An elderly man in Northern Ireland came to the emergency room complaining of weakness in his left arm and a recent history of falls and trouble with his balance.

Doctors were surprised to discover the cause – a large air pocket in his skull where part of his brain should be.
“We immediately realized there was something significantly abnormal about the images, even before our specialist radiology team had given us the formal report,” said Dr. Finlay Brown, a general practitioner trainee in Belfast, who was one of the doctors on call at the hospital at the time, in an email.
“We thought that this was a pocket of air but were not sure how it had got there!”
Brown and co-author Djamil Vahidassr described the case in an article published in BMJ Case Reports in February.
The article says that an 84-year-old man was referred to the emergency department after he had been complaining of recurrent falls. He was otherwise in pretty good health for his age – he didn’t smoke or drink much, he was independent and he could still do physical activity.
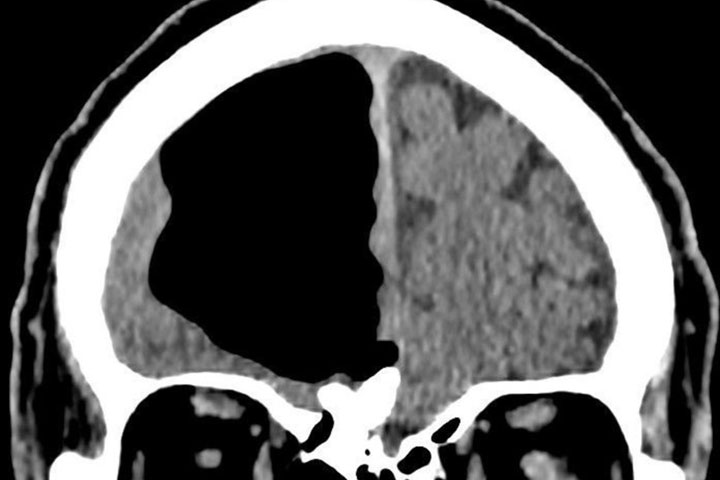
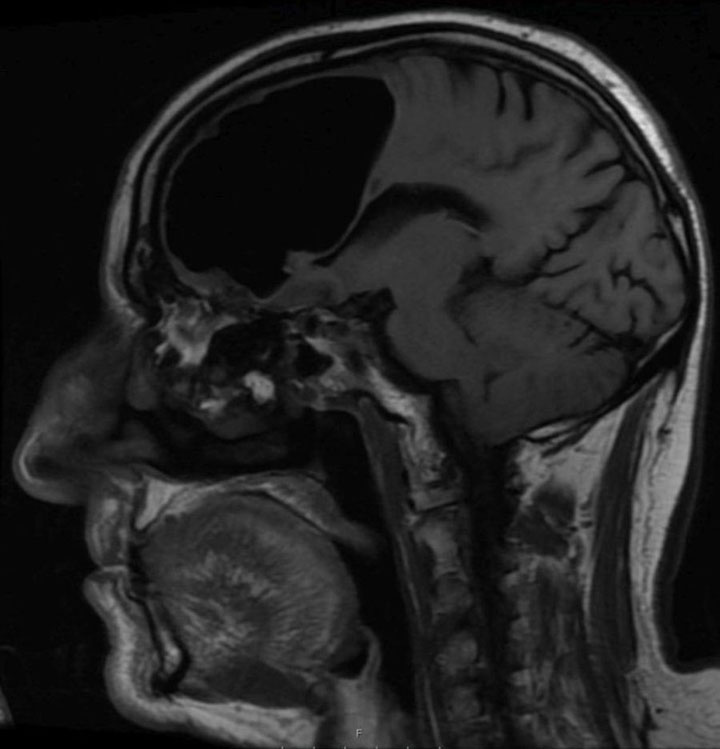
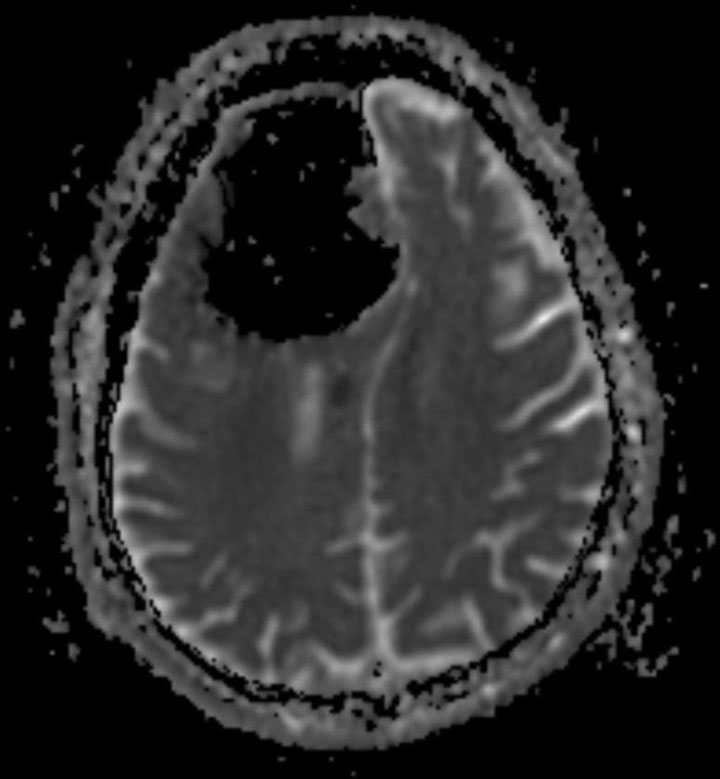
A CT scan revealed a nine-centimetre air-filled cavity in his right frontal lobe, looking like a big black blank area on the scan.

Get weekly health news
This was due to an “ethmoidal osteoma,” which Brown explained is a slow-growing bone growth in his sinus. It eventually eroded through the base of his skull cavity.
“It had formed a ‘one-way valve’ effect that would allow air to get through into the skull but wasn’t able to get out. This caused a build-up of air under pressure insidiously over months to years,” he explained. Air was able to get into the man’s skull through the sinus, and then was trapped there.
As more air got in, it slowly pushed the brain aside, said Brown. It pushed and compressed the brain, a soft organ, to make room for the air. And as this happened, doctors believe the pressure may have caused a small stroke due to lack of blood flow to that part of the brain.
“In theory if the pressurized cavity was relieved the brain would shift back into its normal position,” Brown said.
Doctors placed the man on medication to reduce the risk of further strokes. He was also offered surgery to decompress the air pocket and to remove the bone growth from his sinus. However, after the patient and his family discussed the risks, they decided not to have the surgery.
Instead, the patient was placed on secondary stroke prevention and eventually sent home. In his follow-up appointment 12 weeks later, the weakness on his left side appeared to have resolved.
He was “much improved” said Brown, despite still having a big empty space in his skull.







Comments
Want to discuss? Please read our Commenting Policy first.