Canada’s smaller communities are being hit hardest by the overdose crisis with hospitalization rates for opioid poisoning that are more than double those of larger cities, according to a new report.

The analysis from the Canadian Institute for Health Information looked at opioid hospitalizations across the country in 2017 and found communities of 50,000 to 99,999 people had rates that were 2.5 times higher than cities with populations over 500,000.
READ MORE: How lethal opioids devastated a small region of Ontario
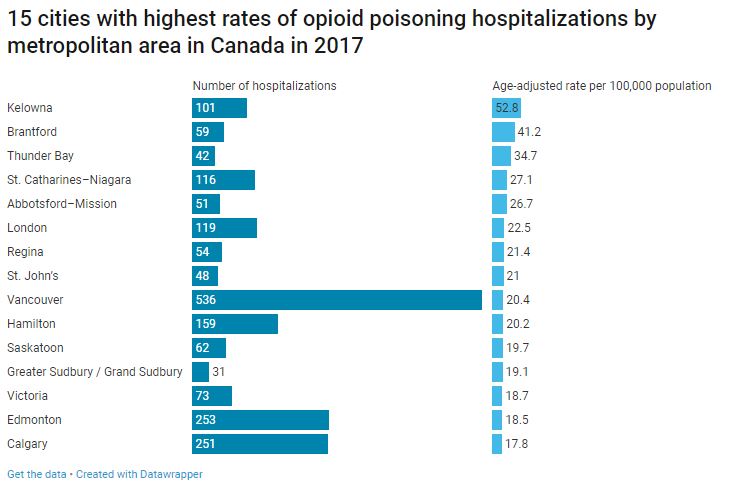
Smaller B.C. cities like Nanaimo, Prince George and Kelowna or Ontario cities like Brantford and Belleville had the highest age-adjusted rates per 100,000 people, according to data broken down by census subdivision.
When looking at the larger metropolitan data, Kelowna, Brantford and Thunder Bay had the highest rates per 100,000 people. Kelowna, for example, has a hospitalization opioid overdose rate of 52.8 per 100,000 while Vancouver has a rate of 20.4 per 100,000 when adjusting for age.
Opioid poisoning occurs when a wrong dosage is taken, it’s combined with another drug or alcohol, or if it was illegally obtained, according to CIHI researchers. The surge in overdose deaths nationally that has killed more than 9,000 since 2016 has largely been attributed to the rise of illicit fentanyl and other powerful synthetic opioids.
Across Canada, the fastest-growing rates of hospitalizations due to opioid poisoning were seen among males age 25 to 44. Other findings from the analysis show the rate of hospitalizations for neonatal opioid withdrawal symptoms increased by 21 per cent between 2013 and 2017.
WATCH: Fentanyl kings in Canada allegedly linked to powerful Chinese gang, the Big Circle Boys
And 17 Canadians were hospitalized per day for opioid poisonings in 2017 — a 23 per cent rise from 2013.

Get weekly health news
For Dr. Jeff Eppler, who works as an emergency department doctor at Kelowna General Hospital, the findings are confirmation of a public health crisis that killed almost 4,000 Canadians in 2017.
“It’s truly unbelievable how many overdoses we have been seeing over the past couple of years,” Eppler told Global News. “I’ve probably seen more overdoses in the last year or two than the last 25.”
“What we see is just the tip of the iceberg of the people that are dying out. Most people who fatally overdose don’t even come in to emergency.”
READ MORE: 2,066 Canadians died of opioid overdoses in the first half of 2018

