Up to 30 per cent of medical tests, treatments and procedures done in Canada are potentially unnecessary – and the excess is hurting both patients and the health system, a new report says.

The report, which was released Thursday by the Canadian Institute for Health Information (CIHI) and Choosing Wisely Canada, focused on eight types of tests and procedures that are commonly ordered by healthcare professionals and were found to be unnecessary and of no value to patients.
These needless tests and procedures, researchers say, are resulting in waste within the health system, as well as increased wait times and could potentially lead to patient harm.
READ MORE: Canada has some of the longest wait times to see doctors, specialists: report
“Many Canadians experience care that may be unnecessary,” David O’Toole, president and CEO of CIHI, says in a statement. “This report is another step toward ongoing standardization of measures and improved data to identify gaps, track improvements and ultimately improve the quality of — and access to — care for Canadians.”
According to the report, about one in four Canadians were recommended a test or treatment by a doctor that they felt was unnecessary. As well, 42 per cent of people surveyed say they expect a prescription or test when they visit the doctor.
However, 67 per cent of people also say they believe patient demand is what drives most unnecessary testing and treatments, not physicians.
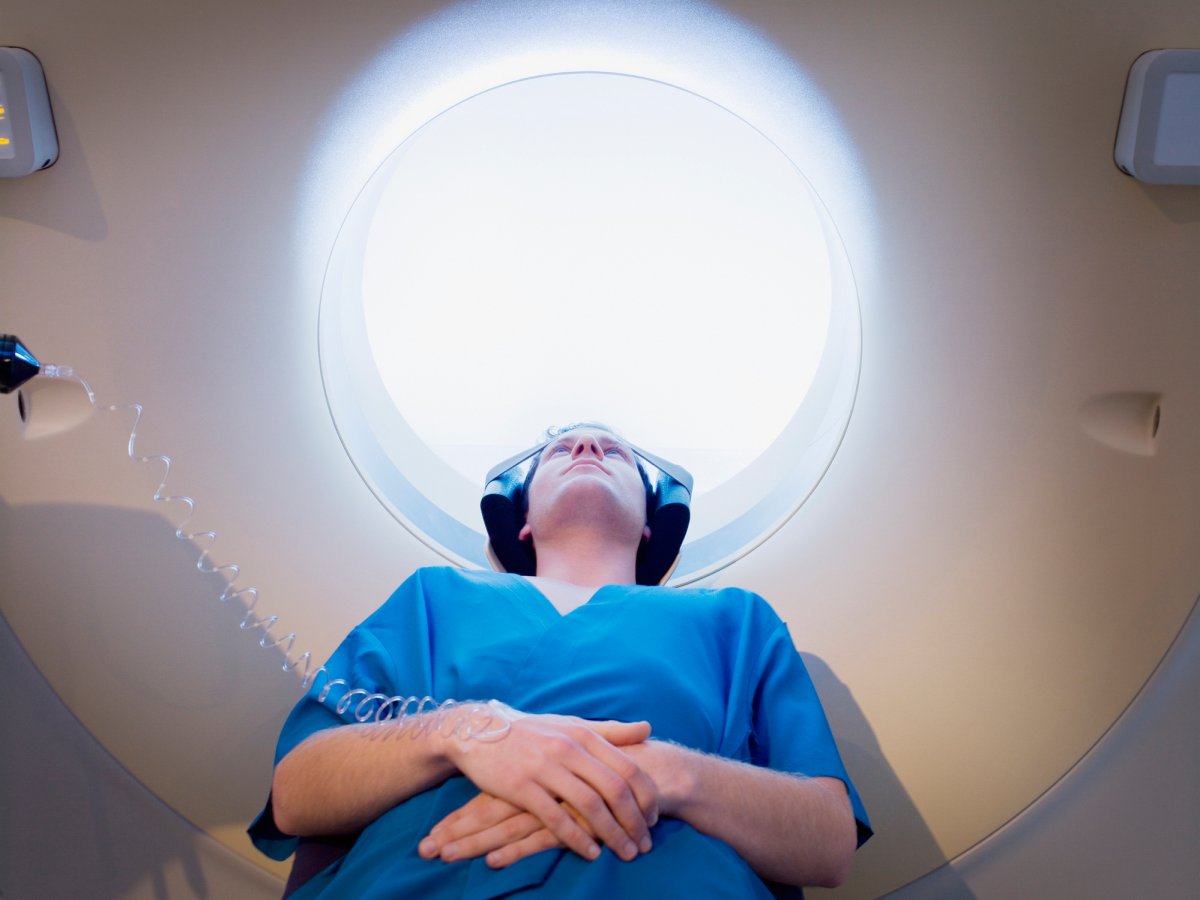
The report found that the most commonly unnecessary tests and treatments had to do with imaging testing (like X-rays and CT scans) for head traumas and cardiac patients, mammography, blood transfusions and drug treatments for insomnia. This pertained to primary, specialist and emergency care sectors.
As a result, researchers made a list of over 200 recommendations. Among them are:
1. Don’t do imaging for lower back pain unless red flags are present
The report found that 30 per cent of Alberta patients with lower back pain without red flags had at least one unnecessary X-ray, CT or MRI.
Researchers say that these types of scans are wasteful because they rarely show the cause of the pain and can actually cause harm to patients when there are no signs of seriously underlying conditions. This harm can include exposure to radiation and could lead to further unnecessary testing and surgery.
In fact, acute lower back pain typically goes away within four weeks — with or without imaging.

