Health Canada wants ideas on how to stop risky prescribing of the drugs fuelling Canada’s fastest-growing addictions.

In a call for proposals published Friday, the federal government said it’s looking for suggestions on how to make prescribing safer, including better training and education for the health professionals giving out these powerful painkillers – badly needed by some but fatal for others.
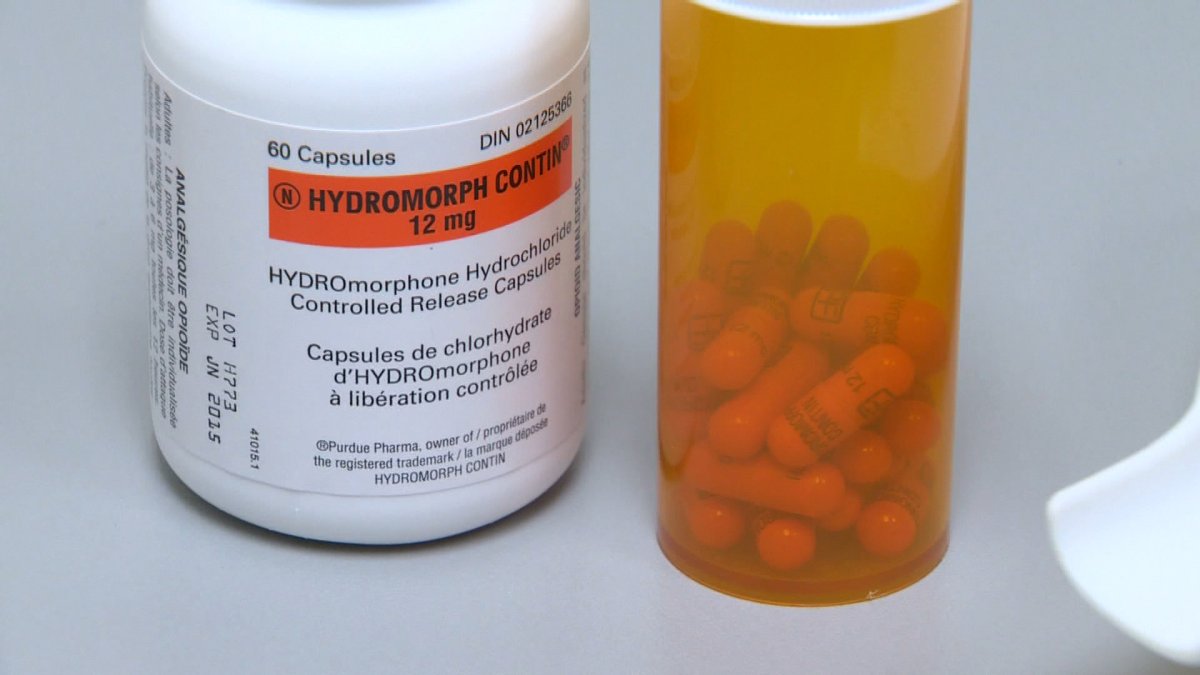
Global News analysis has found prescriptions for Hydromorph Contin, an opioid more potent, less regulated and more easily abused than OxyContin’s replacement, have skyrocketed in Ontario.
Publicly funded prescriptions increased from 25,600 in February, 2012 to 54,900 in June, 2014. All prescriptions – public and private – increased from 30,000 in May, 2012 to 66,000 in June, 2014.
At the same time, data from Ontario’s coroner indicates Hydromorph Contin’s active ingredient is killing more people each year.
The rise in Hydromorph Contin prescriptions worries health professionals on both sides of the border: In the United States, where hydromorphone’s considered the “champagne of opioids,” it’s far less easily available. Smuggled quantities of the pills south across the border from Canada would change that, they fear.
READ MORE: How pilfered Canadian pills are fuelling a U.S. health crisis
But Ontario has no plans to crack down on Purdue-made Hydromorph Contin in the same way the province made it tougher for physicians to prescribe OxyNEO.
READ MORE: Ontario has no plans to crack down on skyrocketing painkillers
Federal Health Minister Rona Ambrose has made prescription drug abuse a personal priority since her appointment last summer. Ottawa came under fire the year before, when it approved generic oxycodone for sale in Canada, even though health experts and provincial health ministers said it would put a cheap, addictive and easily abused drug on the market.
Ambrose already considering requiring other as-yet-unspecified drugs be “tamper-resistant,” making them harder to crush, snort and inject.
READ MORE: Health Minister considers requiring drugs be ‘tamper-resistant’
“But, requiring tamper-resistant formulations of drugs is only one component of the comprehensive approach required to effectively tackle prescription drug abuse,” her call for proposals reads. ”One area in particular that has been identified for improvement is prescriber practices. Improved prescriber education will support appropriate prescriber practices.”
The call for proposals is two-pronged: improving existing guidelines, training and tools for prescribing, and developing new ones.
“Do we need specialized and/or mandatory training for prescribers?” it asks.
The question’s been pondered before and it isn’t without controversy: Many pain advocates fear putting too many barriers up will just mean physicians avoid prescribing opioids altogether, and the people who genuinely need them don’t get them. Others argue these drugs are powerful and potentially dangerous enough to require special training.
The deadline to apply for the $3.6-million initiative is Aug. 29.




Comments