KENEMA, Sierra Leone — An Associated Press investigation has found that the World Health Organization and other responders faced avoidable obstacles in their efforts to stop the spiraling Ebola outbreak last summer in Kenema, a pivotal seeding point for the virus and a microcosm of the messy response across West Africa.

Their work was hampered by poor management, lack of basic protective gear and bureaucratic infighting, according to internal WHO emails, documents and AP interviews. Here are 10 critical mistakes:

1. Questionable chlorine: Unlike other aid agencies, WHO obtained the disinfectant locally in Sierra Leone. On several occasions, officials at Kenema Government Hospital discovered the chlorine had expired or that the containers had their tags ripped off and expiration dates were missing. In an email, WHO’s Sierra Leone representative called for a criminal investigation into the defective disinfectant, which is key to limiting exposure to the virus.
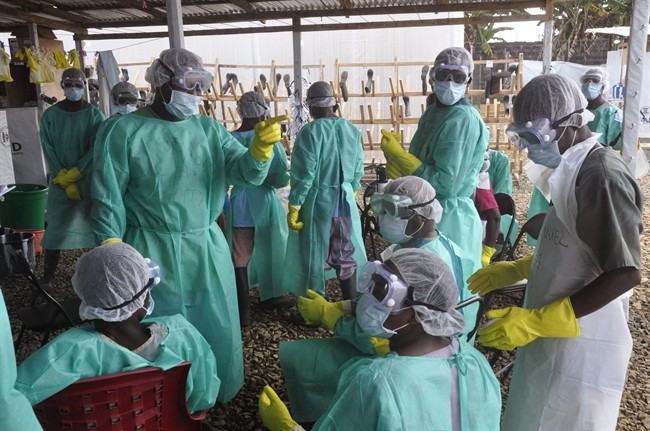
2. Health care workers at risk: More than 40 health staffers died; 20 were infected during the delayed construction of an Ebola clinic meant to relieve pressure on Kenema’s hospital.
READ MORE: New Ebola death in Sierra Leone 6 days after discharging last known patient
Many weren’t properly trained on how to use protective equipment and worked in an Ebola ward so dangerous that aid agency Doctors Without Borders called for its closure.
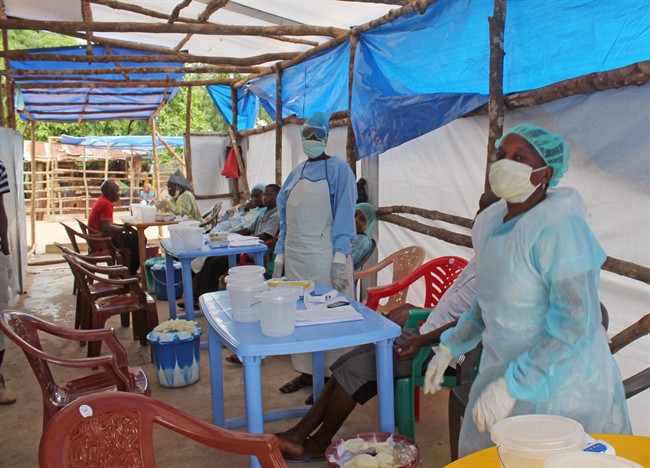
3. Delayed construction: The Red Cross offered to build an Ebola clinic in Kenema, but no one in Sierra Leone’s government or WHO could tell them where to build it. By the time it opened, the outbreak in Kenema already had peaked.
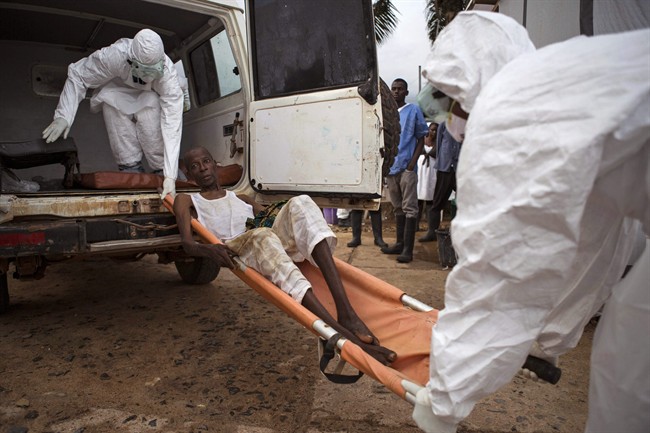
4. No body bags: At the beginning of August 2014, an internal WHO report noted “supplies of body bags have completely run out,” vital information since the bags limit exposure to the corpses of Ebola victims, which are highly contagious. Later that month, an aid official attempting to arrange delivery of about 100 body bags to Kenema was stymied for hours by government bureaucracy. After finally being released, the bags were delayed yet again — this time overnight — when the driver couldn’t reach a sleeping police superintendent for clearance through a checkpoint.

5. Tight-fistedness: WHO responders were so constrained by bureaucracy that Director-General Dr. Margaret Chan intervened, writing in an email that logistics experts in West Africa were getting only a couple hundred dollars a week to cover thousands of dollars in expenses for basics like protective rubber boots and disinfectant.
READ MORE: Blood, sweat and tears: U.S. doctors launch 5-year study of Ebola survivors in Liberia

Get breaking National news
6. Shaky power supply: A generator being used by WHO at the hospital’s laboratory was so unstable one expert feared it might damage the equipment and alerted his colleagues to the potential problem in an Aug. 4 email. The problem was not dealt with and, four days later, the laboratory was hit by a blackout.

7. Weak leadership: WHO officials on the ground in Kenema repeatedly called on their superiors to intervene, warning that the agency’s failure to seize control meant it was being sidelined.
8. Doctored data: A WHO outbreak expert noted in an email that the U.N. agency’s official count of Ebola cases was being altered by a Sierra Leonean official to match his government’s statistics, a practice that spread confusion back in Kenema.

9. No transportation: Despite a fleet of more than 50 new Land Cruisers parked at U.N. headquarters in Freetown, Liberia, WHO responders didn’t have enough vehicles to track the spread of the virus. One WHO official suggested that Sierra Leonean responders requesting motorbikes for travel to villages buy bicycles instead.

10. Infighting: Philippe Barboza, WHO’s Ebola coordinator in Kenema, described the tension between his agency and the U.S. epidemic monitoring company Metabiota as verging on “open conflict” and deteriorating so much he recommended WHO’s outbreak team be pulled from the city.


Comments
Want to discuss? Please read our Commenting Policy first.