A British Columbia man is hoping to become the first person in Canada to receive a century-old experimental treatment known as phage therapy, which uses viruses to target antibiotic-resistant superbug bacterial infections.

Jeff Summerhayes, 57, lives on Vancouver Island and was born with cystic fibrosis, which causes his lungs to fill with mucus and creates a breeding ground for bacterial infections.
When he was 16 years old, Summerhayes became infected with a particularly resilient bacterial strain called Burkholderia cepacia. At the time, doctors didn’t expect him to survive past the age of 20.
“The infection has slowly ravaged my lungs over 30 years,” Summerhayes told Global News. “The only way that they’ve been able to treat the infection so far is with antibiotic therapy.”
But after receiving antibiotics on a regular basis for decades, his bacteria adapted and the treatment became ineffective.
“We were going through more and more drugs that the bacteria was becoming resistant to in a very short period of time,” Summerhayes said.
“That meant they were bombarding me with three or four different antibiotics at a time, and that was hard on my kidneys. The more I have to be on antibiotics, the less likely they are to work and the more damage they do to my other organs.”

In September 2018, Summerhayes’ lungs were on the verge of collapse, and he was forced to undergo a double lung transplant. His doctors have told him he now has a 50 per cent chance of surviving the next year.
In response, Summerhayes and his family began researching experimental treatments, and they came across some literature on phage therapy.
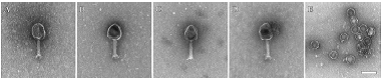
Bacteriophages, or phages for short, are viruses that have naturally evolved to attack only bacteria. They were discovered in 1917 by French-Canadian microbiologist Félix d’Hérelle, who found the phages could be used to fight bacterial infections in people. But following the discovery of penicillin in 1928, phage therapy was all but forgotten by western countries, including Canada.
“We’ve now come full circle,” said Dr. Jonathan Dennis, a microbiologist at the University of Alberta and Canada’s only phage therapy researcher.

Get weekly health news
“Bacteria have evolved to become resistant to these chemical antibiotics, and now we’re losing the advantage that we saw with those chemical antibiotics. We’re not keeping up with the problem and we’re heading towards a crisis.”
WATCH: How a Canadian doctor used phage therapy to save her husband from a superbug

Infectious disease experts have warned that our current overuse of antibiotics could result in 10 million deaths per year by 2050 due to antimicrobial resistance, making superbugs a bigger killer than cancer and making common procedures such as hip replacements and caesarean sections prohibitively risky.
Canadian infectious disease epidemiologist Steffanie Strathdee knows from personal experience how deadly superbugs have become. Strathdee and her American husband, Tom Patterson, are professors at the University of California San Diego. They were on a vacation to Egypt in 2015 when Patterson began feeling nauseous.
“Tom got very sick all of a sudden. We thought it was food poisoning, but he just kept throwing up,” Strathdee said.
Doctors eventually discovered that Patterson was infected with a superbug called Acinetobacter baumannii — a bacteria that was resistant to all antibiotics.
“I was really shocked because I’m trained as an infectious disease epidemiologist at the University of Toronto and I used to plate this bacteria on my Petri dishes in the 1980s,” Strathdee recalled.
“It seemed like a pretty wimpy bacteria back then. But over the next few decades, it has become a very nasty bacteria. It’s what I consider to be a ‘bacteria kleptomaniac’ — it steals these antibiotic resistance genes from other bacteria.”
Patterson’s condition quickly worsened, and he fell into a coma. His doctors said he didn’t have long to live.
“There was nothing that they could do. Little by little, day by day, he was slipping away. And he was going to die unless something drastic happened,” Strathdee said.
“It was also kind of the moment when I kicked myself into gear and decided that if the doctors had given up on him, I didn’t want to.”
In desperation, Strathdee began researching experimental treatments online and came across an article on phage therapy.
“I knew what phages were because, back in the 1980s, I studied virology at the University of Toronto, and my professor there taught us what bacteriophage were. It’s just that I didn’t ever know that they were used to treat people so I got really excited when I thought this might be something that could be used to save Tom,” Strathdee explained.
Strathdee proposed the idea to Patterson’s medical team in San Diego, who subsequently received special permission from the U.S. Food and Drug Administration (FDA) to attempt phage therapy under the terms of compassionate use, which is permitted when no other life-saving treatments are available.
Three days after Patterson was injected with a bacteriophage, he woke from his coma.
“He lifted his head off the pillow and he kissed his daughter’s hand. Everybody freaked out. It was just an incredible feeling,” Strathdee recalled. “I just couldn’t believe it. We all hoped that it was going to work, but it worked so quickly. I mean, here’s a guy who’s hours away, literally, from dying. And then he wakes up.”
Strathdee and her husband have since launched the Center for Innovative Phage Applications and Therapeutics (IPATH) at the UC San Diego School of Medicine, a non-profit that helps others with life-threatening bacterial infections to receive phage therapy.
“I represent evidence-based hope for people with these superbug infections. We’ve saved some lives already,” Patterson said.
IPATH has worked with patients in the U.S., and they’re now hoping to break new ground in Canada by asking Health Canada to allow Summerhayes, the double lung transplant recipient, to receive phage therapy in British Columbia. They’re currently looking for a bacteriophage virus that matches Summerhayes’ bacterial strain.
“It’s the last choice that I have,” Summerhayes said. “There’s nothing else available. We’re running out of antibiotics. If I can solve the bacteria problem and I get through the first year, I’ve been told there’s no reason why I can’t live another 10 years of good, healthy life.”
In a statement provided to Global News, a spokesperson for Health Canada said: “If a physician wants to use phage therapy to treat antimicrobial-resistant infections in a patient, a clinical trial application would need to be filed to Health Canada for review and approval. To date, Health Canada has not received any clinical trial applications for phage therapy.
“Health Canada may consider requests for access to drugs that are unavailable for sale in Canada under the Special Access Programme (SAP),” which considers whether experimental treatments may be used in cases where patients have serious or life-threatening conditions and when conventional treatments have failed or are unavailable.
LISTEN: Super Awesome Science Show recap — ‘phaging’ out the resistance
Strathdee has published a book about her husband’s ordeal, titled The Perfect Predator: A Scientist’s Race to Save Her Husband From a Deadly Superbug. She hopes her story will help to kick-start new research into the century-old treatment.
“Superbugs are a global crisis. This is not a problem that’s going away,” Strathdee said. “We need to step up to the plate. And Canada is well-poised to do that.”
WATCH: B.C. man challenging Health Canada for phage treatment














Comments
Want to discuss? Please read our Commenting Policy first.