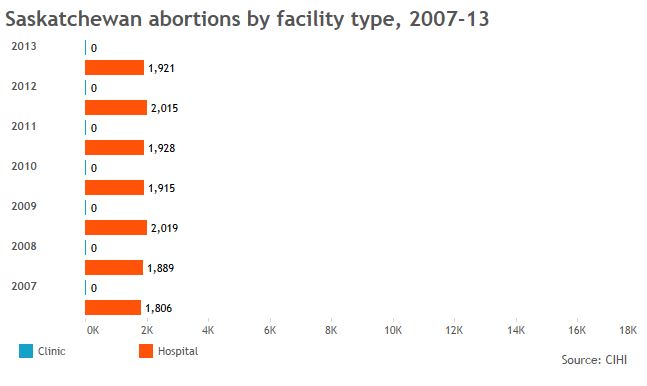
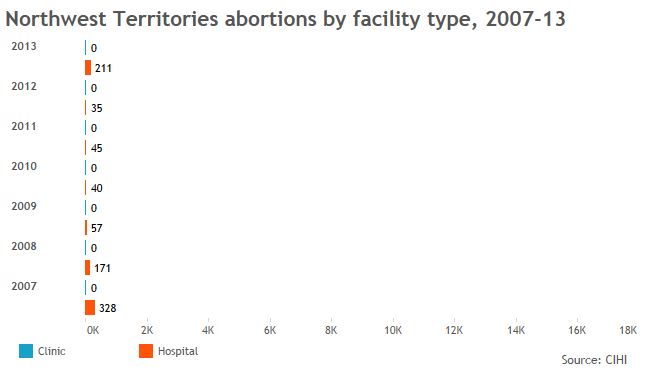
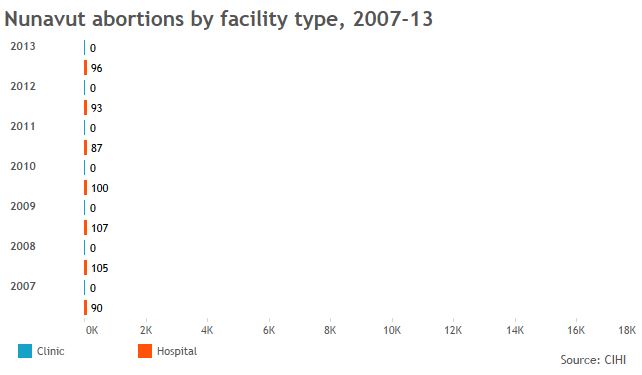
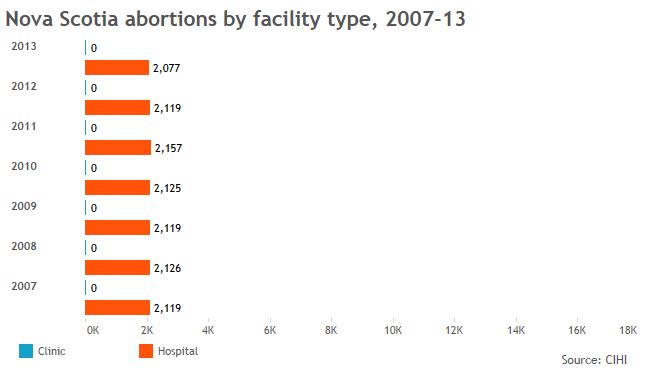
Global News used data from the Canadian Institute of Health Information to create the graphics below and provide a sense of who’s getting abortions in jurisdictions across Canada, and in what kind of facilities.
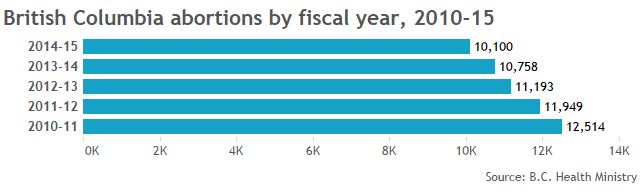
More telling than the numbers we got, though, were the numbers that are missing: Clinic data is incomplete across the board; B.C. doesn’t break down abortions by facility type for fear its facilities will be targeted. So Global News got totals from the province’s health ministry.
The stats we have show a continuing need for abortion services but one that’s declined, year on year, in many parts of the country — thanks, some have said, to better sex education and contraceptive access.
The data also show that, when clinics are available, more women tend to go to them. That’s borne out in research showing some women will travel to clinics rather than seek services in hospitals nearby.
GALLERY: Click through to see abortion statistics in Canadian provinces and territories.
Note: Canadian Institute of Health Information gets its data from provinces, not all of which report complete figures for abortions provided in clinics.

























Comments
Want to discuss? Please read our Commenting Policy first.