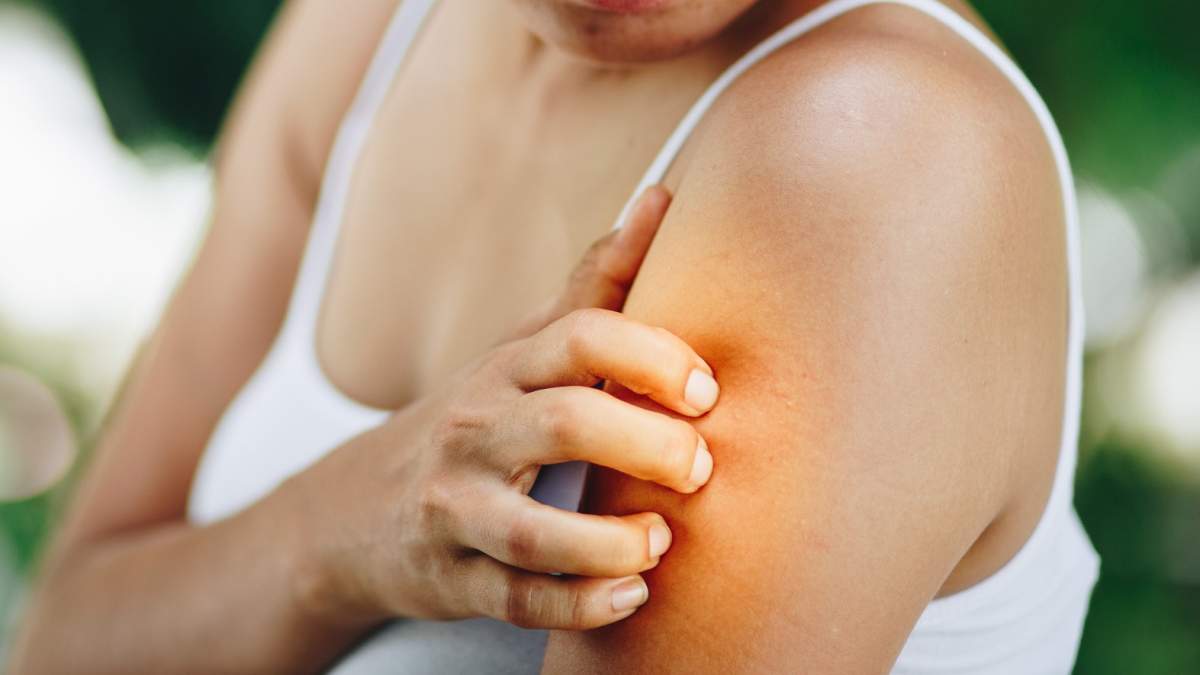
When Lesley-Anne was young, she suffered from eczema, having rashes on her legs and arms. Her symptoms lessened over time until they were only small patches, but in late adulthood, her eczema came back with a vengeance. This time, it also appeared on her face — and was now visible to the world.

“It was really bad. All around my eyes, my eyelids, my lips, my earlobes, my chest and even my hands,” she says.
A new report from the Eczema Society of Canada (ESC), called the Atopic Dermatitis Patient Journey, examines the experience of living with atopic dermatitis (AD), the most common form of eczema. The report details the journey that AD patients go through from symptom onset to diagnosis, treatment and beyond.
The Atopic Dermatitis Patient Journey is based on a survey of 1,057 AD patients and caregivers across Canada, as well as in-depth interviews and a focus group. It shows that people like Lesley-Anne aren’t alone in their struggle with the condition, and that more support and understanding is needed.
Eczema can be a painful journey
Lesley-Anne, who preferred not to use her last name, didn’t always struggle with her condition, but after her AD returned later in life, it was a long and challenging process to find relief. She started with topical medications and various tests, and visited a dermatologist to try to pinpoint the cause of her flare-ups.
“They diagnosed me fairly quickly with eczema,” she recalls. “But they also wondered if there were other factors at play due to the way my eczema presented. I had all that testing done, but I still suffered, and the eczema was still front and centre and just kept getting worse. My eyelids and different areas of my face were so affected — they felt like they were on fire.”

Get breaking National news
She says she would use ice packs for relief and would cover her red, raw skin by wearing sunglasses when she was out with friends. The pain and incessant itch affected her sleep, and on workdays, her eyes were so swollen when she woke up that she would have to get up early to get ready on time.
READ MORE: From sleep to self-esteem, eczema affects more than your skin
Finding relief from eczema flare-ups
According to the Atopic Dermatitis Patient Journey, 41 per cent of adults with AD are in a constant state of flare, where the skin is intensely itchy and raw, and can crack, ooze and bleed. Although their symptoms can improve, they never experience periods of fully clear skin.
Meanwhile, nearly half of adults with AD have had a flare-up so bad they considered it a crisis that required immediate medical attention. In addition, 37 per cent of adult patients and 42 per cent of caregivers surveyed for the report shared concerns that patients won’t actually be able to see their health-care provider during a flare.
“The Atopic Dermatitis Patient Journey started because we recognized that Canadians, including health-care providers and government decision makers, don’t necessarily have a full understanding of what the patient journey looks like across a lifetime and what patients go through day to day in trying to manage this unrelenting condition,” says Amanda Cresswell-Melville, executive director of ESC.
“For some patients, they suffer from the time they wake up in the morning until the time they go to bed — living with unbearable itch, pain and discomfort. Some experience severe cracking and oozing on areas like their joints, making them unable to extend their arm. This makes simple things like movement or exercise impossible. A lot of people don’t understand that the disease can be that severe and that debilitating.”
READ MORE: An eczema diagnosis can often mean more than itchy skin
Many patients face challenges getting care
Topical medications have traditionally been the mainstay of AD treatment, and only recently has there been more research and breakthroughs in new therapies. These advancements are especially important for patients who find their symptoms do not improve even after trying various topical medications.
AD is a spectrum condition for which there is no cure. For many, it is a mild to moderate condition that can be managed with topical treatments and lifestyle modifications. For patients living with moderate to severe forms of AD, however, the condition can be debilitating and life-altering.
“Despite my medications and doctor’s appointments, my skin wasn’t getting better. In fact, it was getting worse and worse. I was trying everything, and it was getting more stressful and affecting more and more parts of my life. It became intense, unpredictable and challenging all around,” Lesley-Anne says.
Because she lives near Toronto, Lesley-Anne was able to seek the medical attention she required without long wait times, which can be common for those who live in more remote regions of Canada. After years of painful flares, she finally found control over her condition by working in partnership with a doctor who was willing to listen, walk her through her treatment plan and make adjustments in her regimen to help her find relief.
In addition to fostering empathy and understanding for those who live with AD, ESC is also working to mitigate current gaps in care by providing education and support to health-care providers. “Part of our mandate is to help support primary care providers, so that patients can get the best care they can at all care levels,” Cresswell-Melville says.
For more information and to read the Atopic Dermatitis Patient Journey, visit Eczema Society of Canada.