When Andrea Carter started working on the HIV file a decade ago, she couldn’t have predicted the progress being made today.

“Honestly, I can say five years ago I don’t think we would have seen this or I wouldn’t have imagined that we would have been here,” said the director of programs for HIV Community Link, looking back on the what she describes as momentum gained in dealing with the virus over the course of 2017.
“I think it’s a really exciting time in HIV with all of these new advancements.”
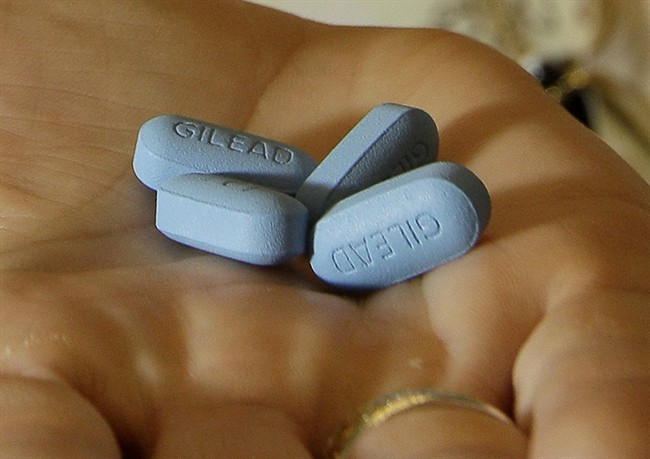
Earlier this year, three generic versions of the drug Truvada (also known as PrEP – or pre-exposure prophylaxis) came to market, significantly reducing the cost for the one-a-day pill which is proven to be up to 99 per cent effective in preventing the transmission of HIV.
WATCH BELOW: How the fear of HIV has changed over time

READ MORE: HIV prevention drug Truvada difficult for some to access in Alberta
In Ontario, the generics were added to the public health plan in September. In Alberta, there is still no provincially-funded coverage for the drug when it is prescribed as a preventative treatment.
“In Toronto, they’ve just announced there is a decrease for the first time in many years– a significant decrease– in new HIV cases,” Carter said. “I think to some degree that can be attributed to the availability and affordability of PrEP in Ontario.”
Carter would like to see the Alberta government add PrEP to the provincial drug program in the new year and points to a number of indicators, which lead her to be optimistic.
“Over the past year, Alberta Health and Alberta Health Services have been working on developing a new strategy for sexually transmitted and blood-borne infections, including HIV,” she said.
Among the recommendations made from the work is a mission to increase access to PrEP across Alberta, something a working group will now look at how to implement.
READ MORE: B.C. assesses Truvada, an HIV prevention drug that looks ‘very promising’
Carter also believes new clinical guidelines for PrEP from the Canadian Institute of Health Research will increase information and awareness surrounding the drug, not only for potential patients but for health providers – some of whom aren’t as well versed on the treatment.
“I think this is going to make a big change.”
Finally, Carter said efforts to remove the stigma surrounding HIV have allowed for more open conversations, specifically around the topic of patients who are positive but undetectable because they’re taking an effective treatment for the virus.
“We’re really at a tipping point in HIV and there’s potentially a light at the end of the tunnel for addressing the HIV epidemic, with all these sorts of movements and biomedical technologies we have at hand,” Carter said looking ahead to the new year.
“I think PrEP is a key piece of this. Now is a really critical time for there to be some movement on this. If not, then I think we’re missing an opportunity.”





Comments