Get weekly health news
2. Don’t use atypical antipsychotics as a first-line intervention for insomnia in children and youth
Atypical antipsychotic drugs are generally used to treat psychiatric conditions like schizophrenia and autism.
However, researchers found that rates of low-dose quetiapine (which is often used to treat insomnia) increased in kids and young adults between the age of five and 25 in Manitoba, Saskatchewan and B.C., even though this is not recommended.
There is limited proof that atypical antipsychotics improve sleep, the report says, yet 36 per cent of child psychiatrists and developmental pediatricians had prescribed them between 2005 and 2006.
These types of medications often come with side effects like obesity, high blood sugar and high cholesterol.
3. Don’t use benzodiazepines and/or other sedative-hypnotics in older adults as the first choice for insomnia, agitation or delirium
Benzodiazepine is a sedative-hypnotic medication.
The report found that one in 10 seniors uses this medication on a regular basis, even though it is not recommended by experts.
Adults who use these types of medications are at an increased risk for motor vehicle accidents, hip fractures, daytime fatigue and falls.
Chronic use of benzodiazepines in particular are concerning because experts only recommend seniors take them for only two to four weeks.
4. Don’t routinely do screening mammography for average-risk women ages 40 to 49
Researchers say that screening for breast cancer among average-risk women ages 40 to 49 can potentially lead to more harm than good – yet 22 per cent of women in this category received a screening mammogram.
- Something’s fishy: 1 in 5 seafood products are mislabelled, study finds
- After controversial directive, Quebec now says anglophones have right to English health services
- Why non-alcoholic beer is gaining steam at Oktoberfest: ‘Nobody will judge you’
- Recall expands for Nutrabolics vegan bars over undeclared milk
To save one woman from dying of breast cancer, 2,100 average-risk women ages 40 to 49 would need to be screened every two years for 11 years. That could lead to 700 false-positives, 75 unnecessary biopsies and 10 unnecessary mastectomies or lumpectomies due to over-diagnosis.
5. Don’t routinely perform preoperative testing (such as chest X-rays, echocardiograms or cardiac stress tests) for patients undergoing low-risk surgeries. Don’t order a baseline electrocardiogram for asymptomatic patients undergoing low-risk non-cardiac surgery. Don’t perform stress cardiac imaging or advanced non-invasive imaging as a preoperative assessment in patients scheduled to undergo low-risk non-cardiac surgery
Between 18 and 35 per cent of patients in Ontario, Saskatchewan and Alberta who had a low-risk procedure also underwent preoperative testing.
READ MORE: 1 in 18 Canadian hospital patients experience harm from preventable errors: study
The report says these types of tests for low-risk surgeries do little to improve care and result in distressed patients and wasted resources. They may also expose patients to radiation, waste time, sometimes delay surgery and may result in false-positives, which can lead to further unnecessary testing and increased wait times.
6. Don’t do imaging for minor head trauma unless red flags are present / Don’t order CT head scans in adults and children who have suffered minor head injuries
According to researchers, 30 per cent of patients going through emergency departments in Ontario and Alberta with low-risk minor head trauma received a CT head scan.
The majority of patients with this type of head trauma often do not suffer serious brain injury. Such tests can expose patients to radiation exposure and can increase wait times for patients who do need CT scans.
7. Don’t routinely obtain head CT scans in hospitalized patients with delirium in absence of risk factors
In Ontario alone, 23 per cent of inpatients with delirium had a potentially unnecessary CT scan of their head.
Researchers say delirium is a sudden and severe change in brain function and can cause patients to appear confused or impact their ability to think clearly.
Delirium is a common problem among hospitalized patients and as much as 60 per cent of senior patients suffer from it while hospitalized.
This type of unnecessary testing can, again, expose patients to radiation, cause anxiety, and increase wait times to use the machine.
8. Don’t transfuse red blood cells for arbitrary hemoglobin or hematocrit thresholds in the absence of symptoms, active coronary disease, heart failure or stroke
Blood is a much-needed and costly resource. Doing such transfusions without red flags depletes the supply without improving patient outcomes, the report states.
These transfusions can cause reactions that range from mild to severe and include allergic reactions or anaphylaxis, acute hemolytic reactions, transfusion-associated circulatory overload and blood infections.







Comments