The report does not say why Canada’s smaller communities are being hit harder by opioid overdoses, but Dr. Eppler has his theories.
“There are more and more people that are suffering from socioeconomic factors like job losses and increased marginalization,” he said. “I think people have started self-medicating depression with opioids.”
Dr. Malcolm Lock, the medical officer of health with Ontario’s Brant County, said while Brantford saw higher overdose rates — roughly 40 per 100,000 in 2017 — the numbers have fallen significantly in 2018 to 3.3 per 100,000, according to figures from the Brant County Health Unit.
Lock said emergency department calls and visits for opioid-related overdoses have all gone down, including deaths.
“2018, we are back now to provincial averages,” Lock said. “We have aggressively increased our naloxone kits and put a lot into education.”
“We can’t prove any association but it’s really the biggest thing we can think of that’s made a major difference to our stats.”
Looking at the national picture, hospitalization rates for opioid overdoses have increased in provinces like Newfoundland and Labrador, Ontario, Manitoba and British Columbia, but have decreased in provinces like Saskatchewan, Nova Scotia, P.E.I and New Brunswick, according to CIHI.
WATCH: How the opioid crisis affects children left behind

CIHI’s analysis shows a Canada-wide decrease in opioid-related hospitalizations for the last three months of 2017 and the first three months of 2018.
Researchers with CIHI attributed the decreases in part to a number of Canada wide initiatives that included new opioid prescribing guidelines, an increase in the number of supervised consumption sites and better provincial prescription monitoring.
“We are seeing a lot of positive initiatives put in place and it does take time for the data to reflect that,” said Krista Louie, manager of opioid reporting with CIHI. “Between the end of last year and the beginning of this year, we are seeing a slight decrease nationally. We can’t know for sure whether that trend will continue but it is a positive.”
However, new numbers from the Public Health Agency of Canada showed more than 2,000 Canadians lost their lives to apparent opioid overdoses in the first half of 2018 — or more than 11 people a day. Of the deaths reported between January and June, 94 per cent were the result of accidental overdoses and 72 per cent involved fentanyl-related substances.
“This indicates the continuing role of fentanyl contamination of the street drug supply in this crisis, highlighting the vital importance of increasing access to a safer supply of drugs to prevent death and other harms,” the health agency said in a statement.
READ MORE: If helping China hunt fugitives is the price of stemming deadly fentanyl flow, should Canada pay?
In B.C., 734 people died of opioid-related overdoses while Ontario saw 638 deaths and Alberta saw 379. The new numbers also showed that life expectancy in Canada, which increased by almost three years between 2000 and 2016, has slowed partly due to the dramatic rise in opioid-related deaths.
“When I see these numbers its certainly very tragic,” said federal Health Minister Ginette Petitpas Taylor. “I’m hopeful that if we continue to work together that we’ll be able to turn the tide on this crisis. But it’s going to take time, it’s not going to be done overnight. It’s my number one priority.”
CIHI’s analysis also looked at emergency department visits for opioid poisoning in Alberta, Ontario and Yukon and found that rates increased in Ontario 73 per cent from 5,958 to 8,834 and in 23 per cent in Alberta from 2,402 to 4,359.
Yukon increased from 37 to 122 but at a significantly higher rate of 101.9 per 100,000 people to 317.2 per 100,000 people. Due to the low volume reporting in Yukon, CIHI warns these trends must be interpreted with caution as they could be higher or lower.
WATCH: With 3,996 opioid deaths in 1 year, Canada hasn’t called a ‘public health emergency’
The five Ontario cities with the highest ED visits for opioid poisonings were Brantford, St. Catharines-Niagara, Peterborough and Barrie. The highest Alberta municipalities were Lethbridge, Red Deer, Medicine Hat, Wood Buffalo, and Grande Prairie.
The overdose crisis in Barrie and Simcoe County was recently profiled in a Global News’ multi-part series, Fentanyl: Making a Killing, that revealed the scale of the fentanyl trade across Canada.
On Monday night, MPs in Ottawa convened a debate on Canada’s opioid crisis that looked at solutions such as declaring a public health emergency or coming up with more funding for treatment beds.
The federal Budget 2018 set aside $231.4 million to tackle the crisis, with $150 million going to the provinces and territories to fight the overdose crisis, while opposition parties criticized the Liberals saying there needs to be more money for addiction and treatment services.





























Comments
Want to discuss? Please read our Commenting Policy first.