WATCH ABOVE: When you call for an ambulance, you expect a quick response. But, several paramedics say a failed system is making patients wait. Kendra Slugoski reports.

EDMONTON – Desperate for change, paramedics and Emergency Medical Technicians (EMTs) are speaking out about their frustration on the front lines.
“I’ve had to explain to families why it took us a half hour, 45 minutes to get to their side when they’re crying for help,” says ‘Mike’ a rural EMT. Afraid of losing his job, Global News has agreed to protect his identity.
“When the odds are so significantly stacked against you, when you’re not protecting the community you chose to work in because you’re somewhere else and tragedy strikes, you begin to lose hope,” Mike writes in a blog post.
READ MORE: Code Red – A blog from one ‘utterly frustrated EMT’
Alberta Health Services took over the ambulance fleet in 2009 and developed a borderless system. It allows dispatch to pull ambulances and their crews outside of the city into the metro areas.
“We often refer to Edmonton as the vortex. Once you’re in, good luck getting out.”
Mike says he is often dispatched to drive patients to Edmonton for non-emergency transfers. Once in the hospital, he must stay with that patient until a bed is available. Many of his days are spent sitting and waiting.
Mike has also been called to different counties because their ambulance crews are tied up in the city.
“So now you’re getting these holes in the province where there’s no EMS coverage whatsoever. On multiple occasions, I’ve been the only ambulance available in a 100 kilometre radius.”
READ MORE: Code Red Part 1 – Paramedics warn of lengthening response times
In 2012, 11 paramedics put their livelihoods on the line and spoke to Global News about long waits in hospital emergency rooms, as well as a lack of ambulances on the road.
Our award-winning Code Red series prompted the health minister to promise more resources and more paramedics.

