When the birth control pill came out in 1960, it was revered for liberating women. Unlike their mothers before them, an entire generation of women was able to enter the workforce and blaze a career trail for themselves without being roadblocked by an unplanned pregnancy.

Yet, unintended pregnancies still hover around 60 per cent in Canada, according to the Society of Obstetricians and Gynaecologists of Canada (SOGC), and men and women alike use withdrawal as one of the top three forms of birth control. The other two are the pill and condoms. These results were drawn from a 2016 survey of 3,200 Canadian women.
WATCH BELOW: IUD baby goes viral after holding birth control device in hand after birth

The SOGC also noted that many women “know very little” about IUDs, despite the fact that they’re one of the most effective methods of contraception available.
“Fifty per cent of women said they didn’t know anything about IUDs and few had any specific knowledge,” says Dr. Jennifer Blake, CEO of the SOGC. “We don’t know if doctors aren’t informing their patients or if there’s some other failure of awareness, but women are not aware of how effective IUDs are and how they can be used.”

Get weekly health news
What is an IUD?
An acronym for intrauterine device, IUDs are long-acting reversible contraceptives (LARCs) that are inserted into the uterus by a physician. They are up to 99.4 per cent effective at preventing pregnancy, and can remain in your body from three to five years (depending on the type of device).
In fact, Blake says, “they’re a more effective form of birth control than tubular sterilization.”
How does it work?
There are two types of IUDs: hormonal, which is made from plastic and releases a small amount of the hormone progestin, and non-hormonal, which is made from copper.
The former increases the amount of cervical fluid released every month and makes it thicker, thus making it difficult for sperm to enter the uterus. The latter works because the copper creates a non-habitable environment for a fertilized egg to implant in the uterus.
READ MORE: Birth control for men: Is there gender inequality in health research?
In both cases, the fact alone that there’s a foreign object in the uterus makes it less likely to get pregnant.
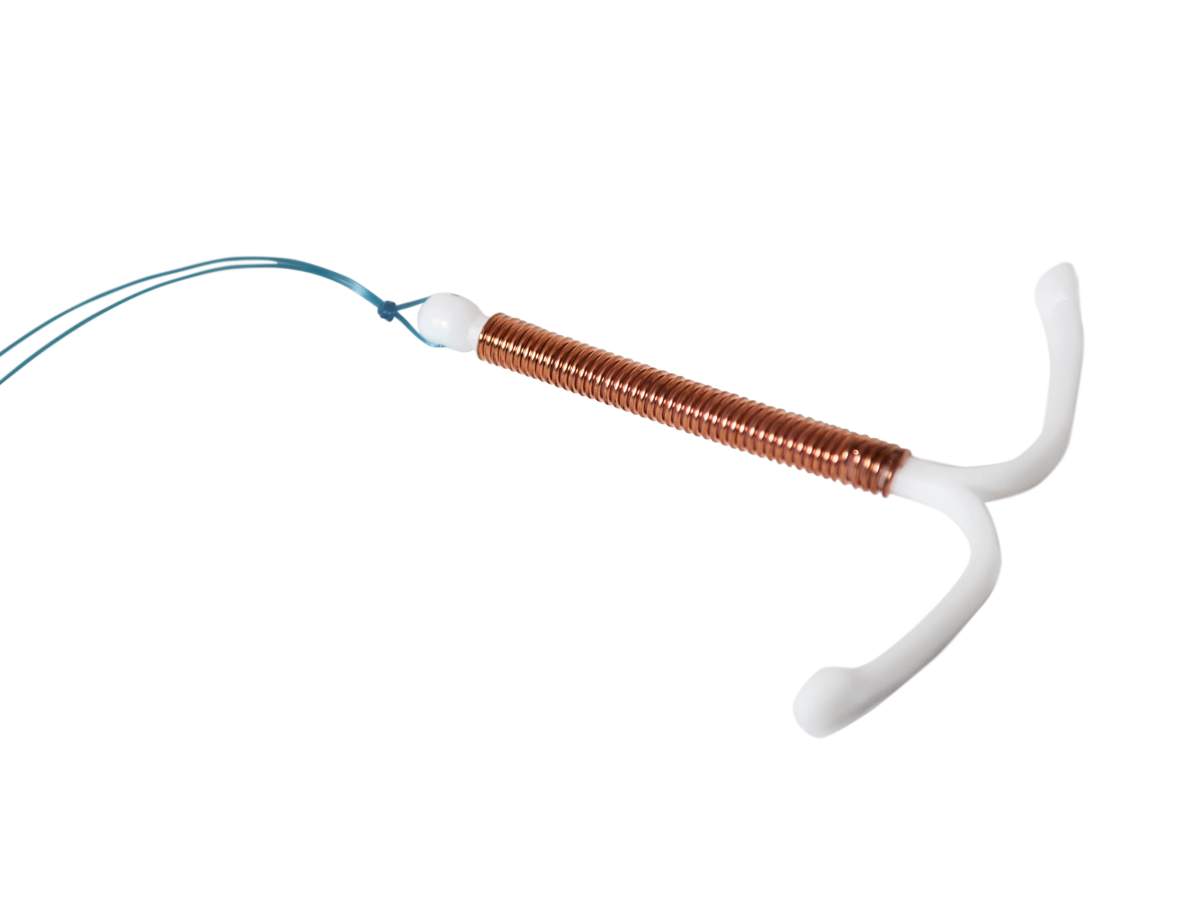
What does it look like?
An IUD is a T-shaped device that is inserted by your physician. There’s a small string at the end of it that extends to the vagina, making it easy for women to ensure it’s still in place.
It has to be removed by your doctor, as well.
How does it differ from the pill?
“Women who are allergic to synthetic estrogen can safely use an IUD, as well as women who smoke,” since smoking while taking oral contraceptives has been shown to increase the chances of blood clots and stroke, says Katymay Malone, a health education specialist and visiting instructor at Mississippi University for Women, in Columbus, Miss.
Plus, once an IUD is inserted, you no longer have to think about birth control — “the pill is easily forgotten,” Blake points out.
And according to Dr. Deborah Ottenheimer, an OBGYN at Ottenheimer Health Care in New York, “studies show an IUD is 99 per cent effective at preventing unplanned pregnancy,” she said to Women’s Health Magazine. The pill, on the other hand, has a roughly 92 per cent success rate.
What are the drawbacks to an IUD?
The birth control pill will lighten a woman’s period, whereas that effect depends on which IUD you use. In one class, Blake says, your period can get really light, while in another, it could get heavier.
READ MORE: Male birth control study halted due to ‘mood swings’ in participants
Malone says some women report increased cramps and back aches, and there have also been cases of it slipping out, although these are very rare.
“One of the biggest concerns is that women are worried about having a foreign object inserted through their cervix into the uterus,” Malone says. “There are a range of experiences, from those who say they didn’t feel a thing to women who report the insertion was painful. It’s recommended that it is inserted midway through your period because that’s when the cervix is most open.”
There is also a one per cent chance of puncturing the uterus, although previous reports of IUDs potentially causing inflammatory pelvic disease have been largely debunked.









Comments
Want to discuss? Please read our Commenting Policy first.