In a rural corner of P.E.I., a small hospital is trying a first-in-Canada approach to delivering care that could offer a solution to doctor shortages across the country.

Instead of a doctor doing hospital rounds in person, a nurse rolls in a TV cart with the physician on a video screen from an office elsewhere in the province or the country.
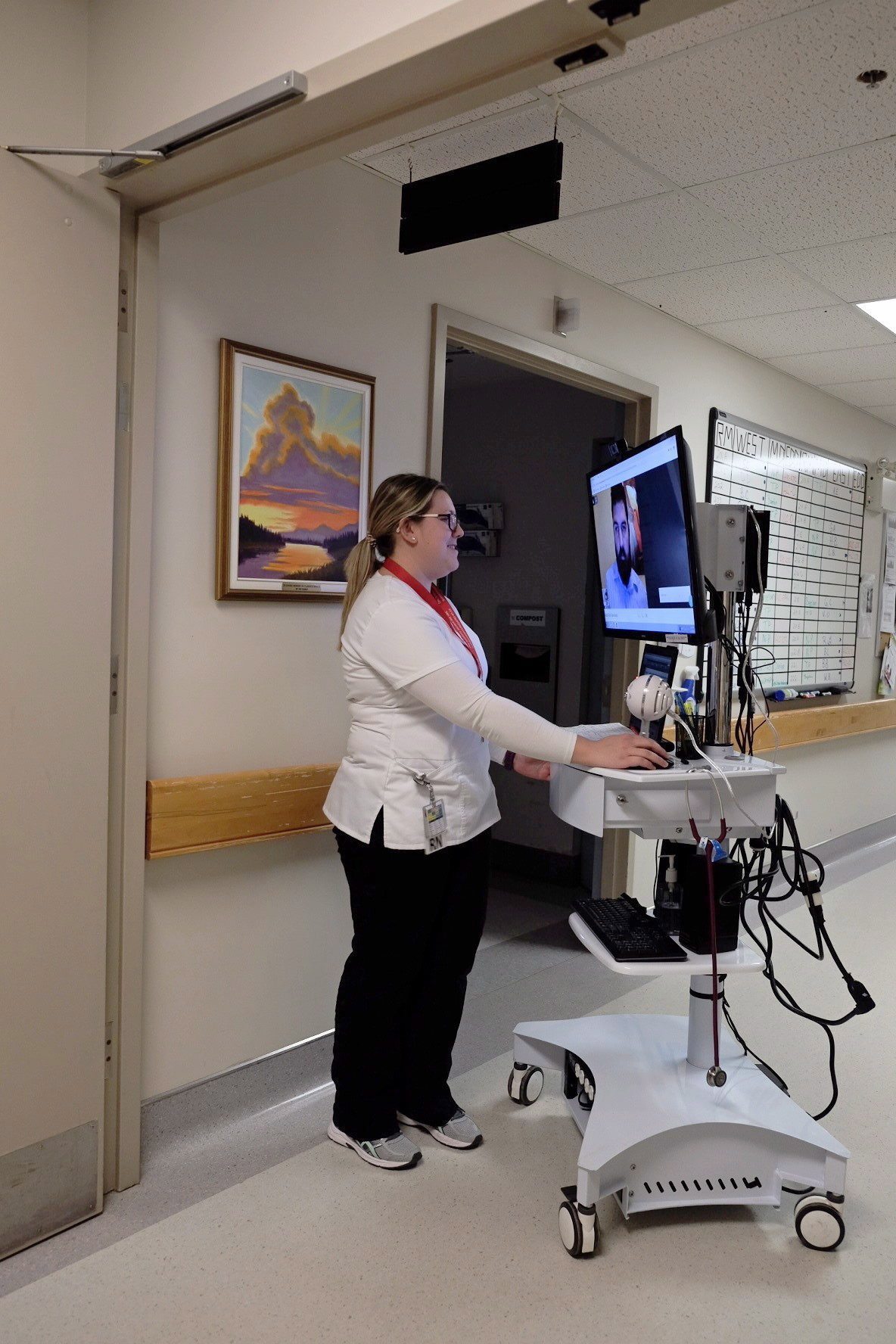
Western Hospital in Alberton, P.E.I., has undertaken a six-month pilot “tele-rounding” project – doctors treating patients via a secure video conference link. They can check on patients, review their files, order tests and even use a digital, bluetooth-enabled stethoscope applied by a nurse while a doctor listens remotely.
“There are no doctors on the floor there, but there are nursing staff and lab technicians. The nurse takes the cart from patient to patient, and we’re essentially doing hospital rounds technologically enabled and we’re providing physician care,” said Dr. Brett Belchetz, an emergency department physician and CEO of Maple – the Toronto company providing the tele-rounding service.
READ MORE: Kingston needs to pin down concrete numbers on doctor shortage, says medical consultant
Western Hospital approached Maple, which has a tele-medicine app used across Canada that gives people access to a doctor. Hospital officials hoped they could the technology for their patients who didn’t have a family doctor.
Now, Maple hopes that if the P.E.I. pilot is successful, they could use it elsewhere.
“There are doctors with excess capacity, and we’re allowing them to use that excess capacity to keep a rural hospital open,” Belchetz said.
“If you look at the Stats Canada numbers, only about 50 per cent of Canadian doctors work fully all year despite the great need we have for more care.”

Get weekly health news
Some 6.6 per cent of Canadians reported being unable to find a family doctor in 2010, with numbers substantially higher in some provinces.
Similar tele-rounding is already done in some parts of the U.S. and the U.K.
There are nine physicians participating in the tele-rounding pilot, including three physicians from Prince Edward Island and others from Nova Scotia and Ontario who are licensed to work on the Island.
Hospital administrator Paul Young said the pilot project is a stop-gap to help address vacancies with family physicians and avoid having to close the hospital, which is about 50 minutes west of Summerside, P.E.I.
He said since the pilot project was started, two new family physicians have been recruited to work at the hospital, starting early in 2019.
“Our patients and our communities place their trust in our ability to provide safe, effective, quality care on a consistent basis, regardless of the challenges we may be facing,” Young said.
Julie Gaudet recently spent 11 days in hospital in Alberton following surgery on her foot and says she was impressed with the tele-rounding system.
“I thought it made a lot of sense, especially being out in the country, and with the shortage of doctors here on the Island. I thought it was an excellent experience,” she said.
Gaudet, 67, said the doctors spent lots of time with her and asked lots of questions, and she quickly forgot that the doctor wasn’t actually in the room with her.
“They were right there in front of you on the TV screen. I could see them. They could see me. He had all my charts from 20 years ago. He knew all my medications. It was just top notch,” she said.
Young said most patients were a bit hesitant at first, but now they have patients asking for the “TV doctors.”
Since the pilot project began in August, more than 1,200 tele-rounding consults have been performed on nearly 60 patients over the course of their hospital stay.
Belchetz said the pilot project will be cost-neutral for the P.E.I. government – it won’t cost more than the province would have spent on having doctors there.
“Nobody is suggesting we run hospitals in the future with no doctors. When they get a full complement of doctors we’ll be happy to step back. But this can be used when doctors are sick or on holidays,” Belchetz said.
The pilot project will be reviewed in February.













Comments
Want to discuss? Please read our Commenting Policy first.