TORONTO – A Montreal hospital has been battling for the last year to extinguish an outbreak with a worrisome and highly drug-resistant bacteria.

The outbreak at the Jewish General is the first in Canada caused by this strain of the bacteria, a bug that has sparked serious concern because of how easily it spreads and its ability to transfer resistance to other bacteria.
A report on the outbreak was presented in Chicago on Sunday to the Interscience Conference on Antimicrobial Agents and Chemotherapy, a major annual gathering of infectious diseases specialists.
Dr. Mark Miller, head of infection control at the Jewish General, said the outbreak has been brought under control, but a few patients with the bacteria are still being treated in the hospital.
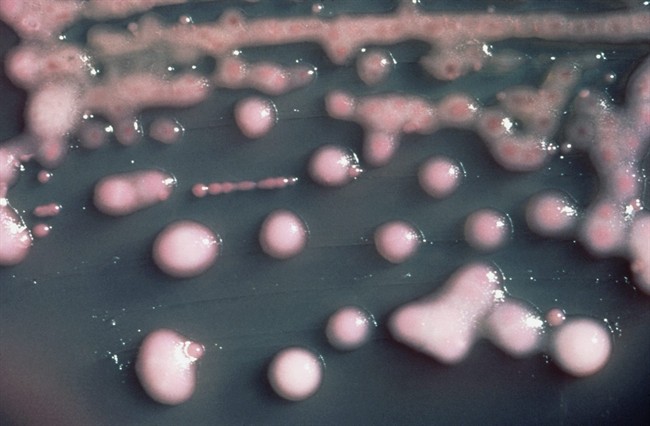
The outbreak was caused by Klebsiella pneumoniae, which is normally found in the human intestine. In healthy people, these bacteria can live in the intestine without causing illness. In hospitals, however, they can cause a range of infections, including pneumonia, bloodstream infections and urinary tract infections.
Klebsiella pneumoniae traditionally have been treated with antibiotics called carbepenems. But in the last decade or so, a strain of the bacteria has developed that is resistant to this class of drugs. To make matters worse, the genetic component that gives Klebsiella pneumoniae this resistance has the capacity to transfer into other bacteria, making them resistant to these drugs as well.
The strain with this component is called KPC-producing Klebsiella pneumoniae, and it has even more tricks in its arsenal. The gene that makes it resistant to carbepenems is packaged in a cassette of genes that confer resistance to a number of other antibiotics.
- Michael Kovrig reflects on ‘brutally hard’ Chinese detention: ‘You’re totally alone’
- TD Bank moves to seize home of Russian-Canadian jailed for smuggling tech to Kremlin
- U.S. moves to ban Chinese software, hardware from all vehicles in America
- Conservatives set to table non-confidence motion Tuesday. What to expect
Miller said the version that slipped into his hospital could only be treated with two antibiotics – an old drug with serious side-effects and a newer drug. He and others worry about the day they will find KPC that responds to no drugs at all.

Get daily National news
That has happened. In fact, the Ottawa Hospital had three cases of KPC-producing Klebsiella pneumoniae in 2008, one of which was resistant to all antibiotics.
Microbiologist Marc Desjardins said the Ottawa Hospital was lucky – the three cases didn’t spark an outbreak. (One patient caught the bacteria from one of the other two, but there was no sustained spread in the hospital.) But the patients were hard to treat and for one, nothing worked.
“The bug was resistant to everything. There was absolutely not a single antibiotic we could give that patient,” Desjardins said. The woman, who had other grave health problems, eventually died.
Battling bacteria that are not susceptible to any antibiotics is a nightmare scenario, he admitted.
“At least in serious infections, there is hope to actually treat the infection. With KPCs, if your organism is resistant to everything, we currently in our baggage of antibiotics have nothing available to treat them,” Desjardins said.
“The only thing to do is to use combinations (of antibiotics) and hope.”
KPC was first spotted in North Carolina in 1998. Since then, bacteria with this factor have spread widely. Hospitals in Israel and Greece have battled the problem. In the United States, New York state has experienced a lot of KPC outbreaks.
Canada first started to look for KPC in 2009, said Dr. Michael Mulvey, head of the division of antimicrobial resistance and nosocomial (hospital-acquired) infections at the Public Health Agency of Canada. Since then, surveillance has spotted 80 cases, a figure Mulvey thinks is probably an underestimate.
Most have been isolated cases, though another Quebec hospital has battled an outbreak, Mulvey said. He would not disclose the location or the name of the facility.
“The risk to Canadians right now is very low,” Mulvey insisted.
“But in the hospitals, we’re always concerned about antimicrobial resistance, especially in the very ill patients that are immunocompromised. And the fact that these are multi-drug resistant and the odd one is now pan-resistant, it certainly is a concern in the hospitals.”
At the Jewish General, the first KPC case was discovered in August of last year. Since then, 27 patients have tested positive for it. Some died, though Miller said it was a judgment call as to whether the bacteria caused their deaths or merely contributed to their decline. He would not say how many KPC patients had died.
“We’ve been truly impressed,” Miller said of the bacteria’s ability to spread from person to person and the facility with which it shares its resistance capabilities with other bacteria in its general class.
His laboratory spotted the resistance cassette in other bacteria isolated from patients in the hospital, including Serratia and Enterobacter.
Another concerning feature of KPC-producing Klebsiella pneumoniae is the rate at which it causes illness. With any hospital-acquired bacteria, a portion of people who pick it up won’t develop an infection. They are said to be “colonized.”
With some hospital bugs, there might be 150 carriers for every person who actually develops an infection from it. But with this bacteria, the ratio is more like one infection for every 10 people colonized, Miller said.
Another problem: It takes months for people carrying the KPC-strain to “clear” it from their systems. That can be a concern if someone carrying it is released from hospital and goes home to an elderly spouse, or one with a chronic illness.
Getting the Jewish General’s outbreak under control took Herculean efforts. The normal approaches to outbreaks of hospital infections – isolating colonized patients and requiring anyone going into their rooms to don gloves and gowns – didn’t work.
Miller said his hospital eventually had to open a dedicated KPC ward to house all the patients. Staff taking care of those patients were not allowed to work elsewhere in the hospital. The ward was a drain on resources and expensive to operate, but there was no alternative, he suggested.
Desjardins agreed.
“Bringing these outbreaks with KPCs under control is a fairly difficult thing to do and you need more aggressive measures to do that than just telling people to wash their hands and to put the patient under isolation.”






Comments