Get weekly health news
Three years later, many other paramedics say nothing has changed.
One of those paramedics is a 40-year veteran. George Porter now works in southern Alberta, but has spent time in cities and towns across the province.
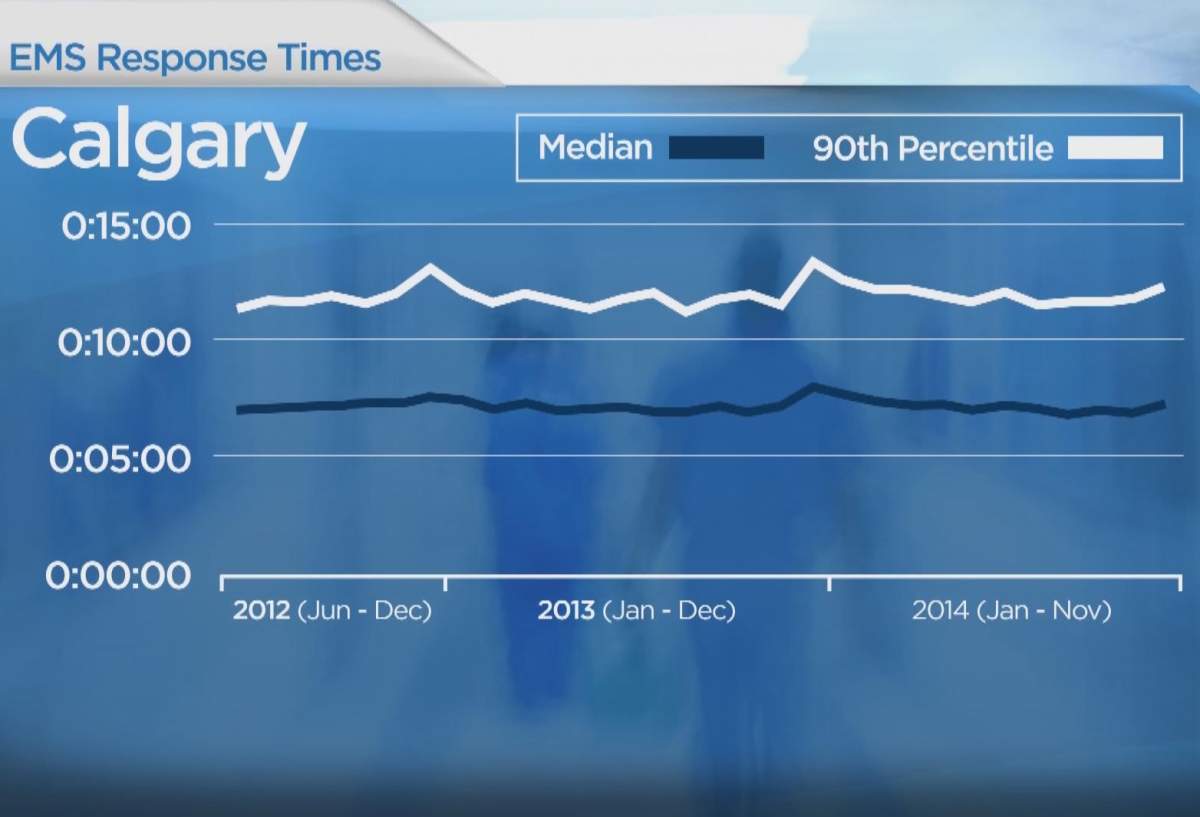
AHS does not have response time benchmarks, but Chief Paramedic Darren Sandbeck says times have remained consistent.
“I challenge that,” says Porter, who explains he has expressed concern to management and a previous Health Minister. Porter says rural crews are constantly being called for inter-facility transfers and are basically being treated like taxi drivers.
“A huge percentage of the transfers we’re doing don’t need to be in an ambulance. They need a ride.”
But Alberta’s top paramedic says it comes down to geography.
Sandbeck says Alberta is a big province and an ambulance can’t be everywhere quickly. AHS maintains the borderless system is a better use of resources.
“I believe every Albertan would like to know they’re going to get the closest ambulance and that’s what our deployment model does.”
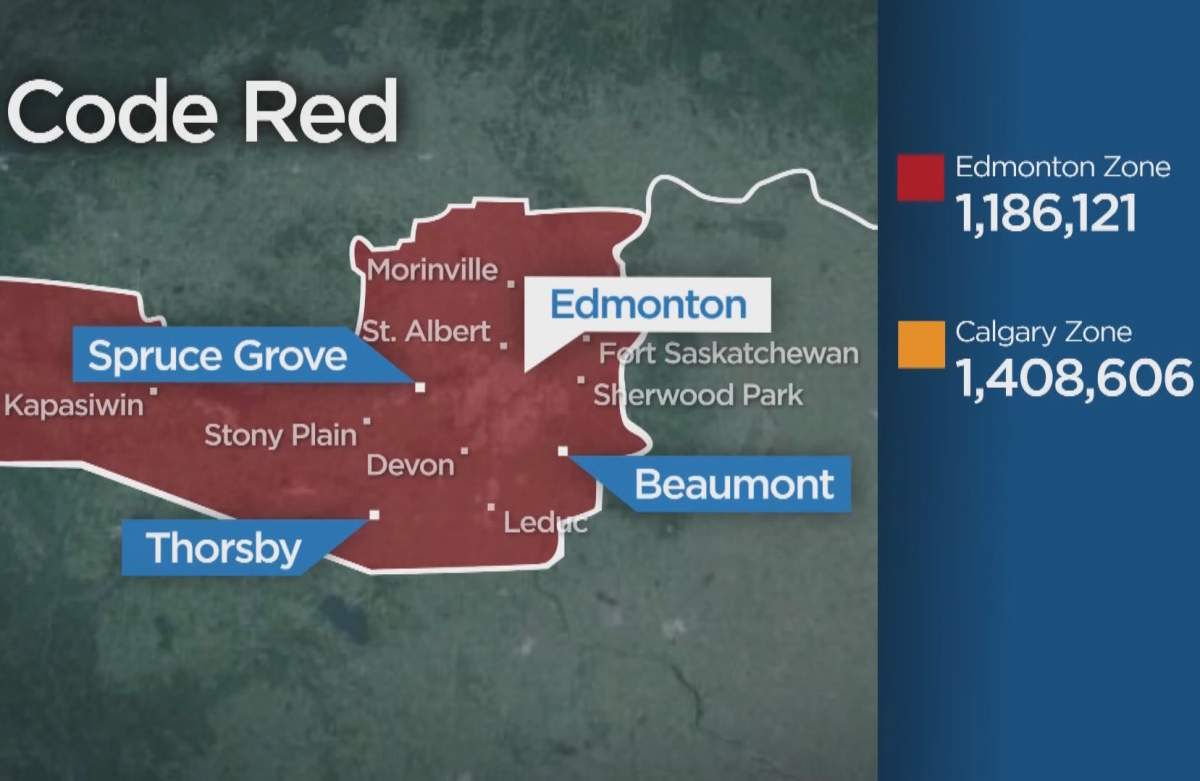
GRAPHIC: The maps below Alberta Health Services’ zones and the regions and the populations of those regions (as of 2011 AHS records).
Paramedics and EMTs say once they arrive in big city hospitals, they are waiting hours to release a patient.
According to one Edmonton paramedic, it’s not unusual to spend an entire shift in the emergency room and sometimes staff even trade off.
“They take over patient care there, they’re stuck there their entire shift and another paramedic relieves them.”
A Calgary paramedic says patients should also be alarmed.
“They should be absolutely concerned — people in the metro areas, people in the big cities for sure. Their hospitals are back-logged, ambulances are not available.”
AHS says it has tried to reduce hospital times for EMS crews, but says it hasn’t had a lot of success. A pilot project was launched at two Edmonton hospitals to free up space in emergency rooms, and allow ambulance crews to get back on the road.
READ MORE: AHS pilot project aims to cut ER wait times, get more ambulances on the road
Porter says the solution is simple: non-emergency transfers should not take priority over emergency coverage.
“I don’t get it. I haven’t got it from day one and I still don’t get it, why we’re in this situation five years after the fact.”













Comments
Want to discuss? Please read our Commenting Policy first.